Thank you for visiting nature.com. You are using a browser version with limited support for CSS. To obtain the best experience, we recommend you use a more up to date browser (or turn off compatibility mode in Internet Explorer). In the meantime, to ensure continued support, we are displaying the site without styles and JavaScript.
- View all journals
- Explore content
- About the journal
- Publish with us
- Sign up for alerts
- Review Article
- Open access
- Published: 31 January 2024

A decade of love: mapping the landscape of romantic love research through bibliometric analysis
- Yixue Han 1 ,
- Yulin Luo 1 ,
- Zhuohong Chen 1 ,
- Nan Gao 1 ,
- Yangyang Song 1 &
- Shen Liu 1
Humanities and Social Sciences Communications volume 11 , Article number: 187 ( 2024 ) Cite this article
4082 Accesses
1 Citations
23 Altmetric
Metrics details
Given the limited availability of bibliometric and visual analysis on the topic of romantic love, the primary objective of the current study is to fill this gap by conducting a comprehensive visual analysis of relevant literature. Through this analysis, the current study aimed to uncover current research trends and identify potential future directions in the field of romantic love. The current study’s search criteria were met by an impressive 6858 publications found in the Web of Science database for the period between 2013 and 2022. A thorough analysis was conducted on the bibliographic visualization of the authors, organizations, countries, references, and keywords. Over time, there has been a remarkable surge in the number of significant publications. Among the authors in the field of romantic love, Emily A. Impett has emerged as the most prolific. The Journal of Social and Personal Relationships is indeed one of the top journals that has published a significant number of articles on the topic of romantic love. During the preceding decade, the University of California System emerged as a prominent producer of publications centered around romantic love, solidifying the United States’ position as a dominant player in this field. In recent times, there has been a significant surge in the popularity of keywords such as “same-sex,” “conflict resolution,” and “social relationships” within academic literature. These topics have experienced a burst of attention, as evidenced by a substantial increase in references and citations. Through the use of visualization maps and analysis of key publications, the current study offers a comprehensive overview of the key concepts and potential avenues for future research in the field of romantic love. Gaining a deep understanding of the complex dynamics and societal implications of romantic love has been instrumental in formulating policies that embody increased compassion and support. As a result, these policies have played a pivotal role in fostering resilient familial ties and contributing to the enduring stability and prosperity of our social fabric.
Similar content being viewed by others
Who reads contemporary erotic novels and why?
The cultural evolution of love in literary history

Meanings and implications of love: review of the scholarship of love with a sub-Saharan focus
Introduction, the development course of romantic love.
Romantic love, as defined by Hatfield and Rapson ( 1987 ) as an intense longing for union with another, has long been recognized as a driving force behind some of humanity’s most remarkable achievements. Studies by Bartels and Zeki ( 2000 ) and the work of Fehr ( 2013 , 2015 ) have further emphasized its profound impact. Previous research has suggested that romantic love has a crucial role in the development and maintenance of romantic relationships. It involves a transition from the significant investment of time and attention in the initial stages to enhanced communication and satisfaction in committed partnerships (Mizrahi et al. 2022 ). However, recent research has shown that in the United States, the divorce rate has consistently remained at historically high levels. According to the Centers for Disease Control and Prevention ( 2017 ), ~40–50% of first marriages end in divorce. In recent times, there has been a trend toward shorter and more prevalent romantic relationships. Alirezanejad ( 2022 ) found that different generations of women have maintained distinct expectations and experiences when it comes to love. Additionally, the significance of commitment in romantic relationships has witnessed a decline. These findings also indicate that there are additional factors at play that influence the dynamics between romantic love and the duration of relationships. The triangular theory of love, being one of the most widely used theories on romantic love, proposes that romantic love consists of three components: intimacy, passion, and an absence of commitment, alongside a willingness to invest resources without expecting reciprocation (Jimenez-Picon et al. 2022 ). The Love Attitude Scale (LAS) developed by Clyde and Susan Hendrick has been a significant contribution in the study of romantic love using psychometric methods. Tobore ( 2020 ) introduced a comprehensive four-fold framework that aims to elucidate the dynamics of how love evolves and diminishes. This framework includes the elements of attraction, empathy or connection, trust, and respect. As a result, the enigmatic and unique nature of romantic love has captivated the attention of scholars from various disciplines, including psychology, biology, sociology, and neuroscience. These scholars have conducted extensive research and investigations into the complexities of romantic love. Thus, the present study conducted a comprehensive and in-depth analysis and discourse on romantic love, spanning multiple research domains. Additionally, the publication emphasized the influence of romantic love on positive emotions as well as its association with various negative behaviors. Furthermore, it underscored the importance of utilizing bibliometric analysis as a valuable approach to study and understand romantic love.
The research directions of romantic love in different disciplines
Psychologists have focused on exploring the relationship between romantic love and negative emotions in individuals with mental illnesses. Lafontaine et al. ( 2020 ) found a correlation between romantic love insecurity, specifically anxiety and avoidance, and the occurrence of intimate partner violence (IPV). This pattern of behavior was shown to undermine relationships and diminish individuals’ sense of security. Moreover, individuals with schizophrenia and other mental health conditions faced significant challenges in building and sustaining healthy interpersonal connections, partly due to the enduring stigma associated with mental illness (Budziszewska et al. 2020 ). Biological researchers have delved into the physiological activities and responses associated with romantic love. Furthermore, biological research has demonstrated that communication plays a crucial role in enhancing romantic relationships by facilitating physiological and behavioral adaptations between partners. For instance, a study by Zeevi et al. ( 2022 ) revealed that men and women in a romantic relationship can enhance their romantic interest in each other by synchronizing their skin electrical activities and modifying their behavior. These findings suggest that the social adaptation of the sympathetic nervous system and motor behavior play a critical role in the romantic attraction between partners. Furthermore, recent biological research conducted by Kerr et al. ( 2022 ) has discovered a correlation between unsuitable adult attachment in romantic relationships and the interpersonal circumplex, which is a component of personality pathology. Furthermore, a sociological study on pair-bonding conducted by Fletcher et al. ( 2015 ) highlighted that romantic love is intricately linked to the evolution and survival of Homo sapiens, making it a biologically significant function with profound evolutionary implications. Neuroscientists have examined the activation of different brain regions that are triggered by romantic love activities. Functional magnetic resonance imaging (fMRI) has emerged as a prominent technique for studying the neurobiological basis of love. Researchers such as Acevedo et al. ( 2020 ) and Chester et al. ( 2021 ) have utilized fMRI to investigate the neural correlates of romantic love and gain insights into the brain mechanisms underlying this complex phenomenon. Neuroscientists have identified specific brain regions associated with love, including the insula and anterior cingulate cortex. These regions are involved in the processing of emotional experiences related to valued objects. A study by Bartels and Zeki ( 2000 ) highlighted the involvement of these brain regions in the experience of romantic love, shedding light on the neural mechanisms underlying the emotional aspects of love. The activation of reward-related areas in the brain, particularly those rich in oxytocin, has been observed in individuals experiencing love. Studies by Acevedo et al. ( 2012 ) and Bartels and Zeki ( 2004 ) have shown that regions associated with reward processing, such as the ventral tegmental area and nucleus accumbens, are involved in the experience of romantic love. Indeed, the involvement of the reward system in love has surpassed expectations. During the initial stages of romantic love, research conducted by Fisher et al. ( 2010 ) has shown that reward-related brain regions, including the bilateral ventral tegmental areas, are activated more strongly compared to the later stages of passion.
The social impact of romantic love
Undoubtedly, falling in love has a profound impact on people’s daily lives, as highlighted by research conducted by Quintard et al. ( 2021 ). Falling in love has been associated with enhanced well-being and has been correlated with fervor, activity, pleasure, and other positive emotions, as noted in research conducted by Langeslag ( 2022 ). However, it is important to acknowledge that the pitfalls of romantic love are often overlooked. Research, such as that conducted by Lonergan et al. ( 2022 ), has found associations between romantic love and criminal activity as well as psychological disorders. Additionally, studies by Aron et al. ( 2005 ), Merritt et al. ( 2022 ) and Li et al. ( 2022 ) have highlighted the presence of unpleasant affective states such as hyperarousal, anxiety, and depression in the context of romantic love. In recent decades, romantic love has undergone significant transformations that have had a substantial impact on both personal and societal life, as emphasized by research conducted by Reis et al. ( 2013 ).
The necessity of bibliometric analysis
Bibliometrics is a field that encompasses the quantitative study of documents, aiming to provide researchers with insights into academic, technological, and scientific advancements (William and Concepción 2001 ). The methodology utilized a range of techniques, including author analysis, concept mapping, clustering, factor analysis, and citation analysis, to investigate historical data and assist scholars in identifying significant trends and emerging directions within their disciplines (Daim et al. 2006 ; Hou et al. 2022 ). The term “bibliometrics” was coined by the distinguished British scientist Allen Richard in 1969, replacing the previously employed term “statistical bibliography.” In recent years, there has been a surging interest in this approach, with a growing number of researchers incorporating it into their work. Bibliometric analysis has been employed in various research domains, including the study of romantic love. These analyses offer valuable insights into the research areas that have been investigated, as well as potential future trends, challenges, and opportunities in the field. To the best of our knowledge, there have been limited previous publications that have specifically analyzed romantic love based on the triangular theory of love development and explored the concept across different disciplines.
In the current study, we utilized state-of-the-art analytical tools, including CiteSpace (6.2.R2), VOSviewer (1.6.18), Microsoft Excel (2019), and Scimago Graphica (1.0.26), in conjunction with the most recent data obtained from the Web of Science (WOS) core collection database. These tools allowed us to conduct a comprehensive bibliometric and visual analysis of publications related to romantic love published in the last decade. By employing these cutting-edge tools and leveraging the extensive data available from WOS, we aimed to gain valuable insights into the research landscape surrounding romantic love during this specific time frame. Our study aimed to achieve several objectives. First, we sought to identify the current research hotspots and trends within the field of romantic love. Second, we aimed to conduct an in-depth examination of visual maps and seminal articles, providing a comprehensive overview of the literature.
Material and methods
Data acquisition and search strategy.
The Web of Science (WOS) platform served as a valuable resource, containing a vast collection of over 9000 significant academic articles. This database stands as one of the oldest and most comprehensive citation index records, encompassing a wide range of disciplines, including social science, engineering technology, biomedicine, arts and humanities, and various other subjects. Since its establishment in 1900, the Web of Science (WOS) has served as a cornerstone of scholarly research and has wielded significant influence within academic circles (Ellegaard and Wallin 2015 ). The quantitative analysis feature of the platform facilitated the acquisition of various types of information related to scholarly publications. This included data on the annual number of papers published, papers published by state or region, popular journals within specific disciplines, frequently utilized publishing houses, and highly downloaded and cited literature. Indeed, references that receive multiple citations play a crucial role in providing a robust foundation for the study of romantic love, as emphasized by Xu et al. ( 2022 ).
The subject matter of romantic love and its interrelation with romantic relationships has a profound impact on the satisfaction and longevity of love between individuals, as highlighted by Zagefka ( 2022 ). Passionate love is a fundamental concept within romantic relationships, as emphasized by Mizrahi et al. ( 2022 ). Sternberg’s triangular theory of love stands as one of the most substantial and frequently referenced frameworks for understanding love, as noted by Sorokowski et al. ( 2021 ). To comprehensively explore the topic, the search strategy incorporated the inclusion of the following elements: The topic could encompass “romantic love,” OR “passionate love,” OR “romantic relationship,” OR “triangular theory of love.”‘ The search was conducted within the Web of Science Core Collection database, which covers the time period from 2013 to 2022. The database indexes the Science Citation Index Expanded (SCI-EXPANDED) and Social Science Citation Index-Expanded (SSCI-EXPANDED). The search was limited to publications written in the English language. To refine the search and focus on specific types of publications, certain categories were excluded from the search results. These excluded categories included early access, book chapters, proceeding papers, data papers, and retracted publications. By excluding these categories, the search aimed to prioritize reviews and articles, which are typically considered primary sources of scholarly information. As a result of these refined search criteria, a total of 6858 relevant items were identified and included in the analysis.
The retrieval strategy employed in this research was designed to maintain the integrity and impartiality of the search process (see Fig. 1 ).
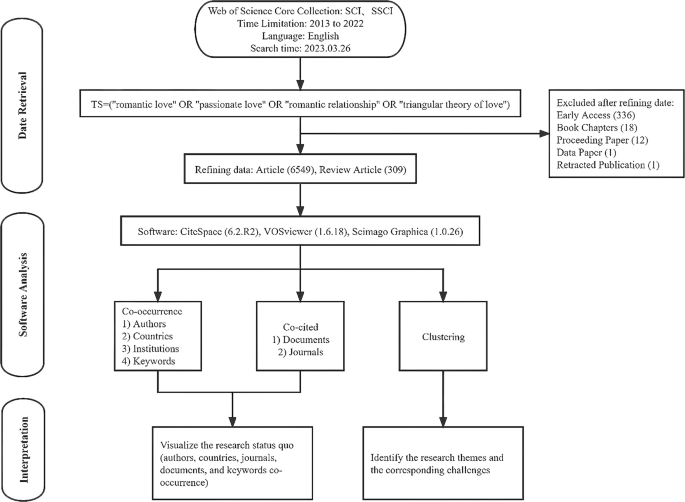
To ensure that the search results were not influenced by daily database updates, all searches were conducted on a single day, specifically on March 26, 2023.
Analysis tool
For bibliometric analysis, the current study utilized a powerful combination of CiteSpace (6.2.R2), VOSviewer (1.6.18), Microsoft Excel (2019), and Scimago Graphica (1.0.26). These state-of-the-art software tools seamlessly integrated insights from scientometrics, information science, computer science, and other related fields to generate highly intuitive and informative visual maps. These maps revealed the development trajectory and structural underpinnings of scientific research. Indeed, each of these four software applications held unique and irreplaceable significance, excelling in specific domains of bibliometric analysis. Excel, for instance, demonstrated unparalleled proficiency in the intuitive transformation of charts. CiteSpace specialized in the clustering of topics and the delineation of the spatio-temporal background of words. VOSviewer played a pivotal role in both displaying and analyzing keywords, leveraging its distinctive capabilities. Lastly, Scimago Graphica contributed significantly to the geographical perspective of statistical analysis, offering insights that were unmatched in their comprehensiveness. Collectively, these tools not only proved indispensable but also brought their individual strengths to the forefront, contributing uniquely to the overall analytical landscape. Indeed, the Excel program was commonly employed to comprehensively analyze key data points such as the number of published papers, frequency of citations, and matched published documents. It was also employed to synthesize all the information for creating intuitive visual representations (Fig. 2 ) to illustrate the trends in the number of publications, citations, and their corresponding fitting functions during different periods. The use of CiteSpace in the current study was focused on highlighting the most salient occurrence burst on a timeline map and detecting the centrality of romantic love studies (Zhang et al. 2022a ). In order to attain a comprehensive understanding of the progress in romantic love research, an evolutionary analysis was undertaken, utilizing CiteSpace’s burst function. Co-occurrence analysis on pertinent keywords is another valuable method used to gain insights into the relationships and patterns among keywords in a specific research domain. Indeed, the analyses conducted, including the evolutionary analysis and co-occurrence analysis, facilitated an examination of the prevailing themes and trends of romantic love across different generations from a chronological perspective. VOSviewer, a powerful visualization tool, was utilized in the current study to portray the borders of romantic love with varying color clusters. It also facilitated the exploration of the co-occurrence of authors, institutions, and keywords associated with romantic love. The circles of various colors and sizes were used to represent the occurrence frequency of distinct cluster words and different keywords, respectively. The examination of keywords in the current study, augmented by chart analysis, delved into a more profound, comprehensive, and scientific level. Scimago Graphica 1.0.18, a tool designed for visualizing international collaboration, proved highly effective in the current study for facilitating the visualization of international collaboration (He et al. 2022 ). By organically combining the atlas and the world map, researchers were able to intuitively observe differences in the number of publications across various countries and the extent of national collaboration between different regions.
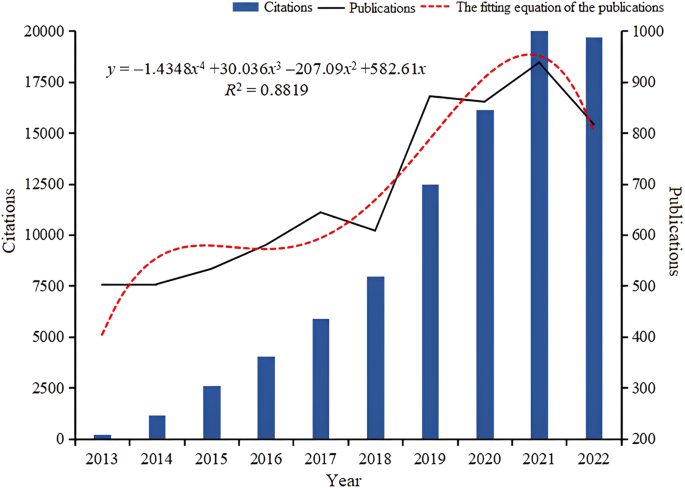
The trend exhibited an upward trajectory, with an estimated 938 publications in 2021, compared to 502 publications in 2013. Notably, the annual publication volume in the field of romantic love had reached its peak in 2021, as indicated by the fitted equation. However, it is worth mentioning that there was a slight decrease in publication numbers during specific periods. From 2017 to 2018, the annual publication count declined from 644 to 608. Similarly, from 2019 to 2020, there was a minor decrease from 872 to 861 publications annually. Additionally, there was a slight decline from 2021 to 2022, with the number of publications decreasing from 938 to 817 annually.
In the previous study, a comprehensive range of factors was considered to provide a thorough and scientifically rigorous atlas analysis of romantic love research. These factors included the annual publication rate, citation counts, H-index, impact factor, centrality, and occurrence/citation burst. An increase in the volume of publications can indicate the growth of a field and provide insights into future research directions (Wang 2016 ). While the number of citations a paper receives may not directly measure an author’s academic influence, it can indicate the recognition of the author’s work by peers worldwide. The “H-index” was a tool for evaluating academic influence, where a researcher with an “H-index” of 10 had 10 papers that had been cited at least 10 times (Wang et al. 2021 ). Since its inception in the 1950s, the impact factor has been widely regarded as a prominent index for ranking scientific literature. It has become an emblem of the prestige and significance of journals and authors in determining the relevance of a journal (Oosthuizen and Fenton 2014 ). For the current study, Journal Citation Reports (JCR) were utilized to calculate impact factors (2021). The centrality of research objects can indeed reflect their impact on the entire field, with greater centrality indicating a greater representation of homologous study content within a subject area. In the study conducted by Gao et al. ( 2021 ), betweenness centrality scores were adjusted to the range of [0, 1]. Specifically, if the betweenness centrality score of a main keyword exceeded 0.10, it was considered to indicate the significance of the study target. In the study conducted by Xu et al. ( 2022 ), the concept of a “burst term” was utilized to refer to an unexpected term that emerged in the research, potentially indicating new directions or orientations discovered during the investigation. The Kleinberg burst detection method, which is implemented in the CiteSpace software, was employed to identify these burst terms and highlight them as indicators of frontier research.
Publication outputs
A total of 6858 records met the search criteria. As depicted in Fig. 2 , the number of annual publications in the field of romantic love has shown a consistent upward trend since 2013. This increase is accompanied by a corresponding surge in citation counts, as indicated by the fitted equation. Citation counts in the field of romantic love have also experienced a significant upsurge since 2013, with an approximate 90-fold increase by 2022. Furthermore, based on current trends and fitting curves, the number of studies in this field is expected to continue rising, with an increasing number of researchers focusing on this topic.
Distribution by journals
The current study retrieved a total of 6858 records from 1251 journals, with ~33.79% of the material published by 20 publications that released more than 50 papers in this field. The top ten journals, accounting for 23.78% (92–400) of all papers published, had an average publication count of 134 papers per journal (see Table 1 ). Among them, the Journal of Social and Personal Relationships (400 publications, IF 2021 = 2.681) had the highest number of papers on romantic love research, followed by Personal Relationships (189 publications, IF 2021 = 1.528), and Personality and Individual Differences (185 publications, IF 2021 = 3.950). Notably, the Journal of Personality and Social Psychology was the most influential professional core journal in this field, boasting the highest impact factor (8.460). Both European and American journals have made significant contributions to this field, with the United States and the United Kingdom accounting for 40% and 50% of the top 10 journal publishing countries/regions, respectively. The impact factors of the top 10 most-published journals ranged from 1.528 to 8.460, with an average of 4.070. It is worth noting that publishing romantic love-related articles in high-impact journals remains challenging.
Distribution by authors and research areas
A staggering 15,088 authors contributed to the total number of papers. In Fig. 3 , the collaborative efforts of the writers were illustrated through a network map, where the connections between the nodes signified their collaborative affiliations. Among the top three clusters, the red cluster included authors Joseph P. Allen, Martine Hebert, and Marie-France Lafontaine, who had converged due to their shared research interests in adolescent dating violence and aggression (Cenat et al. 2022 ; Niolon et al. 2015 ). The blue cluster consisted of authors Frank D. Fincham, James K. Monk, and Ashley K. Randall, who had explored the interplay between relationship satisfaction, stress, and relationship maintenance in romantic relationships (Randall and Bodenmann 2017 ; Vennum et al. 2017 ). The yellow cluster included authors Todd K. Shackelford, William J. Chopik, and Justin K. Mogilski, whose work focused on the topic of polygamy (Moors et al. 2019 ; Sela et al. 2017 ). Martine Hebert, Todd K. Shackelford, Frank D. Fincham, and Emily A. Impett emerged as the cooperative network’s central nodes, underscoring their crucial role in advancing research on romantic love.
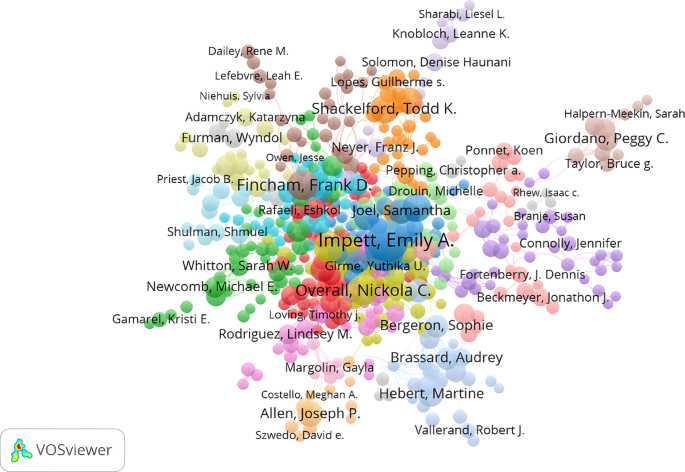
The authors’ cooperative network was partitioned into eight distinct clusters.
Table 2 provided a rundown of the most productive authors, with their published works ranging from 28 to 74 publications, averaging 41. The H-index, a yardstick for measuring academic influence, was employed to assess their impact. Notably, Emily A. Impett emerged as the dominant force within the cohort of scholars dedicated to the study of romantic love, having authored the most papers among the group (74 publications, H-index = 38). Additionally, Nickola C. Overall (42 publications, H-index = 19) and Amy Muise (60 publications, H-index = 30) also featured prominently as leading contributors to the field.
Table 3 and Fig. 4 displayed the number of publications in different fields of study related to the topic of romantic love. Notably, publications in the fields of biology, neuroscience, and economics were also included in Table 3 . The humanities were increasingly collaborating on romantic love research. Furthermore, the topic of romantic love was gaining popularity in the fields of psychology and sociology.
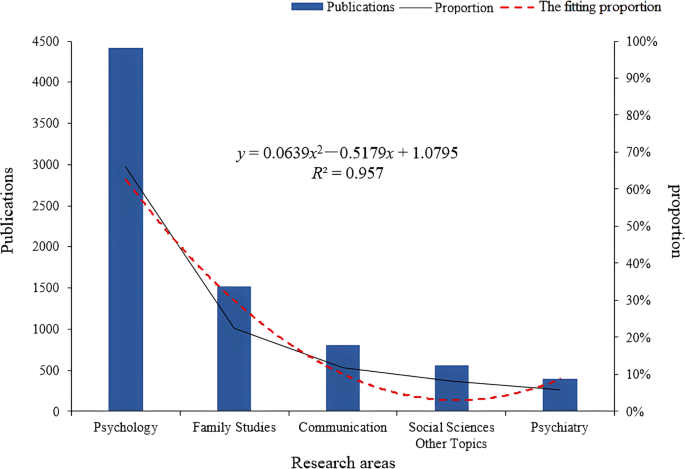
The field of psychology, including psychology and psychiatry, was significantly ahead. The field of sociology encompassed various topics in the social sciences, including sociology and social work.
Distribution by country and institution
A total of 6858 publications had been published and disseminated to 104 countries and regions worldwide. In the country analysis, Scimago Graphica had been used to explore the geographic collaboration network of participating nations. The participants of the current study were drawn from 104 different countries spanning Asia, Africa, Europe, North America, and South America, with Europe exhibiting the highest level of overall engagement, underscoring the global trend toward collaboration. The United States and the United Kingdom had demonstrated the greatest degree of cooperation. Notably, China, South Africa, Spain, Italy, France, and other countries with high cooperation densities had formed the most significant multi-center cooperation network in this field (see Fig. 5 ). Figure 6 illustrated international collaboration.
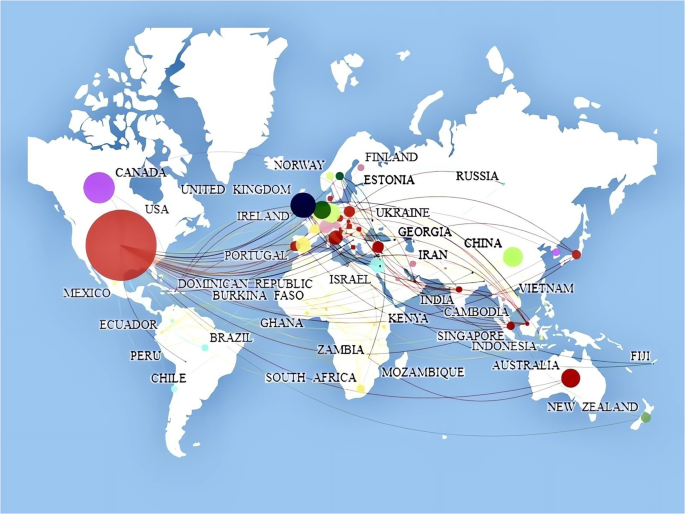
By leveraging Scimago Graphica, it was possible to merge geographical perspectives with national publications and collaborative relationships, providing an intuitive and scientific method to illuminate the various conditions of countries involved in the research on romantic love.
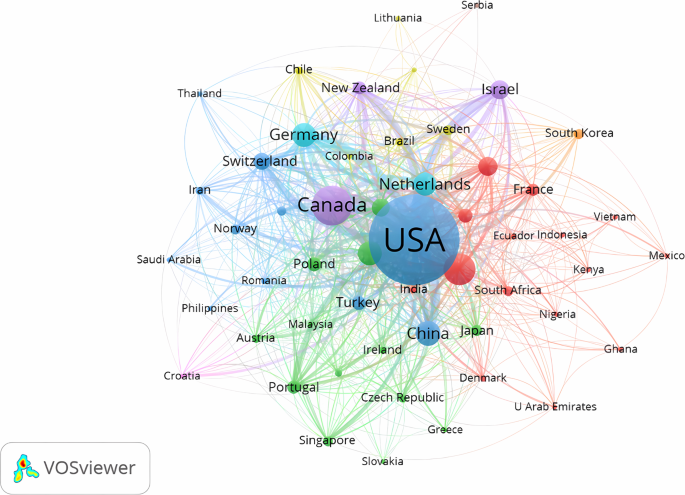
The largest blue cluster was comprised of the United States, China, Switzerland, Turkey, and Norway, demonstrating collaboration across the Americas, Europe, and East Asia.
Table 4 outlined the specifics of the top ten countries in the landscape of romantic love research. The United States topped the list with 4092 publications, followed by Canada with 802 publications, and the United Kingdom with 540 publications. It is noteworthy that the majority of publications were disseminated from high-income countries, aligning with the overall prosperity of those nations. Most papers were disseminated in high-income countries. This trend might have stemmed from the overarching principles governing scientific inquiry, or it could be attributed to authors in these nations having the freedom to engage in research spanning areas not necessarily centered on economic growth. However, within the realm of general well-being, this emerges as a pertinent concern. Primarily, high-income countries historically boasted more affluent reservoirs of research resources, encompassing financial backing, cutting-edge equipment, and a pool of adept talent. This affluence empowered researchers in these nations to embark on a diverse array of investigations, spanning domains intricately tied to economic growth and extending to those delving into broader realms such as general well-being and social development. The discernible divergence in resource allocation likely contributed to the disproportionate prevalence of publications in high-income countries. Secondarily, the scrutiny of whether the romantic love research domain intricately correlates with economic growth warrants profound contemplation. At times, the merit of research doesn’t solely reside in its potential to spur short-term economic growth but extends to its impact on the overarching well-being and sustainable evolution of society. High-income countries, historically oriented toward prioritizing protracted social well-being, manifested a proclivity to endorse research that, while not directly contributing to economic growth, played an indispensable role in the comprehensive development of society. Institutional collaboration was vividly portrayed in Fig. 7 , which consisted of six clusters. A total of 3328 institutions contributed to the 6858 articles on romantic love. Of the top 10 organizations, universities occupied the top spot (as indicated in Table 5 ), with the State University System of Florida (246 publications), the University System of Ohio (248 publications), and the University of California System (365 publications) leading the pack. Notably, nine out of the top 10 institutions hailed from the United States, which was a testament to the country’s exceptional research prowess in this field.
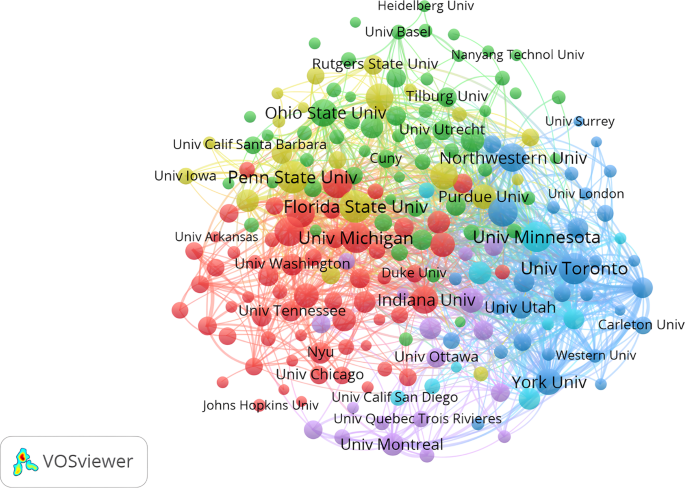
The red cluster denoted collaboration among Florida State University, University of Michigan, University of Washington, and Indiana University; the green cluster represented Ohio State University, University of Basel, and Nanyang Technological University; while the blue cluster embodied York University, the University of Toronto, Northwestern University, and Carleton University. Northwestern University, Florida State University, the University of Minnesota, and the University of Toronto were the major nodes in the cooperative network.
Analysis of references
Reference analysis played a critical role in bibliometric research, as the references with the highest citation bursts formed the foundation of knowledge at the forefront of research (Fitzpatrick 2005 ). In Fig. 8 , the current study presented the most relevant references on romantic love, which had experienced a surge in citations over the past decade. By the end of 2022, Mikulincer and Shaver’s ( 2016 ) articles had seen a significant increase in their citation counts, with the highest spike (14.35) observed in 2016, followed by Wincentak et al.’s ( 2017 ) studies (9.9). These two studies had been widely cited over the years and accurately captured the latest trends in romantic love research.

These references were represented by red and green bars, indicating their frequent and less frequent citation, respectively.
Mikulincer and Shaver’s ( 2016 ) delved into the causes and methods for measuring individual differences in adult attachment, as well as how to modify attachment styles, using several empirical studies. Additionally, they explored the cutting-edge genetics, neurological, and hormonal substrates of attachment, expanding the impact model’s depiction of how the attachment system functioned. In the study, Wincentak et al. ( 2017 ) discussed the prevalence of dating violence among adolescents of different genders using a meta-analysis method, while also examining the potential regulatory effects of age, demographics, and measurement. Research has shown that in adolescent dating violence, the crime rate of women was significantly lower than that of men. Based on the analysis of these articles, current research trends in romantic love included adult attachment and the examination of adolescents’ irrational beliefs about love and the resulting adverse consequences, such as dating violence.
Analysis of keywords
Keyword burst refers to keywords that have shown a sharp increase in frequency over time, enabling the assessment of the current study focus in this area and reflecting the development pattern of future research. The current study extracted the burst terms of various years in the area of romantic love to obtain the burst terms of various years in the area of romantic love (see Fig. 9 ). As we’ve seen, the field had a diverse range of research interests. By the end of 2022, the three words with the highest peak were “same-sex” (2020–2022), “conflict resolution” (2020–2022), and “social relationships” (2020–2022):
Same-sex: in a society that valued heterosexual relationships, same-sex relationships were often met with shame and stigma, leading to additional pressures uniquely linked to their sexual orientation and partnership (Feinstein et al. 2018 ; Rostosky and Riggle 2017 ). Moreover, the online conduct of gay individuals has been demonstrated to have significant implications for their sexual risk behaviors and emotional well-being in romantic relationships (Zhang et al. 2022b ). The development of effective dual interventions has been shown to enhance the health and well-being of same-sex couples and their families. These interventions should also educate parents about the potential negative effects of heteronormative assumptions and attitudes on their children’s positive adolescent development (Pearson and Wilkinson 2013 ).
Conflict resolution: previous research has shown the irony that a person’s favorite individual, such as their romantic partner, is often the very person with whom they engage in destructive behavior during conflicts, making this destructive response one of the most challenging issues in relationships (Alonso-Ferres et al. 2021 ). As a result, it was critical to effectively resolve conflicts in a constructive manner. The emergence of computer-mediated communication (CMC) as a novel conflict resolution approach prompted researchers to explore this matter. Ultimately, they discovered that there were no differences in pain, anger, and conflict resolution levels between face-to-face and CMC discussions (Pollmann et al. 2020 ). Another study focused on neural activity during conflict resolution, revealing that mediation could enhance conflict resolution and was linked to increased activity in the nucleus accumbens, a crucial area of the brain’s reward circuit (Rafi et al. 2020 ). The finding emphasizes the importance of identifying neural mechanisms that could enhance conflict resolution and improve relationship outcomes. By exploring various conflict resolution approaches and associated neural mechanisms, researchers can facilitate a deeper understanding of how to successfully resolve conflicts and enhance relationship satisfaction.
Social relationships: long-term relationships are vital to the mental health of both humans and animals. Positive emotions and experiences, such as romantic or platonic love, play a significant role in the establishment and maintenance of social bonds. With this in mind, researchers integrated brain imaging studies on emotions characterized by social connections to investigate whether and how humans and animals experience social emotions and influences similarly in the context of social relationships (Zablocki-Thomas et al. 2022 ). An ecological and cross-cutting perspective study found that black Americans viewed their partner’s interactions regarding discrimination as an opportunity for their romantic partner to offer support, as revealed in semi-structured interviews (Rice 2023 ). Furthermore, as romantic relationships represent one of the most unique types of social connections, researchers utilized functional magnetic resonance imaging (fMRI) scanning techniques to explore the neurobiological mechanisms of romantic relationships (Eckstein et al. 2023 ), offering valuable insight for the preservation and maintenance of social relationships and interactions.
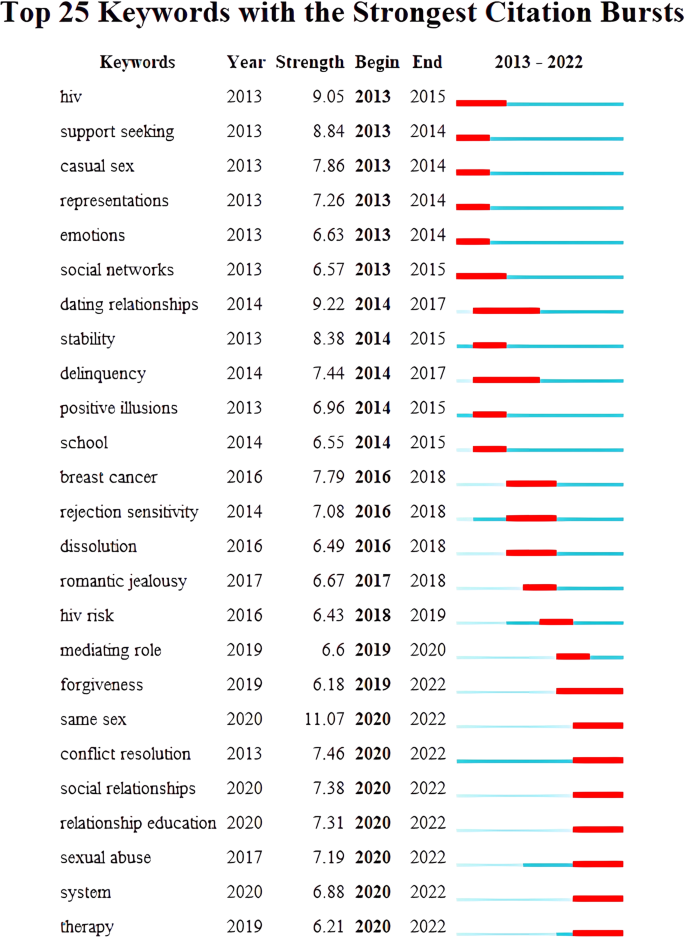
Over the last 10 years, the most popular keywords were “same-sex” (11.07), “dating relationships” (9.22), and “HIV” (9.05), indicating high demand for these topics in recent years. The keywords with the longest blasting times were “dating relationships” (2014–2017) and “delinquency” (2014–2017). The phrases that were still trending in 2022 were hotspots.
Figure 10 illustrated the relationship between keywords. The connection strength between two nodes was a quantitative measure of their relationship. The most frequently used keyword, “romantic relationship,” was represented by the largest node in Fig. 10 (see Table 6 ). The “romantic relationship” (2036) node had thicker lines than “attachment” (766), “gender” (728), “satisfaction” (664), “behavior” (529), “marriage” (508), “commitment” (419), “adolescents” (417), “associations” (395), and “intimate partner relationship” (336). The nodes had a minimum link strength of 150. The close connections between “romantic relationship” and “marriage,” “commitment,” and “intimate partnership” demonstrated the importance of stable, long-term relationships in maintaining romantic love (Fu et al. 2012 ).
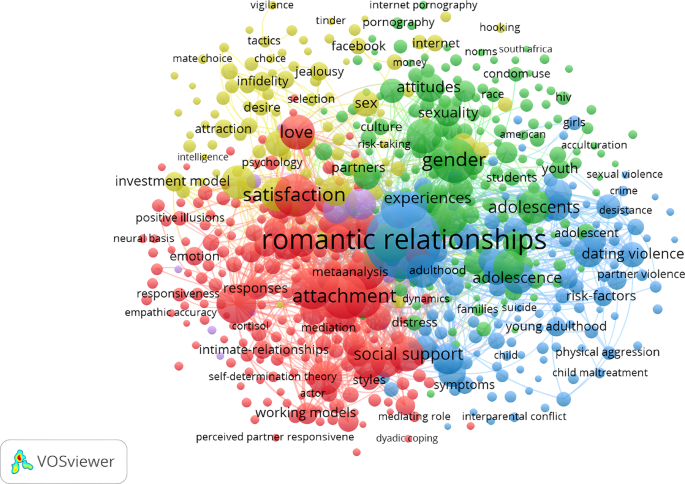
The connection strength between two nodes was a quantitative measure of their relationship. The total link strength of a node was the sum of its link strengths relative to all other nodes (Liao et al. 2018).
Keywords are essential in identifying the central themes and prospective avenues of a publication. By examining the co-occurrence of keywords, one can discern the current trajectory of research and development in a specific field (Zhang et al. 2022c ). In the present investigation, a total of 16,148 keywords were extracted from 6858 articles related to romantic love, with 10,571 being used only once, accounting for 65.46% of the total keywords. Through keyword co-occurrence analysis, six distinct color-coded clusters were identified, comprising attachment, gender, romantic relationships, personality, communication, and dynamics. The red cluster, attachment, delved into the complex relationships among commitment, fulfillment, companionship, and attachment insecurity. To address the diminished satisfaction in partner relationships caused by attachment insecurity, promoting healthy dualistic coping strategies (DCS) was recommended (Peloquin et al. 2022 ). The green cluster, gender, focused on the issues of dating violence victimization experienced by young individuals of different genders, with sexual minorities being particularly vulnerable to bullying (Cosma et al. 2022 ). The blue cluster, romantic connections, primarily examined the link between depressive symptoms and violent intimate partner relationships. Recent studies showed that dating violence and peer victimization were prevalent among young individuals (Smith et al. 2021 ) and that dating aggression was associated with both internalized and externalized psychopathology in young couples (Lantagne and Furman 2021 ). Additionally, the misuse of internet dating may lead to depression (Toplu-Demirtas et al. 2020 ). Apart from the six clusters mentioned, there was a noticeable trend toward integrating research with neuroimaging technology, which might lead to the emergence of new clusters in the realm of romantic love. The interconnectedness of attachment, gender, and romantic relationships was evident in the strong theoretical foundation and widespread attention these clusters received, whereas the clusters of personality, communication, and dynamics were more peripherally related. Due to their significance, future research on romantic love will continue to explore topics such as intimate partner violence, teenage dating violence victimization, attachment insecurity, and sexual abuse, with a focus on the three interconnected clusters of attachment, gender, and romantic relationships. In traditional notions, our understanding of romantic love had primarily consisted of terms such as romantic relationships and intimate commitments. However, practical issues such as misperceptions about love and a lack of regard for partners have gradually shifted the subject matter of research pertaining to romantic love toward dating violence. The research trajectory demonstrates a shift in the focus of romantic love research from a more idealized perspective toward a more realistic one. Finally, Fig. 11 displayed a keyword timeline graph that depicted when the most prevalent keywords first appeared and their evolving importance over time.
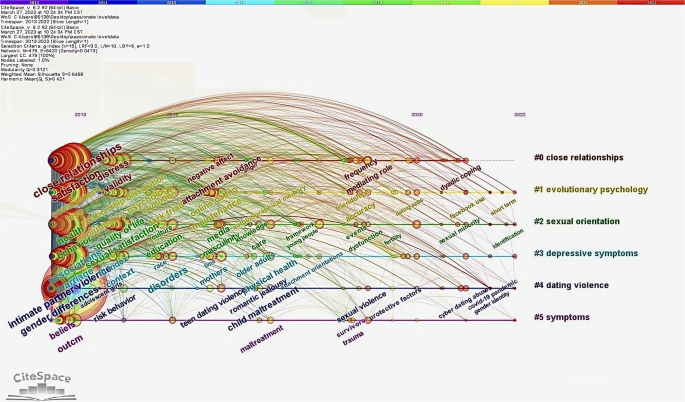
This keyword timeline graph was depicted when the most prevalent keywords first appeared and their evolving importance over time.
The current study used advanced bibliometrics and literature data visualization techniques with CiteSpace, VOSviewer, and Web of Science to examine the growth of research publications in the field of romantic love, as well as the main research nations, journals, and emerging trends. The thorough review provided insight into the present status of development and research in this field, while also clarifying the historical path of scholarship and providing clear guidance for future research. Using bibliometric methods, the study investigated romantic love research from 2013 to 2022. The results showed a steady increase in publications on this topic, with a slight decrease noted in 2019, likely due to the detrimental impact of the COVID-19 pandemic on academic research. However, the analysis of current trends indicates a projected increase in research output on romantic love in the coming years.
Romantic love has been a global phenomenon, with Europe and the United States leading in widespread participation and clear concentration. Among the top 10 countries producing research in this field, the United States led with 4092 publications between 2013 and 2022. China, ranking fourth in terms of publications, emerged as the most prolific developing nation (328). However, compared to the United States, China lagged behind in publications and international collaboration. Therefore, China needs to expand its research efforts in this area and broaden its international partnerships. The top ten research institutions, mainly universities, played a vital role in advancing this field. Notably, nine out of ten of these institutions were located in the United States, further highlighting the preeminent position of American academic institutions in this area of study.
In the current study, we have discovered noteworthy findings regarding notable authors in the field of romantic love. The research studies have primarily focused on four distinct perspectives: the Limerence Theory, the Rate of Change in Intimacy Model, the Self-Expansion Model, and the Triangular Theory of Love. These perspectives have proposed four possible sources of romantic passion and assessed empirical evidence for and against each. Among the authors, Emily A. Impett has emerged as the most prolific author (Carswell and Impett 2021 ). Frank D. Fincham, who has the highest H-index, has conducted extensive research on the interplay between mindfulness and idiosyncratic mindfulness in romantic relationships. Notably, his research on adolescent intimate partner violence has received the most citations (Cui et al. 2013 ; Frank and Ross 2017 ; Kimmes et al. 2018 ). Furthermore, we found that an author’s centrality and citation frequency did not always correlate with their number of publications, indicating that various factors had contributed to an author’s academic influence (Zhang et al. 2022a ).
The term “burst term” refers to a term that unexpectedly appears in research and may indicate new directions or a novel perspective derived from research (Xu et al. 2022 ). According to Fig. 8 , the following references experienced a citation burst by the end of 2022: (1) Mikulincer and Shaver ( 2016 ) delved into the causes and measures of individual differences in adult attachment, explored the modifiability of attachment styles, and unveiled cutting-edge research in genetics, neurology, and hormones associated with attachment. They also extended the impact model’s depiction of the attachment system’s operation. (2) Wincentak et al. ( 2017 ) conducted a meta-analysis to investigate the prevalence of dating violence among adolescents of various genders, while also examining the potential impact of age, demographic factors, and measurement methods. Their findings suggested that the rate of perpetration of dating violence was significantly higher among male adolescents than female adolescents. In other words, male adolescents were more likely to engage in dating violence than their female counterparts. This gender difference in dating violence rates highlighted the need for targeted prevention and intervention efforts to address this issue among young people.
CiteSpace displayed keywords in bursts, as shown in Fig. 9 . These data were significant for reference in cutting-edge prediction research. The terms “same-sex,” “conflict resolution,” and “social relationships” might be used frequently in the coming years, indicating potential areas of focus within the domain of romantic love:
Same-sex: same-sex relationships faced unique pressures and stigma in a society that largely valued heterosexual partnerships, leading to feelings of shame and additional stressors based on sexual orientation (Feinstein et al. 2018 ; Rostosky and Riggle 2017 ). Notably, studies have revealed that the online behavior of gay individuals could significantly impact their emotional well-being and sexual risk behaviors within their romantic relationships (Zhang et al. 2022b ). To improve the health and well-being of same-sex couples and their families, effective dual interventions have been developed, including educating parents about the potential harm caused by heteronormative assumptions and attitudes on their children’s adolescent development (Pearson and Wilkinson 2013 ).
Conflict resolution: prior research has revealed the paradox that a person’s beloved partner, such as their significant other, is often the individual with whom they engage in harmful behavior during conflicts. The negative reaction could be one of the most challenging issues in a relationship (Alonso-Ferres et al. 2021 ). Therefore, it is imperative to resolve conflicts in a successful manner. Computer-mediated communication (CMC) has emerged as a novel approach to conflict resolution, and researchers have investigated this matter, concluding that there are no disparities in the levels of pain, anger, and conflict resolution between face-to-face and CMC discussions (Pollmann et al. 2020 ). Another study explored the neural mechanisms during conflict resolution, and researchers discovered that mediation could improve conflict resolution and was linked to elevated activity in the nucleus accumbens, a crucial area in the brain’s reward circuit (Rafi et al. 2020 ).
Social relationships: long-term relationships play a critical role in maintaining the mental health of both humans and animals. Positive emotions and emotional experiences, such as romantic or platonic love, are intricately linked to the formation and sustenance of social bonds. To gain insights into how social emotions manifest in both humans and animals, researchers integrated brain imaging studies of emotions associated with social connections (Zablocki-Thomas et al. 2022 ). From an ecological and cross-cutting perspective, another study found that Black Americans viewed their partner’s interactions around discrimination as an opportunity for their romantic partner to provide support, as revealed in semi-structured interviews (Rice 2023 ). Furthermore, given the unique nature of romantic relationships in social interactions, researchers used functional magnetic resonance imaging (fMRI) techniques to investigate the neurobiological mechanisms of such relationships (Eckstein et al. 2023 ), which could serve as a reference for the preservation and cultivation of social relationships.
To our knowledge, our study represented a novel application of quantitative bibliometric tools such as CiteSpace and VOSviewer to analyze the literature on romantic love over the past decade. While our analysis yielded intriguing insights into the research landscape of this field, our study was not without limitations. First and foremost, our sample was limited to articles and reviews available in a single database, and thus, may not have been fully representative of the entire research landscape on this topic. Second, the current study restricted our data collection to English-language publications, and future studies may benefit from including publications in other languages to ensure a more comprehensive analysis. Additionally, including different types of publications, such as conference papers and working papers, might have provided further insights into recent advancements in the field. Furthermore, it could be acknowledged that the analysis in the current study could be expanded to consider the contributions of other scholars and institutions in the field, beyond those captured by our data set. Finally, while the bibliometric tools used in our analysis were objective, our interpretation of the results remained subjective and may have been subject to varying interpretations.
Concluding remarks
Research significance and future development.
The present study’s comprehensive analysis of the literature on romantic love, as well as its reporting of research findings across diverse domains over the past decade, offered a solid groundwork for future research and potential worldwide applications. From 2013 to 2022, a staggering 6858 articles and reviews on romantic love were published globally, indicating a bright future for this field of inquiry. In terms of research potency, the United States led the pack, with the University of California System accounting for the majority of publications in the area of romantic love, and Emily A. Impett ranking as the most prolific contributor. The Journal of Social and Personal Relationships had published the most articles on romantic love research, while the most recent trends in romantic love-related keywords included “same-sex,” “conflict resolution,” and “social relationships.” The current research was predominantly centered around intimate relationships, evolutionary psychology, sexual orientation, and symptoms of depression. The trends elucidated by these findings underscore the holistic and interdisciplinary nature of romantic love within the realms of psychology, sociology, biology, and neuroscience. Subsequent investigations into romantic love hold the promise of a more profound amalgamation of methodologies derived from psychology and neuroscience, thereby illuminating the physiological underpinnings of love and emotional experiences. This prospect entails a meticulous exploration of brain activity, probing how intricate psychological processes intertwine with biology to forge the intricacies of romantic relationships. Furthermore, romantic love research stands poised to cultivate seamless integration and interdisciplinary cooperation across a spectrum of fields in the future, yielding profound ramifications.
Method limitation
The current study, which utilized tools such as CiteSpace and Vosviewer for a quantitative analysis of the literature on romantic love over the past 10 years, is the first of its kind to our knowledge. Our investigation, though producing intriguing results through bibliometric analysis and visualization of related articles, is not without its limitations. Firstly, the samples utilized were limited to a single database (WOS), which may not encompass all relevant publications on the subject. Secondly, the scope of our data collection was limited to articles and reviews in English only, leaving out potential information from other types of publications such as working papers and conference papers. In future studies, a broader consideration of different languages should also be given. Additionally, the neural mechanism and physiological function of romantic love remain an under-researched area with limited empirical evidence to support ongoing controversy.
Data availability
Original data for the current study are available via this link: https://rec.ustc.edu.cn/share/0d874150-b039-11ee-be97-f5a41b2eeb6e .
Acevedo BP, Aron A, Fisher HE, Brown LL (2012) Neural correlates of long-term intense romantic love. Soc Cogn Affect Neurosci 7(2):145–159
Article PubMed Google Scholar
Acevedo BP, Poulin MJ, Collins NL, Brown LL (2020) After the honeymoon: neural and genetic correlates of romantic love in newlywed marriages. Front Psychiatry 11:634
Article Google Scholar
Alirezanejad S (2022) Becoming a wife, a beloved, or both: caught in feminine struggle in Tehran. Sex Cult 26(3):811–833
Alonso-Ferres M, Valor-Segura I, Expósito F (2021) Elucidating the effect of perceived power on destructive responses during romantic conflicts. Span J Psychol 24:e21
Aron A, Fisher H, Mashek DJ, Strong G, Li H, Brown LL (2005) Reward, motivation, and emotion systems associated with early-stage intense romantic love. J Neurophysiol 94(1):327–337
Bartels A, Zeki S (2000) The neural basis of romantic love. NeuroReport 11(17):3829–3834
Article CAS PubMed Google Scholar
Bartels A, Zeki S (2004) The neural correlates of maternal and romantic love. NeuroImage 21(3):1155–1166
Budziszewska MD, Babiuch-Hall M, Wielebska K (2020) Love and romantic relationships in the voices of patients who experience psychosis: an interpretive phenomenological analysis. Front Psychol 11:570928
Article PubMed PubMed Central Google Scholar
Carswell KL, Impett EA (2021) What fuels passion? An integrative review of competing theories of romantic passion. Soc Personal Psychol Compass 15(8):e12629
Cenat JM, Mukunzi JN, Amedee LM, Clormeus LA, Dalexis RD, Lafontaine MF, Hebert M (2022) Prevalence and factors related to dating violence victimization and perpetration among a representative sample of adolescents and young adults in Haiti. Child Abus Negl 128(3):105597
Centers for Disease Control and Prevention (2017) Key statistics from the National Survey of Family Growth—D Listing. https://www.cdc.gov/nchs/nsfg/key_statistics/d.htm#divorce
Chester DS, Martelli AM, West SJ, Lasko EN, Brosnan P, Makhanova A, McNulty JK (2021) Neural mechanisms of intimate partner aggression. Biol Psychol 165:108195
Cosma A, Kolto A, Young H, Thorsteinsson E, Godeau E, Saewyc E, Gabhainn SN (2022) Romantic love and involvement in bullying and cyberbullying in 15-year-old adolescents from eight European countries and regions. J LGBT Youth 20(1):33–54
Cui M, Gordon M, Ueno K, Fincham FD (2013) The continuation of intimate partner violence from adolescence to young adulthood. J Marriage Fam 75(2):300–313
Daim TU, Rueda G, Martin H, Gerdsri P (2006) Forecasting emerging technologies: use of bibliometrics and patent analysis. Technol Forecast Soc Change 73(8):981–1012
Eckstein M, Stossel G, Gerchen MF, Bilek E, Kirsch P, Ditzen B (2023) Neural responses to instructed positive couple interaction: an fMRI study on compliment sharing. Soc Cogn Affect Neurosci 18(1):nsad005
Ellegaard O, Wallin JA (2015) The bibliometric analysis of scholarly production: how great is the impact? Scientometrics 105(3):1809–1831
Feinstein BA, McConnell E, Dyar C, Mustanski B, Newcomb ME (2018) Minority stress and relationship functioning among young male same-sex couples: an examination of actor–partner interdependence models. J Consult Clin Psychol 86(5):416–426
Fehr B (2013) The social psychology of love. In: Simpson JA, Campbell L (eds.) The Oxford handbook of close relationships. Oxford University Press, Oxford, p 201–233
Google Scholar
Fehr B (2015) Love: conceptualization and experience. In: Mikulincer M, Shaver PR, Simpson JA, Dovidio JF (eds.) APA handbook of personality and social psychology, vol 3 interpersonal relations. American Psychological Association, Washington, p 495–522
Chapter Google Scholar
Fisher HE, Brown LL, Aron A, Strong G, Mashek D (2010) Reward, addiction, and emotion regulation systems associated with rejection in love. J Neurophysiol 104(1):51–60
Fitzpatrick RB (2005) Essential science indicators. Med Ref Serv Q 24(4):67–78
Fletcher GJ, Simpson JA, Campbell L, Overall NC (2015) Pair-bonding, romantic love, and evolution: the curious case of homo sapiens. Perspect Psychol Sci 10(1):20–36
Frank DF, Ross WM (2017) Infidelity in romantic relationships. Curr Opin Psychol 13:70–74
Fu Y, Zhou Y, Liang ZY, Li S (2012) New insights into the neurophysiological mechanism of romantic love. Chin Sci Bull 57(35):3376–3383
Gao C, Wang R, Zhang L, Yue CW (2021) Visualization analysis of CRISPR gene-editing knowledge map based on Citespace. Biol Bull 48(6):705–720
Hatfield E, Rapson RL (1987) Passionate love/sexual desire: can the same paradigm explain both? Arch Sex Behav 16(3):259–278
He TM, Ao JW, Duan CC, Yan R, Li XM, Liu L, Li XF (2022) Bibliometric and visual analysis of nephrotoxicity research worldwide. Front Pharmacol 13:940791
Article CAS PubMed PubMed Central Google Scholar
Hou ZM, Jiang P, Su ST, Zhou HH (2022) Hotspots and trends in multiple myeloma bone diseases: a bibliometric visualization analysis. Front Pharmacol 13:1003228
Jimenez-Picon N, Romero-Martin M, Romero-Castillo R, Palomo-Lara JC, Alonso-Ruiz M (2022) Internalization of the romantic love myths as a risk factor for gender violence: a systematic review and meta-analysis. Sex Res Soc Policy. https://doi.org/10.1007/s13178-022-00747-2
Kerr S, Penner F, Ilagan G, Choi‑Kain L, Sharp C (2022) Maternal interpersonal problems and attachment security in adolescent offspring. Borderline Pers Disord Emot Dysregulation 9(1):18
Kimmes JG, Jaurequi ME, May RW, Srivastava S, Fincham FD (2018) Mindfulness in the context of romantic relationships: initial development and validation of the relationship mindfulness measure. J Marital Fam Ther 44(4):575–589
Lafontaine MF, Azzi S, Bell-Lee B, Dixon-Luinenburg T, Guérin-Marion C, Bureau JF (2020) Romantic perfectionism and perceived conflict mediate the link between insecure romantic attachment and intimate partner violence in undergraduate students. J Fam Violence 36(2):195–208
Langeslag SJE (2022) Electrophysiological correlates of romantic love: a review of EEG and ERP studies with beloved-related stimuli. Brain Sci 12(5):551
Lantagne A, Furman W (2021) A dyadic perspective on psychopathology and young adult physical dating aggression. Psychol Violence 11(6):569–579
Li Y, Wagner B, Guo G (2022) Romantic partnerships and criminal offending: examining the roles of premarital cohabitation, serial cohabitation, and gender. Justice Q. https://doi.org/10.1080/07418825.2022.2118618
Liao HC, Tang M, Luo L, Li CY, Chiclana F, Zeng XJ (2018) A bibliometric analysis and visualization of medical big data research. Sustainability 10(1):166
Lonergan M, Saumier D, Pigeon S, Etienne PE, Brunet A (2022) Treatment of adjustment disorder stemming from romantic betrayal using memory reactivation under propranolol: a open-label interrupted time series trial. J Affect Disord 317:98–106
Merritt OA, Rowa K, Purdon CL (2022) Context matters: criticism and accommodation by close others associated with treatment attitudes in those with anxiety. Behav Cogn Psychother 51(1):1–11
Mikulincer M, Shaver PR (2016) Attachment in adulthood: structure, dynamics, and change, 2nd edn. The Guilford Press, New York
Mizrahi M, Lemay EP, Maniaci MR, Reis HT (2022) Seeds of love: positivity bias mediates between passionate love and prorelationship behavior in romantic couples. J Soc Personal Relatsh 39(7):2207–2227
Moors AC, Ryan W, Chopik WJ (2019) Multiple loves: the effects of attachment with multiple concurrent romantic partners on relational functioning. Personal Individ Differ 147:102–110
Niolon PH, Kuperminc GP, Allen JP (2015) Autonomy and relatedness in mother-teen interactions as predictors of involvement in adolescent dating aggression. Psychol Violence 5(2):133–143
Oosthuizen JC, Fenton JE (2014) Alternatives to the impact factor. Surgeon 12(5):239–243
Pearson J, Wilkinson L (2013) Family relationships and adolescent well-being: are families equally protective for same-sex attracted youth? J Youth Adolescence 42(9):1494–1496
Peloquin K, Boucher S, Benoit Z, Jean M, Beauvilliers L, Carranza-Mamane B, Brassard A (2022) “We’re in this together”: attachment insecurities, dyadic coping strategies, and relationship satisfaction in couples involved in medically assisted reproduction. J Marital Fam Ther 49(1):92–110
Pollmann MMH, Crockett EE, Vanden Abeele MMP, Schouten AP (2020) Does attachment style moderate the effect of computer-mediated versus face-to-face conflict discussions? Pers Relatsh 27(1):939–955
Quintard V, Jouffe S, Hommel B, Bouquet CA (2021) Embodied self-other overlap in romantic love: a review and integrative perspective. Psychol Res 85(3):899–914
Rafi H, Bogacz F, Sander D, Klimecki O (2020) Impact of couple conflict and mediation on how romantic partners are seen: an fMRI study. Cortex 130:302–317
Randall AK, Bodenmann G (2017) Stress and its associations with relationship satisfaction. Curr Opin Psychol 13:96–106
Reis HT, Aron A, Clark MS, Finkel EJ (2013) Ellen Berscheid, Elaine Hatfield, and the emergence of relationship science. Perspect Psychol Sci 8(5):558–572
Rice TM (2023) Echoes of slavery: reflections on contemporary racial discrimination in Black Americans’ romantic relationships. J Soc Pers Relat. https://doi.org/10.1177/02654075231154934
Rostosky SS, Riggle ED (2017) Same-sex relationships and minority stress. Curr Opin Psychol 13:29–38
Sela Y, Mogilski JK, Shackelford TK, Zeigler-Hill V, Fink B (2017) Mate value discrepancy and mate retention behaviors of self and partner. J Personal 85(5):730–740
Smith K, Hebert M, Brendgen M, Blais M (2021) The mediating role of internalizing problems between peer victimization and dating violence victimization: a test of the stress generation hypothesis. J Interpers Violence 37(1):13–14
Sorokowski P, Sorokowska A, Schmehl S et al. (2021) Universality of the triangular theory of love: adaptation and psychometric properties of the Triangular Love Scale in 25 countries. J Sex Res 58(1):106–115
Tobore TO (2020) Towards a comprehensive theory of love: the quadruple theory. Front Psychol 11:862
Toplu-Demirtas E, May RW, Seibert GS, Fincham FD (2020) Does cyber dating abuse victimization increase depressive symptoms or vice versa? J Interpers Violence 37(2):1–17
Vennum A, Monk JK, Pasley BK, Fincham FD (2017) Emerging adult relationship transitions as opportune times for tailored interventions. Emerg Adulthood 5(4):293–305
Wang LF, Liu XN, Zhang K, Liu ZC, Yi Q, Jiang J, Xia YY (2021) A bibliometric analysis and review of recent researches on Piezo (2010–2020). Channels 15(1):310–321
Wang ZM (2016) Comparative analysis of research hotspots of related data at home and abroad. Knowl Manag Forum 1(3):163–173
William WH, Concepción SW (2001) The literature of bibliometrics, scientometrics, and informetrics. Scientomerics 52(2):291–314
Wincentak K, Connolly J, Card N (2017) Teen dating violence: a meta-analytic review of prevalence rates. Psychol Violence 7(2):224–241
Xu ZP, Shao TJ, Dong ZB, Li SL (2022) Research progress of heavy metals in desert-visual analysis based on CiteSpace. Environ Sci Pollut Res 29(29):43648–43661
Article CAS Google Scholar
Zablocki-Thomas PB, Rogers FD, Bales KL (2022) Neuroimaging of human and non-human animal emotion and affect in the context of social relationships. Front Behav Neurosci 16:994504
Zagefka H (2022) Lay beliefs about the possibility of finding enduring love: a mediator of the effect of parental relationship quality on own romantic relationship quality. Am J Fam Ther. https://doi.org/10.1080/01926187.2022.2084797
Zeevi L, Selle NK, Kellmann EL, Boiman G, Hart Y, Atzil S (2022) Bio‑behavioral synchrony is a potential mechanism for mate selection in humans. Sci Rep 12(1):4786
Article ADS CAS PubMed PubMed Central Google Scholar
Zhang AD, Reynolds NR, Huang CM, Tan SM, Yang GL, Yan J (2022b) The process of contemporary gay identity development in China: the influence of internet use. Front Public Health 10:954674
Zhang F, Ye J, Bai Y, Wang H, Wang W (2022c) Exercise-based renal rehabilitation: a bibliometric analysis from 1969 to 2021. Front Med 9:842919
Article ADS Google Scholar
Zhang SY, Wang S, Liu RL, Dong H, Zhang XH, Tai XT (2022a) A bibliometric analysis of research trends of artificial intelligence in the treatment of autistic spectrum disorders. Front Psychiatry 13:967074
Download references
Acknowledgements
This research was supported by the Starting Fund for Scientific Research of High-Level Talents at Anhui Agricultural University (rc432206) and the Outstanding Youth Program of Philosophy and Social Sciences in Anhui Province (2022AH030089) to SL.
Author information
Authors and affiliations.
Department of Psychology, School of Humanities and Social Sciences, Anhui Agricultural University, Hefei, 230036, Anhui, China
Yixue Han, Yulin Luo, Zhuohong Chen, Nan Gao, Yangyang Song & Shen Liu
You can also search for this author in PubMed Google Scholar
Contributions
SL worked toward conceptualization, validation, supervision, foundation, and editing. YH worked toward methodology, writing, and formal analysis. YL, ZC, NG, and YS worked toward writing, validation, and formal analysis.
Corresponding author
Correspondence to Shen Liu .
Ethics declarations
Competing interests.
The authors declare no competing interests.
Ethical approval
Ethical approval was not required as the current study did not involve human participants.
Informed consent
Informed consent was not required as the current study did not involve human participants.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/ .
Reprints and permissions
About this article
Cite this article.
Han, Y., Luo, Y., Chen, Z. et al. A decade of love: mapping the landscape of romantic love research through bibliometric analysis. Humanit Soc Sci Commun 11 , 187 (2024). https://doi.org/10.1057/s41599-024-02665-7
Download citation
Received : 20 October 2023
Accepted : 11 January 2024
Published : 31 January 2024
DOI : https://doi.org/10.1057/s41599-024-02665-7
Share this article
Anyone you share the following link with will be able to read this content:
Sorry, a shareable link is not currently available for this article.
Provided by the Springer Nature SharedIt content-sharing initiative
This article is cited by
Mapping the landscape of internet pornography, loneliness, and social media addiction: a citespace bibliometric analysis.
- Abhishek Prasad
- Kadhiravan Subramanian
International Journal of Mental Health and Addiction (2024)
Quick links
- Explore articles by subject
- Guide to authors
- Editorial policies
HYPOTHESIS AND THEORY article
Towards a comprehensive theory of love: the quadruple theory.

- Independent Researcher, San Diego, CA, United States
Scholars across an array of disciplines including social psychologists have been trying to explain the meaning of love for over a century but its polysemous nature has made it difficult to fully understand. In this paper, a quadruple framework of attraction, resonance or connection, trust, and respect are proposed to explain the meaning of love. The framework is used to explain how love grows and dies and to describe brand love, romantic love, and parental love. The synergistic relationship between the factors and how their variations modulate the intensity or levels of love are discussed.
Introduction
Scholars across an array of disciplines have tried to define the meaning and nature of love with some success but questions remain. Indeed, it has been described as a propensity to think, feel, and behave positively toward another ( Hendrick and Hendrick, 1986 ). However, the application of this approach has been unsuccessful in all forms of love ( Berscheid, 2010 ). Some social psychologists have tried to define love using psychometric techniques. Robert Sternberg Triangular Theory of Love and Clyde and Susan Hendrick’s Love Attitudes Scale (LAS) are notable attempts to employ the psychometric approach ( Hendrick and Hendrick, 1986 ; Sternberg, 1986 ). However, data analysis from the administration of the LAS, Sternberg’s scale and the Passionate Love Scale by Hatfield and Sprecher’s (1986) found a poor association with all forms of love ( Hendrick and Hendrick, 1989 ). Other studies have found a poor correlation between these and other love scales with different types of love ( Whitley, 1993 ; Sternberg, 1997 ; Masuda, 2003 ; Graham and Christiansen, 2009 ).
In recent years, the neuropsychological approach to study the nature of love has gained prominence. Research has compared the brain activity of people who were deeply in love while viewing a picture of their partner and friends of the same age using functional magnetic resonance imaging (fMRI) and concluded that there is a specialized network of the brain involved in love ( Bartels and Zeki, 2000 ). Indeed, several lines of investigation using fMRI have described a specialized area of the brain mediating maternal love ( Noriuchi et al., 2008 ; Noriuchi and Kikuchi, 2013 ) and, fMRI studies have implicated multiple brain systems particularly the reward system in romantic love ( Aron et al., 2005 ; Fisher et al., 2005 , 2010 ; Beauregard et al., 2009 ). Brain regions including ventral tegmental area, anterior insula, ventral striatum, and supplementary motor area have been demonstrated to mediate social and material reward anticipation ( Gu et al., 2019 ). Although brain imaging provides a unique insight into the nature of love, making sense of the psychological significance or inference of fMRI data is problematic ( Cacioppo et al., 2003 ).
Also, there has been growing interests in the neurobiology of love. Indeed, evidence suggests possible roles for oxytocin, vasopressin, dopamine, serotonin, testosterone, cortisol, morphinergic system, and nerve growth factor in love and attachment ( Esch and Stefano, 2005 ; De Boer et al., 2012 ; Seshadri, 2016 ; Feldman, 2017 ). However, in many cases, definite proof is still lacking and the few imaging studies on love are limited by selection bias on the duration of a love affair, gender and cultural differences ( De Boer et al., 2012 ).
So, while advances have been made in unraveling the meaning of love, questions remain and a framework that can be employed to understand love in all its forms remains to be developed or proposed. The objective of this article is to propose a novel framework that can be applied to all forms of love.
Theoretical Background and Hypothesis Development (The AAC Model)
In the past few decades, the psychological literature has defined and described different forms of love and from these descriptions, the role of attraction, attachment-commitment, and caregiving (AAC), appears to be consistent in all forms of love.
Attraction theory is one of the first approaches to explain the phenomenon of love and several studies and scholarly works have described the importance of attraction in different forms of love ( Byrne and Griffitt, 1973 ; Berscheid and Hatfield, 1978 ; Fisher et al., 2006 ; Braxton-Davis, 2010 ; Grant-Jacob, 2016 ). Attraction has been described as an evolutionary adaptation of humans for mating, reproduction, and parenting ( Fisher et al., 2002a , 2006 ).
The role of attachment in love has also been extensively investigated. Attachment bonds have been described as a critical feature of mammals including parent-infant, pair-bonds, conspecifics, and peers ( Feldman, 2017 ). Indeed, neural networks including the interaction of oxytocin and dopamine in the striatum have been implicated in attachment bonds ( Feldman, 2017 ). The key features of attachment include proximity maintenance, safety and security, and separation distress ( Berscheid, 2010 ). Multiple lines of research have proposed that humans possess an innate behavioral system of attachment that is essential in love ( Harlow, 1958 ; Bowlby, 1977 , 1988 , 1989 ; Ainsworth, 1985 ; Hazan and Shaver, 1987 ; Bretherton, 1992 ; Carter, 1998 ; Burkett and Young, 2012 ). Attachment is essential to commitment and satisfaction in a relationship ( Péloquin et al., 2013 ) and commitment leads to greater intimacy ( Sternberg, 1986 ).
Also, several lines of evidence have described the role of caregiving in love. It has been proposed that humans possess an inborn caregiving system that complements their attachment system ( Bowlby, 1973 ; Ainsworth, 1985 ). Indeed, several studies have used caregiving scale and compassionate love scale, to describe the role of caring, concern, tenderness, supporting, helping, and understanding the other(s), in love and relationships ( Kunce and Shaver, 1994 ; Sprecher and Fehr, 2005 ). Mutual communally responsive relationships in which partners attend to one another’s needs and welfare with the expectation that the other will return the favor when their own needs arise ( Clark and Mills, 1979 ; Clark and Monin, 2006 ), have been described as key in all types of relationships including friendship, family, and romantic and compassionate love ( Berscheid, 2010 ).
Attachment and caregiving reinforce each other in relationships. Evidence suggests that sustained caregiving is frequently accompanied by the growth of familiarity between the caregiver and the receiver ( Bowlby, 1989 , p. 115) strengthening attachment ( Berscheid, 2010 ). Several studies have proposed that attachment has a positive influence on caregiving behavior in love and relationships ( Carnelley et al., 1996 ; Collins and Feeney, 2000 ; Feeney and Collins, 2001 ; Mikulincer, 2006 ; Canterberry and Gillath, 2012 ; Péloquin et al., 2013 ).
The AAC model can be seen across the literature on love. Robert Sternberg triangular theory of love which proposes that love has three components —intimacy, passion, and commitment ( Sternberg, 1986 ), essentially applies the AAC model. Passion, a key factor in his theory, is associated with attraction ( Berscheid and Hatfield, 1978 ), and many passionate behaviors including increased energy, focused attention, intrusive thinking, obsessive following, possessive mate guarding, goal-oriented behaviors and motivation to win and keep a preferred mating partner ( Fisher et al., 2002b , 2006 ; Fisher, 2005 ). Also, evidence indicates that attachment is central to intimacy, another pillar of the triangular theory ( Morris, 1982 ; Feeney and Noller, 1990 ; Oleson, 1996 ; Grabill and Kent, 2000 ). Commitment, the last pillar of the triangular theory, is based on interdependence and social exchange theories ( Stanley et al., 2010 ), which is connected to mutual caregiving and secure attachment.
Hendrick and Hendrick’s (1986) , Love Attitudes Scale (LAS) which measures six types of love ( Hendrick and Hendrick, 1986 ) is at its core based on the AAC model. Similarly, numerous works on love ( Rubin, 1970 ; Hatfield and Sprecher, 1986 ; Fehr, 1994 ; Grote and Frieze, 1994 ), have applied one or all of the factors in the ACC model. Berscheid (2010) , proposed four candidates for a temporal model of love including companionate love, romantic love, and compassionate love and adult attachment love. As described, these different types of love (romantic, companionate, compassionate, and attachment) all apply at least one or all of the factors in the AAC model.
New Theory (The Quadruple Framework)
The AAC model can be fully captured by four fundamental factors; attraction, connection or resonance, trust, and respect, providing a novel framework that could explain love in all its forms. Table 1 shows the core factors of love, and the four factors derived from them.
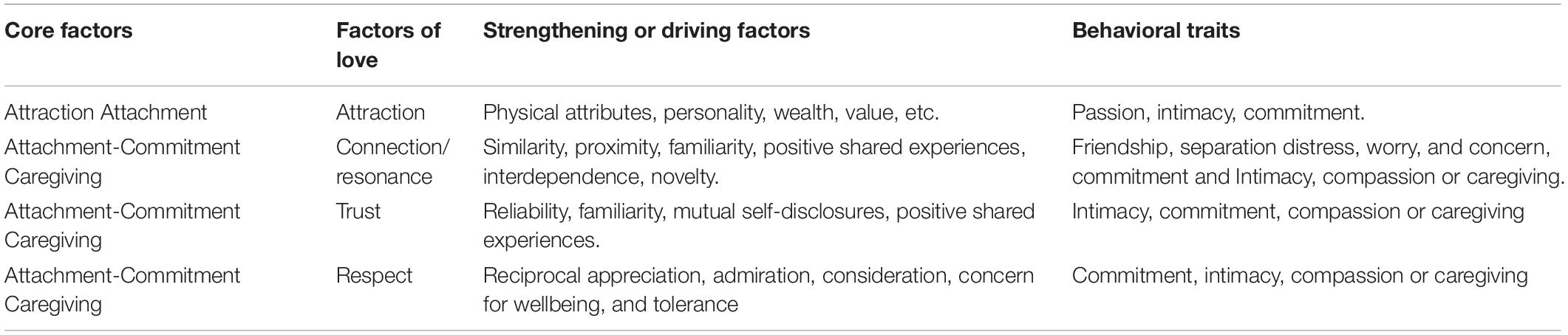

Table 1. Factors of love.
Evidence suggests that both attachment and attraction play a role in obsession or passion observed in love ( Fisher et al., 2005 ; Honari and Saremi, 2015 ). Attraction is influenced by the value or appeal perceived from a relationship and this affects commitment ( Rusbult, 1980 ).
Connection or Resonance
Connection is key to commitment, caregiving, and intimacy. It creates a sense of oneness in relationships and it is strengthened by proximity, familiarity, similarity, and positive shared experiences ( Sullivan et al., 2011 ; Beckes et al., 2013 ). Homogeneity or similarity has been observed to increase social capital and engagement among people ( Costa and Kahn, 2003a , b ), and it has been described as foundational to human relationships ( Tobore, 2018 , pp. 6–13). Research indicates that similarity plays a key role in attachment and companionship as people are more likely to form long-lasting and successful relationships with those who are more similar to themselves ( Burgess and Wallin, 1954 ; Byrne, 1971 ; Berscheid and Reis, 1998 ; Lutz-Zois et al., 2006 ). Proximity plays a key role in caregiving as people are more likely to show compassion to those they are familiar with or those closest to them ( Sprecher and Fehr, 2005 ). Similarity and proximity contribute to feelings of familiarity ( Berscheid, 2010 ). Also, caregiving and empathy are positively related to emotional interdependence ( Hatfield et al., 1994 ).
Trust is crucial for love ( Esch and Stefano, 2005 ) and it plays an important role in relationship intimacy and caregiving ( Rempel and Holmes, 1985 ; Wilson et al., 1998 ; Salazar, 2015 ), as well as attachment ( Rodriguez et al., 2015 ; Bidmon, 2017 ). Familiarity is a sine qua non for trust ( Luhmann, 1979 ), and trust is key to relationship satisfaction ( Simpson, 2007 ; Fitzpatrick and Lafontaine, 2017 ).
Respect is cross-cultural and universal ( Frei and Shaver, 2002 ; Hendrick et al., 2010 ) and has been described as fundamental in love ( Hendrick et al., 2011 ). It plays a cardinal role in interpersonal relations at all levels ( Hendrick et al., 2010 ). Indeed, it is essential in relationship commitment and satisfaction ( Hendrick and Hendrick, 2006 ) and relationship intimacy and attachment ( Alper, 2004 ; Hendrick et al., 2011 ).
Synergetic Interactions of the Four Factors
Connection and attraction.
Similarity, proximity, and familiarity are all important in connection because they promote attachment and a sense of oneness in a relationship ( Sullivan et al., 2011 ; Beckes et al., 2013 ). Research indicates that proximity ( Batool and Malik, 2010 ) and familiarity positively influence attraction ( Norton et al., 2015 ) and several lines of evidence suggests that people are attracted to those similar to themselves ( Sykes et al., 1976 ; Wetzel and Insko, 1982 ; Montoya et al., 2008 ; Batool and Malik, 2010 ; Collisson and Howell, 2014 ). Also, attraction mediates similarity and familiarity ( Moreland and Zajonc, 1982 ; Elbedweihy et al., 2016 ).
Respect and Trust
Evidence suggests that respect promotes trust ( Ali et al., 2012 ).
Connection, Respect, Trust, and Attraction
Trust affects attraction ( Singh et al., 2015 ). Trust and respect can mediate attitude similarity and promote attraction ( Singh et al., 2016 ).
So, although these factors can operate independently, evidence suggests that the weakening of one factor could negatively affect the others and the status of love. Similarly, the strengthening of one factor positively modulates the others and the status of love.
Relationships are dynamic and change as events and conditions in the environment change ( Berscheid, 2010 ). Love is associated with causal conditions that respond to these changes favorably or negatively ( Berscheid, 2010 ). In other words, as conditions change, and these factors become present, love is achieved and if they die, it fades. Figure 1 below explains how love grows and dies. Point C in the figure explains the variations in the intensity or levels of love and this variation is influenced by the strength of each factor. The stronger the presence of all factors, the higher the intensity and the lower, the weaker the intensity of love. The concept of non-love is similar to the “non-love” described in Sternberg’s triangular theory of love in which all components of love are absent ( Sternberg, 1986 ).
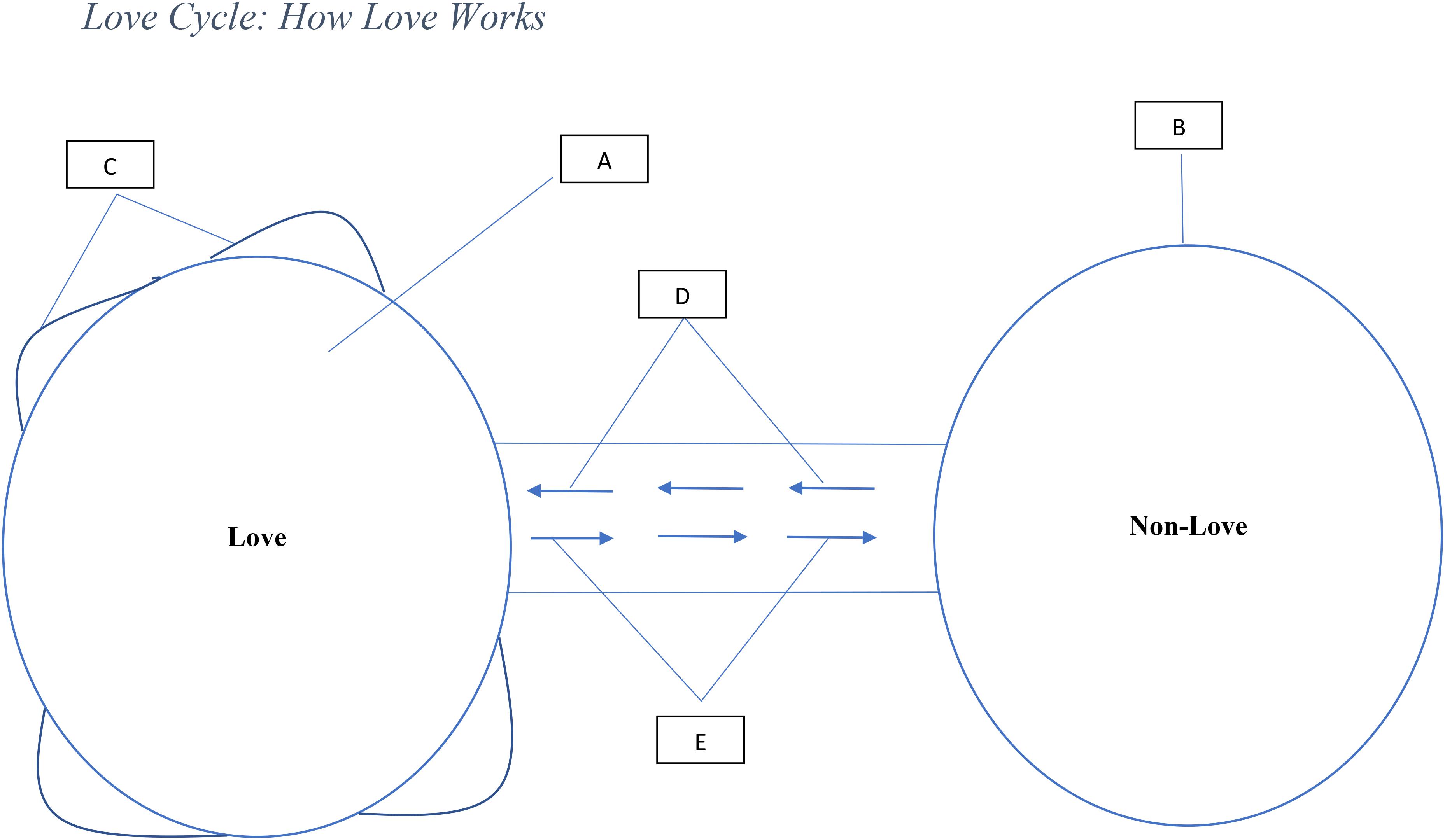
Figure 1. Description: (A) Presence of love (all factors are present). (B) Absence of love (state of non-love or state where all factors are latent or dormant). (C) Different levels of love due to variations in the four factors. (D) Movement from non-love toward love (developmental stage: at least one but not all four factors are present). (E) Movement away from love toward non-love (decline stage: at least one or more of the four factors are absent).
Application of the Quadruple Framework on Romantic, Brand and Parental Love
Romantic, parental and brand love have been chosen to demonstrate the role of these factors and their interactions in love because there is significant existing literature on them. However, they can be applied to understand love in all its forms.
Romantic Love
Attraction and romantic love.
Attraction involves both physical and personality traits ( Braxton-Davis, 2010 ; Karandashev and Fata, 2014 ). To this end, attraction could be subdivided into sexual or material and non-sexual or non-material attraction. Sexual or material attraction includes physical attributes such as beauty, aesthetics, appeal, wealth, etc. In contrast, non-sexual or non-material attraction includes characteristics such as personality, social status, power, humor, intelligence, character, confidence, temperament, honesty, good quality, kindness, integrity, etc. Both types of attraction are not mutually exclusive.
Romantic love has been described as a advanced form of human attraction system ( Fisher et al., 2005 ) and it fits with the passion component of Sternberg’s triangular theory of love which he described as the quickest to recruit ( Sternberg, 1986 ). Indeed, research indicates that physical attractiveness and sensual feelings are essential in romantic love and dating ( Brislin and Lewis, 1968 ; Regan and Berscheid, 1999 ; Luo and Zhang, 2009 ; Braxton-Davis, 2010 ; Ha et al., 2010 ; Guéguen and Lamy, 2012 ) and sexual attraction often provides the motivational spark that kickstarts a romantic relationship ( Gillath et al., 2008 ). Behavioral data suggest that love and sex drive follow complementary pathways in the brain ( Seshadri, 2016 ). Indeed, the neuroendocrine system for sexual attraction and attachment appears to work synergistically motivating individuals to both prefer a specific mating partner and to form an attachment to that partner ( Seshadri, 2016 ). Sex promotes the activity of hormones involved in love including arginine vasopressin in the ventral pallidum, oxytocin in the nucleus accumbens and stimulates dopamine release which consequently motivates preference for a partner and strengthens attachment or pair-bonding ( Seshadri, 2016 ).
Also, romantic love is associated with non-material attraction. Research indicates that many people are attracted to their romantic partner because of personality traits like generosity, kindness, warmth, humor, helpfulness, openness to new ideas ( Giles, 2015 , pp. 168–169). Findings from a research study on preferences in human mate selection indicate that personality traits such as kindness/considerate and understanding, exciting, and intelligent are strongly preferred in a potential mate ( Buss and Barnes, 1986 ). Indeed, character and physical attractiveness have been found to contribute jointly and significantly to romantic attraction ( McKelvie and Matthews, 1976 ).
Attraction is key to commitment in a romantic relationship ( Rusbult, 1980 ), indicating that without attraction a romantic relationship could lose its luster. Also, romantic attraction is weakened or declines as the reason for its presence declines or deteriorates. If attraction is sexual or due to material characteristics, then aging or any accident that compromises physical beauty would result in its decline ( Braxton-Davis, 2010 ). Loss of fortune or social status could also weaken attraction and increase tension in a relationship. Indeed, tensions about money increase marital conflicts ( Papp et al., 2009 ; Dew and Dakin, 2011 ) and predicted subsequent divorce ( Amato and Rogers, 1997 ).
Connection and Romantic Love
Connection or resonance fits with the intimacy, and commitment components of Sternberg’s triangular theory of love ( Sternberg, 1986 ). Connection in romantic love involves intimacy, friendship or companionship and caregiving and it is strengthened by novelty, proximity, communication, positive shared experiences, familiarity, and similarity. It is what creates a sense of oneness between romantic partners and it is expressed in the form of proximity seeking and maintenance, concern, and compassion ( Neto, 2012 ). Evidence suggests that deeper levels of emotional involvement or attachment increase commitment and cognitive interdependence or tendency to think about the relationship in a pluralistic manner, as reflected in the use of plural pronouns to describe oneself, romantic partner and relationship ( Agnew et al., 1998 ).
Research indicates that both sexual attraction and friendship are necessary for romantic love ( Meyers and Berscheid, 1997 ; Gillath et al., 2008 ; Berscheid, 2010 ), indicating that connection which is essential for companionship plays a key role in romantic love. A study on college students by Hendrick and Hendrick (1993) found that a significant number of the students described their romantic partner as their closest friend ( Hendrick and Hendrick, 1993 ), reinforcing the importance of friendship or companionship in romantic love.
Similarity along the lines of values, goals, religion, nationality, career, culture, socioeconomic status, ethnicity, language, etc. is essential in liking and friendship in romantic love ( Berscheid and Reis, 1998 ). Research indicates that a partner who shared similar values and interests were more likely to experience stronger love ( Jin et al., 2017 ). Indeed, the more satisfied individuals were with their friendships the more similar they perceived their friends to be to themselves ( Morry, 2005 ). Also, similarity influences perceptions of familiarity ( Moreland and Zajonc, 1982 ), and familiarity plays a role in the formation of attachment and connectedness because it signals safety and security ( Bowlby, 1977 ). Moreover, similarity and familiarity affect caregiving. Sprecher and Fehr (2005) , found compassion or caregiving were lower for strangers, and greatest for dating and marital relationships, indicating that similarity and familiarity enhance intimacy and positively influences caregiving ( Sprecher and Fehr, 2005 ).
Proximity through increased exposure is known to promote liking ( Saegert et al., 1973 ), familiarity and emotional connectedness ( Sternberg, 1986 ; Berscheid, 2010 ). Exposure through fun times and direct and frequent communication is essential to maintaining and strengthening attachment and connectedness ( Sternberg and Grajek, 1984 ). In Sternberg’s triangular theory, effective communication is described as essential and affects the intimacy component of a relationship ( Sternberg, 1986 ). Indeed, intimacy grows from a combination of mutual self-disclosure and interactions mediated by positive partner responsiveness ( Laurenceau et al., 1998 , 2005 ; Manne et al., 2004 ), indicating that positive feedback and fun times together strengthens connection.
Also, sexual activity is an important component of the reward system that reinforces emotional attachment ( Seshadri, 2016 ), indicating that sexual activity may increase emotional connectedness and intimacy. Over time in most relationships, predictability grows, and sexual satisfaction becomes readily available. This weakens the erotic and emotional experience associated with romantic love ( Berscheid, 2010 ). Research shows that a reduction in novelty due to the monotony of being with the same person for a long period is the reason for this decline in sexual attraction ( Freud and Rieff, 1997 , p. 57; Sprecher et al., 2006 , p. 467). According to Sternberg (1986) , the worst enemy of the intimacy component of love is stagnation. He explained that too much predictability can erode the level of intimacy in a close relationship ( Sternberg, 1986 ). So, novelty is essential to maintaining sexual attraction and strengthening connection in romantic love.
Jealousy and separation distress which are key features of romantic love ( Fisher et al., 2002b ), are actions to maintain and protect the emotional union and are expressions of a strong connection. Research has found a significant correlation between anxiety and love ( Hatfield et al., 1989 ) and a positive link between romantic love and jealousy in stable relationships ( Mathes and Severa, 1981 ; Aune and Comstock, 1991 ; Attridge, 2013 ; Gomillion et al., 2014 ). Indeed, individuals who feel strong romantic love tend to be more jealous or sensitive to threats to their relationship ( Orosz et al., 2015 ).
Connection in romantic love is weakened by distance, a dearth of communication, unsatisfactory sexual activity, divergences or dissimilarity of values and interests, monotony and too much predictability.
Trust and Romantic Love
Trust is the belief that a partner is, and will remain, reliable or dependable ( Cook, 2003 ). Trust in romantic love fits with the intimacy, and commitment components of Sternberg’s triangular theory of love which includes being able to count on the loved one in times of need, mutual understanding with the loved one, sharing of one’s self and one’s possessions with the loved one and maintaining the relationship ( Sternberg, 1986 ).
It has been proposed that love activates specific regions in the reward system which results in a reduction in emotional judgment and fear ( Seshadri, 2016 ). This reduced fear or trust has been identified as one of the most important characteristics of a romantic relationship and essential to fidelity, commitment, monogamy, emotional vulnerability, and intimacy ( Laborde et al., 2014 ). Indeed, trust can deepen intimacy, increase commitment and increase mutual monogamy, and make a person lower their guards in the belief that they are safe from harm ( Larzelere and Huston, 1980 ; Bauman and Berman, 2005 ). People with high trust in romantic relationships tend to expect that their partner will act in their interest causing them to prioritize relationship dependence over making themselves invulnerable from harm or self-protection ( Luchies et al., 2013 ). In contrast, people with low trust in their partner tend to be unsure about whether their partner will act in their interests and prioritize insulating themselves from harm over relationship dependence ( Luchies et al., 2013 ).
Trust takes time to grow into a romantic relationship. Indeed, people in a relationship come to trust their partners when they see that their partner’s action and behavior moves the relationship forward or acts in the interest of the relationship and not themself ( Wieselquist et al., 1999 ). Research indicates that trust is associated with mutual self-disclosure ( Larzelere and Huston, 1980 ), and positive partner responsiveness which are both essential to the experience of friendship and intimacy in romantic relationships ( Larzelere and Huston, 1980 ; Reis and Shaver, 1988 ; Laurenceau et al., 1998 ).
Also, trust influences caregiving and compassion. Evidence suggests that compassion is positively related to trust ( Salazar, 2015 ). Mutual communal responsiveness or caregiving in relationships in which partners attend to one another’s needs and welfare is done because they are confident that the other will do the same when or if their own needs arise ( Clark and Monin, 2006 ). Repeated acts of communal responsiveness given with no expectation of payback provide a partner with a sense of security and trust and increase the likelihood that they will be communally responsive if or when the need arises ( Clark and Monin, 2006 ), and contributes to a sense of love in romantic relationships ( Berscheid, 2010 ).
Loss or weakening of trust could spell the end of romantic love. Indeed, mistrust corrupts intimacy and often indicates that a relationship has ended or near its end ( LaFollette and Graham, 1986 ) and it makes mutual monogamy, and commitment difficult to achieve in a romantic relationship ( Towner et al., 2015 ). A study on individuals who had fallen out of romantic love with their spouse found that loss of trust and intimacy was part of the reason for the dissolution of love ( Sailor, 2013 ).
Respect and Romantic Love
Multiple lines of evidence suggest that respect is expected in both friendships and romantic relationships ( Gaines, 1994 , 1996 ). In romantic love, it entails consideration, admiration, high regard, and value for the loved one as a part of one’s life ( Sternberg and Grajek, 1984 ; Hendrick et al., 2011 ).
Gottman (1999) , found that the basis for a stable and satisfactory marital relationship is friendship filled with fondness and admiration ( Gottman, 1999 ). Respect is considered one of the most important things married couples want from their partner ( Gottman, 1994 ). Grote and Frieze (1994) , found that respect correlates with companionate or friendship love ( Grote and Frieze, 1994 ), indicating that respect is essential to intimacy and relationship satisfaction. Also, respect is positively correlated with passion, altruism, self-disclosure, and relationship overall satisfaction ( Frei and Shaver, 2002 ; Hendrick and Hendrick, 2006 ). It is associated with the tendency to overlook a partner’s negative behavior or respond with pro-relationship actions or compassion to their shortcomings ( Rusbult et al., 1998 ; Gottman, 1999 ).
Absence or a lack of respect could spell the end of romantic love. Research indicates that there is an expectation of mutual respect in friendship and most relationships and people reacted negatively when this expectation is violated ( Hendrick et al., 2011 ), indicating that a lack of respect could negatively affect commitment and attraction. Indeed, denial of respect is an important negative behavior in friendships and most relationships ( Gaines, 1994 , 1996 ) and a lack of respect is a violation of what it means to love one ‘s partner in a close romantic relationship ( Hendrick et al., 2011 ). Gottman (1993 , 1994) identified contempt, criticism, defensiveness, and stonewalling as four of the relationally destructive behavior and he labeled them as “the four horsemen of the apocalypse.”
Romantic love summary
Romantic love involves the interactions and synergistic interplay between respect, connection, trust, and attraction. All four must be present in love. Any event that results in the loss of any of these factors could cause romantic love to gradually decline and unless effort is made to replenish it, it will eventually fade or collapse. Romantic love is dynamic and requires significant investment from both partners to keep it alive.
Parental Love
Attraction and parental love.
Attraction plays an essential role in parental love and it could be material or non-material. Material attraction involves the child’s health, gender, accomplishments or success, and attractiveness. In contrast, non-material attraction includes traits such as intelligence, character, and other personality traits.
Evidence suggests that culture influences gender preference with attraction greater for sons in most cases ( Cronk, 1993 ). Indeed, mothers and fathers have been found to favor the more intelligent and more ambitious/industrious child ( Lauricella, 2009 ). Also, parental perception that investment in a child will cost more than the benefits to be gained from taking care of the child might influence negative behavior toward the child. Indeed, multiple lines of evidence suggest that parental unemployment increases the rates of child maltreatment and abuse ( Steinberg et al., 1981 ; Lindo et al., 2013 ). Research indicates that teen mothers who have poor social support reported greater unhappiness, were at greater risk for child abuse and often employed the use of physical punishment toward their child ( Haskett et al., 1994 ; de Paúl and Domenech, 2000 ).
Also, several studies have suggested that parents tended to favor healthy children ( Mann, 1992 ; Barratt et al., 1996 ; Hagen, 1999 ). However, when resources are plentiful, parents tend to invest equally in less healthy or high-risk children ( Beaulieu and Bugental, 2008 ), because they have abundant resources to go around without compromising the reproductive value of healthy children ( Lauricella, 2009 ).
Connection and Parental Love
Connection creates a sense of oneness between parent and child and involves caregiving, intimacy, and attachment. It is influenced by proximity, positive and unique shared experiences, and similarity along virtually every dimension between parent and child.
Proximity, and similarity increases attachment and intimacy between parent and child. Research shows that parents are perceived as favoring genetically related children ( Salmon et al., 2012 ), and evidence suggests that paternal resemblance predicted paternal favoritism ( Lauricella, 2009 ). Parental proximity and similarity to a biological child are unique because it is based on genes and blood. In contrast, intimacy between a parent and an adopted child is based solely on shared experiences and proximity and takes time to grow and on many occasions may not develop ( Hooks, 1990 ; Hughes, 1999 ).
Dissimilarities or discrepancy in values, attitudes, etc., can create problems between children and parents and can have a profound effect on their relationship. Indeed, evidence suggests that the rebel child tended to be less close to the parents ( Rohde et al., 2003 ). Research has found that adolescents who are less religious than their parents tend to experience lower-quality relationships with their parents which results in higher rates of both internalizing and externalizing symptoms ( Kim-Spoon et al., 2012 ). When parents and family members were very religious, and a child comes out as an atheist, relationship quality could suffer in the form of rejection, anger, despair, or an inability to relate to one another ( Zimmerman et al., 2015 ). A study of lesbian, gay, and bisexual youngsters, for patterns of disclosure of sexual orientation to families, found that those who had disclosed reported verbal and physical abuse by parents and family members ( D’Augelli et al., 1998 ). Honor killing of female children which have been reported in Pakistan and some parts of the Middle East because of deviation from traditional gender roles or crossing of social boundaries that are deemed as taboo in their culture ( Lindsey and Sarah, 2010 ), is another example of the negative effects of the discrepancy in values between parents and child.
Unique shared experiences between parent and child could increase connection. Bank (1988) observed that the development of favoritism seems to require that the “child’s conception or birth be unusual or stressful,” ( Bank, 1988 ). Evidence suggests that parents most favored child tended to be last-born child and this is linked to their unique position, vulnerability and neediness ( Rohde et al., 2003 ). Also, proximity, positive experiences and time spent together increases connection and intimacy. Research indicates that parents tend to give more love and support to the grown child they were historically closest to and got along with ( Siennick, 2013 ). A study of primiparous women found that mothers with greater contact with their infants were more reluctant to leave them with someone else, and engaged more intimately with their child ( Klaus et al., 1972 ).
Divorce could create distance between a parent and child, weakening connection and intimacy. Indeed, one of the outcomes of divorce is the lessening of contact between divorced non-custodial fathers and their children ( Appleby and Palkovitz, 2007 ), and this can reduce intimacy ( Guttmann and Rosenberg, 2003 ).
Also, parental separation distress, worry, and concern for their child’s welfare, academic performance, and future are expressions of connection and a lack thereof is a sign of poor connection. Indeed, the levels of concern and worry expressed between children and their parents influenced their perceptions of the relationship quality ( Hay et al., 2007 ).
Trust and Parental Love
Trust is essential to parental attachment, intimacy, and caregiving. When there is mistrust, attachment and intimacy between a parent and their child are disrupted or unable to blossom. In Africa and many parts of the world, there have been reports of children being condemned and abandoned by their parents simply because they are tagged as witches with mysterious evil powers ( Tedam, 2014 ; Bartholomew, 2015 ; Briggs and Whittaker, 2018 ). The tag of “witchcraft” stirs up fear and anger, causing the child to be perceived as a deadly threat which inevitably damages attachment, intimacy and eliminates the need for caregiving.
Research has found that firstborn children were most likely to be chosen as those to whom mothers would turn when facing personal problems or crises ( Suitor and Pillemer, 2007 ). This tendency may be linked to trust. Moreover, evidence suggests that the rebel child tended to be less close to the parents ( Rohde et al., 2003 ). In other words, the more obedient, and reliable child is likely to gain the confidence and intimacy of the parents. In contrast, the disobedient and unreliable child is excluded or kept at a distance. Also, trust and poor connection could influence inheritance and disinheritance decisions. Indeed, estrangement, alienation and disaffection of a parent toward a child could result in disinheritance ( Batts, 1990 ; Brashier, 1994 , 1996 ; Foster, 2001 ; Arroyo et al., 2016 ).
Respect and Parental Love
Respect in parental love entails treating the child with consideration and regard. This consideration and regard for the child are essential to intimacy, caregiving and attachment. Indeed, respect is foundational to a harmonious relationship between parent and child ( Dixon et al., 2008 ). Evidence suggests that humans possess an innate behavioral system that leads them to form an attachment to a familiar person who provides care, comfort, and protection ( Harlow, 1958 ; Bowlby, 1989 ). Repeated acts of caregiving contribute to a sense of love in all types of relationships ( Berscheid, 2010 ), reinforcing the role of parental caregiving in fostering intimacy and attachment with the child.
Taking care of an infant’s needs, and making sure they are safe and well, all fall under consideration and regard for the child. Child abuse and neglect ( Tedam, 2014 ; Bartholomew, 2015 ; Briggs and Whittaker, 2018 ), is a display of a lack of consideration for the child’s need.
Also, respect in parental love involves admiration. Research has found that fathers treated more ambitious/industrious sons with high regard, and both parents favored the more intelligent and more ambitious/industrious daughters ( Lauricella, 2009 ) indicating that a child that engages in activities or behavior that is highly regarded by their parents may gain favor with their parents, strengthening intimacy and vice versa.
Parental love summary
Parental love involves the interactions and synergistic interplay between respect, connection, trust, and attraction. Any event that results in the loss of any of these factors could cause parental love to gradually decline. In many cases, the behavior and actions of a child significantly influence parental love.
Brand love has been defined as the level of passionate emotional attachment a satisfied or happy consumer has for a brand and evidence suggests it is very similar to interpersonal love ( Russo et al., 2011 ).
Attraction and Brand Love
Attraction plays an essential role in brand love. Material attraction for a brand includes attributes like superior design, quality, and aesthetics, price, benefits, etc. Non-material attraction involves social status symbol, brand personality, uniqueness, distinctiveness, user experience, image, etc. evidence suggests that when talking about loved brands, people often talk passionately about the brand’s many attractive qualities such as its exceptional performance, good-looking design, value for money, and other positive attributes ( Fournier, 1998 ; Whang et al., 2004 ; Carroll and Ahuvia, 2006 ; Batra et al., 2012 ). Research on brand love has found that brand attractive attributes such as prestige or uniqueness influence brand passion which affects relevant factors such as purchase intention ( Bauer et al., 2007 ).
Also, brand attraction influences brand loyalty, and commitment. Indeed, research indicates that brand benefits influences brand loyalty or commitment ( Huang et al., 2016 ). Brand personality (image, distinctiveness, and self-expressive value) is strongly associated with brand identification and loyalty ( Kim et al., 2001 ; Elbedweihy et al., 2016 ).

Connection and Brand Love
Connection is essential to brand love. It involves brand attachment, commitment, and intimacy and it is strengthened by brand identification, image, familiarity or awareness, proximity, length or frequency of usage and similarity or congruences along virtually every dimension including values, lifestyle, goals, etc. between brand and customer. Brand awareness which means brand familiarity has been described as essential for people to identify with a brand ( Pascual and Académico, 2015 ), and it indirectly affects current purchases ( Esch et al., 2006 ).
Also, brand identification promotes a sense of oneness between a brand and a customer strengthening commitment and it is driven by brand self-similarity, brand prestige and brand distinctiveness ( Stokburger-Sauer et al., 2008 ). Indeed, brand identification contributes to the development of brand love and brand loyalty ( Alnawas and Altarifi, 2016 ) and brand image and identification influence loyalty and positive word of mouth ( Carroll and Ahuvia, 2006 ; Batra et al., 2012 ; Anggraeni and Rachmanita, 2015 ). Brand identity, values and lifestyle similarities to those of the customer appear to have a strong and significant relationship with brand love ( Batra et al., 2012 ; Rauschnabel and Ahuvia, 2014 ; Alnawas and Altarifi, 2016 ; Elbedweihy et al., 2016 ). Findings from research suggest that customer-to-customer similarity and sense of community drive consumer brand identification, loyalty, and engagement ( Bergkvist and Bech-Larsen, 2010 ; Elbedweihy et al., 2016 ).
Moreover, proximity and interaction play a role in brand love. Indeed, the duration of the relationship between a customer and a brand is essential in brand love ( Albert et al., 2007 ). Fournier (1998) , discussed interdependence which involved frequent brand interactions as necessary for a strong brand relationship ( Fournier, 1998 ). Similarly, Batra et al. (2012) found that having a long-term relationship, positive emotional connection and frequent interactions with a brand was an important aspect of brand love ( Batra et al., 2012 ). Indeed, shared experiences and history between a person and a brand can increase their emotional attachment, make the brand to become an important part of the person’s identity narrative and increases their loyalty to the brand ( Thomson et al., 2005 ; Pedeliento et al., 2016 ).
Just like romantic love, concern and worry and proximity seeking, or maintenance are an expression of emotional connectedness to the brand. Indeed, anticipated separation distress has been described as a core element of brand love ( Batra et al., 2012 ), and consumers are likely to feel strong desires to maintain proximity with their loved objects, even feeling “separation distress” when they are distanced from them ( Thomson et al., 2005 ; Park et al., 2010 ).
Also, novelty through continued innovation is vital to maintaining and strengthening both attraction and connection. According to the Harvard business review, the relationship between brand and consumer go through “ruts” and to “keep the spark” alive, innovation and news are essential ( Halloran, 2014 ). Research indicates that innovation plays a role in brand equity and it impacts brand identification or resonance ( Sinha, 2017 ).
Lack of brand familiarity or awareness, poor or negative user experience, a dearth of innovation and increased dissimilarities in values and lifestyles between brand and consumer can all weaken brand connection.
Trust and Brand Love
Trust is essential to brand attachment, intimacy, and commitment. It involves confidence and reliability, or dependability of the brand and it is influenced by brand image, familiarity, values, user experience, and quality. Indeed, brand trust directly influences brand love ( Turgut and Gultekin, 2015 ; Meisenzahl, 2017 ) and a strong relationship exists between brand love and brand trust and identification ( Albert and Merunka, 2013 ). Evidence suggests that brand familiarity influences brand trust ( Ha and Perks, 2005 ) and brand trust and experience, positively influence brand attachment ( Erciş et al., 2012 ; Chinomona, 2013 ; Chinomona and Maziriri, 2017 ).
Also, brand trust affects brand purchase, loyalty, and commitment. Evidence suggests that a strong relationship exists between brand love and brand trust, brand commitment, positive word of mouth, and willingness to pay a higher price for the brand ( Albert and Merunka, 2013 ). Research indicates that brand trust positively affects brand loyalty ( Setyawan and Kussudiyarsana, 2015 ), directly influences brand purchase intentions ( Yasin and Shamim, 2013 ) and positively influences current and future purchases ( Erciş et al., 2012 ). Indeed, more than any other factor, brand trust has been identified as essential for future purchases of a brand ( Esch et al., 2006 ). It is essential in determining purchase loyalty and attitudinal loyalty and it plays a role in brand market share ( Chaudhuri and Holbrook, 2001 ). Brand trust affects both affective and continuance commitment and affective commitment influences repurchase intention and loyalty ( Erciş et al., 2012 ).
Brand quality is essential to brand trust and love. Indeed, Fournier (1998) , discussed the role of brand quality in brand love and highlighted the role of trust in relationship satisfaction and strength ( Fournier, 1998 ). Also, brand trust has been found to positively affect resistance to negative information and repurchase intention ( Turgut and Gultekin, 2015 ).
Brand trust is weakened by poor user experience, brand quality, brand image, and a lack of brand familiarity.
Respect and Brand Love
Brand respect is essential in brand love and plays an important role in brand attachment, intimacy, and commitment. It is influenced by brand identification, values, image, experience, and quality. Brand respect is displayed by the customer in the form of high regard, admiration for the brand, brand loyalty and consideration or tolerance of negative information. Indeed, brand familiarity positively affects brand respect ( Zhou, 2017 ), indicating that brand familiarity increases regard for a brand. Evidence suggests that brand image positively influences brand respect and love ( Cho, 2011 ), indicating that brand image modulates a customer’s regard and admiration for a brand.
Brand respect influences brand commitment and loyalty. Indeed, a strong relationship has been found between brand respect and brand loyalty ( Cho, 2011 ) and brand admiration results in greater brand loyalty, stronger brand advocacy, and higher brand equity ( Park et al., 2016 ). Brand respect affects the behavioral outcomes of brand love such as affective commitment, and willingness to pay a price premium ( Garg et al., 2016 ; Park et al., 2016 ).
Also, evidence suggests that customers’ admiration or high regard for a brand contributes to why they tend to ignore negative information about the brand ( Elbedweihy et al., 2016 ). Fournier (1998) , included respect as one of the components of brand partner quality. This means that respect is one of the factors that reflects the consumer’s evaluation of the brand’s performance ( Fournier, 1998 ).
A lack of respect could negatively influence the relationship between a brand and a customer. Indeed, people react negatively when the expectation of respect is violated ( Hendrick et al., 2011 ) and a violation of expectation between brand and customer has been found to contribute to brand hate ( Zarantonello et al., 2016 ).
Brand love summary
Brand love involves the interactions and synergistic interplay between respect, connection, trust, and attraction. Any event that results in the loss of any of these factors could cause brand love to gradually decline and unless effort is made to replenish it, it will eventually fade or collapse. Brand love is dynamic and requires significant investment from the brand to keep it alive.
Strengths and Advances Made by the Quadruple Theory
The quadruple theory builds on many of the strengths of previous theories of love and it applies a temporal approach that has been proposed as the best way to understand love ( Berscheid, 2010 ). It goes further than previous theories for several reasons. Firstly, it could potentially be applied to any form of love although, only brand, romantic and parental love were discussed in this paper due to the paucity of scholarly articles on other forms of love. One of the reasons current love scales and approaches have been unable to be applied in all forms of love ( Hendrick and Hendrick, 1989 ; Whitley, 1993 ; Sternberg, 1997 ; Masuda, 2003 ; Graham and Christiansen, 2009 ), is because they capture only a part of the ACC model, unlike the quadruple framework which fully captures it.
Unlike previous theories, the quadruple theory’s application of the complex factor of connection/resonance gives it an edge in furthering our understanding of love. Proximity, positive shared experience, familiarity, and similarity are vital to connection and connection has the most profound influence on all the other factors.
Also, the dynamism and variation of these factors provide a fresh way to understand love from its development to collapse. As Figure 1 shows, love tends to take time to mature in a relationship and can die as these factors rise and decline. Figure 1 shows that variations in the presence of these factors represent different levels of love. Love in any relationship is influenced by the events in the environment it is embedded, and it responds favorably or negatively to these changes. Indeed, people get sick, old, lose their finances, travel in search of greener pastures creating distance, develop new interests different from their partner’s and all these influences the presence and absence of love. One brand becomes more innovative, improves its product quality and users experience over another and people gradually love it more than the one they previously loved. In other words, love is very dynamic and may be divided into high, moderate and low. Another point highlighted in Figure 1 is that the absence of one factor represents the absence of love and only the presence of all factors represents the presence of love. Indeed, the decline of a factor can be replenished in response to changes in the environment causing the reestablishment of love. Trust could decline but attraction and respect remain and over time trust could be replenished.
This dynamic understanding of love implies that it can be nurtured and sustained. As an example, for a brand to be loved and to maintain that love, it must make products that are attractive (appealing). It must be able to connect to its target customers by reaching out through adverts to achieve familiarity and it must ensure that its values, goals, actions are consistently similar to those of its customer base. Also, it must ensure its services and products and actions promote and maintain trust with its customers. It must respect (value) its customer’s interests and ensure that its services and products continue to receive the admiration of its customers. Table 2 describes how brand love can be nurtured and preserved.

Table 2. Brand love can be nurtured and maintained.
Using this framework, a love scale or algorithm could be developed to ascertain the presence or absence of love in any relationship. Such a scale must effectively capture these four factors and must consider the type of love being calculated in its approach. As an example, in trying to create a scale for romantic love, sexual attraction, and activity may be important for attraction and connection (depending on the age of the partners) but would be unnecessary in the calculation of brand or parental love.
Major Challenges for the Theory
One of the biggest challenges the theory faces is the lack of psychometric data to prove many of its claims. Most of its arguments are based on decades of psychological data, but its lack of psychometric data weakens the theory significantly. Also, the entire premise of the theory is based on the ACC model, which has not been validated as essential or foundational to understanding love. Perhaps, something else needs to be added to the model that the theory may have missed. The argument that the quadruple theory captures the ACC model better than previous theories on love is an argument that has not been validated, and it remains to be seen if this is true. Also, the argument that it can be applied to all forms of love apart from the three discussed remains to be tested and verified.
Gaps currently exist in our understanding of love and evidences from the existing literature show that a framework that can be applied to all forms of love is needed. The quadruple theory hopes to be that framework. It is likely to broaden our understanding of the complex nature of love. It could make love less complex by making it something that can be cultivated or nurtured, regulated and preserved. Future research should consider the modulatory roles of peptides, neurotransmitters, and hormones on these factors and their influence on love as well as the integrated parts of the brain that modulates all these factors and how they work synergistically in different stages of love.
It is important to note that love is universal and applies to people of all cultures, races, ethnicities, religion and sexual orientations. Indeed, romantic love as described by the quadruple theory applies equally to heterosexual relationships and to the relationships of people in the LGTBQ community.
In conclusion, culture has a monumental influence on what people feel, think, and how they behave toward other people and things in their environment ( Karandashev, 2015 ; Ching Hei and David, 2018 ). So, it can be considered a modulating factor on the factors discussed and on love.
Author Contributions
The author confirms being the sole contributor of this work and has approved it for publication.
Conflict of Interest
The author declares that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Agnew, C. R., Van Lange, P. A. M., Rusbult, C. E., and Langston, C. A. (1998). Cognitive interdependence: commitment and the mental representation of close relationships. J. Pers. Soc. Psychol. 74, 939–954. doi: 10.1037/0022-3514.74.4.939
CrossRef Full Text | Google Scholar
Ainsworth, M. D. (1985). Attachments across the life span. Bull. N. Y. Acad. Med. 61, 792–812.
Google Scholar
Albert, N., and Merunka, D. (2013). The role of brand love in consumer-brand relationships. J. Consum. Mark. 30, 258–266. doi: 10.1108/07363761311328928
Albert, N., Merunka, D., and Valette-Florence, P. (2007). When consumers love their brands: exploring the concept and its dimensions. J. Bus. Res. 61, 1062–1075. doi: 10.1016/j.jbusres.2007.09.014
Ali, S. H. S., Mansur, N., and Abdullah, Z. (2012). Analyzing the issue of respect and trust: determining the mediating role of religion. Procedia Soc. Behav. Sci. 58, 614–623. doi: 10.1016/J.SBSPRO.2012.09.1039
Alnawas, I., and Altarifi, S. (2016). Exploring the role of brand identification and brand love in generating higher levels of brand loyalty. J. Vacat. Mark. 22, 111–128. doi: 10.1177/1356766715604663
Alper, G. (2004). Voices from the unconscious. J. Loss Trauma 10, 73–81. doi: 10.1080/15325020490890660
Amato, P. R., and Rogers, S. J. (1997). A longitudinal study of marital problems and subsequent divorce. J. Marriage Fam. 59, 612–624. doi: 10.2307/353949
Anggraeni, A., and Rachmanita. (2015). Effects of brand love, personality and image on word of mouth; the case of local fashion brands among young consumers. Procedia Soc. Behav. Sci. 211, 442–447. doi: 10.1016/J.SBSPRO.2015.11.058
Appleby, D. W., and Palkovitz, R. (2007). Factors Influencing a Divorced Father’ s Involvement with His Children. Available online at: http://digitalcommons.liberty.edu/ccfs_fac_pubs/7 (accessed February 22, 2020).
Aron, A., Fisher, H., Mashek, D. J., Strong, G., Li, H., and Brown, L. L. (2005). Reward, motivation, and emotion systems associated with early-stage intense romantic love. J. Neurophysiol. 94, 327–337. doi: 10.1152/jn.00838.2004
PubMed Abstract | CrossRef Full Text | Google Scholar
Arroyo, E., Amayuelas, I., and Amorós, E. F. (2016). Kinship bonds and emotional ties: lack of a family relationship as ground for disinheritance. Eur. Rev. Priv. Law 2, 203–222.
Attridge, M. (2013). Jealousy and relationship closeness. SAGE Open 3:215824401347605. doi: 10.1177/2158244013476054
Aune, K. S., and Comstock, J. (1991). Experience and expression of jealousy: comparison between friends and romantics. Psychol. Rep. 69, 315–319. doi: 10.2466/pr0.1991.69.1.315
Bank, S. P. (1988). Favoritism. J. Child. Contemp. Soc. 19, 77–89. doi: 10.1300/J274v19n03_05
Barratt, M. S., Roach, M. A., and Leavitt, L. A. (1996). The impact of low-risk prematurity on maternal behaviour and toddler outcomes. Int. J. Behav. Dev. 19, 581–602. doi: 10.1177/016502549601900308
Bartels, A., and Zeki, S. (2000). The neural basis of romantic love. Neuroreport 11, 3829–3834.
PubMed Abstract | Google Scholar
Bartholomew, L. (2015). Child abuse linked to beliefs in witchcraft. Trans. Soc. Rev. 5, 193–198. doi: 10.1080/21931674.2015.1028809
Batool, S., and Malik, N. I. (2010). Role of attitude similarity and proximity in interpersonal attraction among friends. Int. J. Innov. Manage. Technol. 1.
Batra, R., Ahuvia, A., and Bagozzi, R. P. (2012). Brand love. J. Mark. 76, 1–16. doi: 10.1509/jm.09.0339
Batts, D. A. (1990). I Didn’t ask to be born: the American law of disinheritance and a proposal for change to a sytem of protected inheritance recommended citation. Hastings L. J. 41, 1197–1270.
Bauer, H. H., Heinrich, D., and Martin, I. (2007). “How to create high emotional consumer-brand relationships? The causalities of brand passion,” in Proceedings of the Australian and New Zealand Marketing Academy (ANZMAC) Conference 2007 , Dunedin, 2189–2198.
Bauman, L. J., and Berman, R. (2005). Adolescent relationships and condom use: trust, love and commitment. AIDS Behav. 9, 211–222. doi: 10.1007/s10461-005-3902-2
Beaulieu, D. A., and Bugental, D. (2008). Contingent parental investment: an evolutionary framework for understanding early interaction between mothers and children. Evol. Hum. Behav. 29, 249–255. doi: 10.1016/j.evolhumbehav.2008.01.002
Beauregard, M., Courtemanche, J., Paquette, V., and St-Pierre, É. L. (2009). The neural basis of unconditional love. Psychiatry Res. Neuroimaging 172, 93–98. doi: 10.1016/j.pscychresns.2008.11.003
Beckes, L., Coan, J. A., and Hasselmo, K. (2013). Familiarity promotes the blurring of self and other in the neural representation of threat. Soc. Cogn. Affect. Neurosci. 8, 670–677. doi: 10.1093/scan/nss046
Bergkvist, L., and Bech-Larsen, T. (2010). Two studies of consequences and actionable antecedents of brand love. J. Brand Manage. 17, 504–518. doi: 10.1057/bm.2010.6
Berscheid, E. (2010). Love in the fourth dimension. Annu. Rev. Psychol. 61, 1–25. doi: 10.1146/annurev.psych.093008.100318
Berscheid, E., and Hatfield, E. (1978). Interpersonal Attraction. Boston, MA: Addison-Wesley Pub. Co.
Berscheid, E. A., and Reis, H. T. (1998). “Attraction and close relationships,” in The Handbook of Social Psychology , 4th Edn, Vol. 2, eds D. T. Gilbert, S. T. Fiske, and G. Lindzey (Boston, MA: McGraw-Hill), 193–281.
Bidmon, S. (2017). How does attachment style influence the brand attachment – brand trust and brand loyalty chain in adolescents? Int. J. Advert. 36, 164–189. doi: 10.1080/02650487.2016.1172404
Bowlby, J. (1973). “Affectional bonds: their nature and origin,” in Loneliness: The Experience of Emotional and Social Isolation , ed. R. S. Weiss (Cambridge, MA: MIT Press), 38–52.
Bowlby, J. (1977). The making and breaking of affectional bonds: aetiology and psychopathology in light of attachment theory. Br. J. Psychiatry 130, 201–210. doi: 10.1136/bmj.a3133
Bowlby, J. (1988). A SECURE BASE Parent-Child Attachment and Healthy Human Development A Member of the. New York, NY: Perseus Books Group.
Bowlby, J. (1989). The Making & Breaking of Affectional Bonds. London: Routledge.
Brashier, R. C. (1994). Disinheritance and the modern family. Case West. Reserve L. Rev. 83:121.
Brashier, R. C. (1996). Protecting the child from disinheritance: Must Louisiana stand alone? Repository citation protecting the child from disinheritance: Must Louisiana Stand Alone? Louis. L. Rev. 57.
Braxton-Davis, P. (2010). The social psychology of love and attraction. McNair Sch. J. 14, 5–12.
Bretherton, I. (1992). The origins of attachment theory: John Bowlby and Mary Ainsworth. Dev. Psychol. 28, 759–775. doi: 10.1037/0012-1649.28.5.759
Briggs, S., and Whittaker, A. (2018). Protecting Children from Faith-Based Abuse through Accusations of Witchcraft and Spirit Possession: Understanding Contexts and Informing Practice. Br. J. Soc. Work 48, 2157–2175. doi: 10.1093/bjsw/bcx155
Brislin, R. W., and Lewis, S. A. (1968). Dating and physical attractiveness: replication. Psychol. Rep. 22, 976–976. doi: 10.2466/pr0.1968.22.3.976
Burgess, E. W., and Wallin, P. (1954). Courtship, Engagement, and Marriage , 1st Edn. New York, NY: Lippincott.
Burkett, J. P., and Young, L. J. (2012). The behavioral, anatomical and pharmacological parallels between social attachment, love and addiction. Psychopharmacology 224, 1–26. doi: 10.1007/s00213-012-2794-x
Buss, D. M., and Barnes, M. (1986). Preferences in human mate selection. J. Pers. Soc. Psychol. 50, 559–570. doi: 10.1037/0022-3514.50.3.559
Byrne, D., and Griffitt, W. (1973). Interpersonal attraction. Annu. Rev. Psychol. 24, 317–336. doi: 10.1146/annurev.ps.24.020173.001533
Byrne, D. E. (1971). The Attraction Paradigm. New York, NY: Academic Press.
Cacioppo, J. T., Berntson, G. G., Lorig, T. S., Norris, C. J., Rickett, E., and Nusbaum, H. (2003). Just because you’re imaging the brain doesn’t mean you can stop using your head: a primer and set of first principles. J. Pers. Soc. Psychol. 85, 650–661. doi: 10.1037/0022-3514.85.4.650
Canterberry, M., and Gillath, O. (2012). Attachment and Caregiving Functions, Interactions, and Implications. Available online at: https://gillab.ku.edu/sites/gillab.drupal.ku.edu/files/docs/canterberrygillathchp14.pdf (accessed February 22, 2020).
Carnelley, K. B., Pietromonaco, P. R., and Jaffe, K. (1996). Attachment, caregiving, and relationship functioning in couples: Effects of self and partner. Pers. Relat. 3, 257–278. doi: 10.1111/j.1475-6811.1996.tb00116.x
Carroll, B. A., and Ahuvia, A. C. (2006). Some antecedents and outcomes of brand love. Mark. Lett. 17, 79–89. doi: 10.2307/40216667
Carter, C. S. (1998). Neuroendocrine perspectives on social attachment and love. Psychoneuroendocrinology 23, 779–818.
Chaudhuri, A., and Holbrook, M. B. (2001). The chain of effects from brand trust and brand affect to brand performance: the role of brand loyalty. J. Mark. 65, 81–93. doi: 10.1509/jmkg.65.2.81.18255
Ching Hei, K., and David, M. K. (2018). How love is perceived by malaysian malay children. Int. J. Linguist. Lit. Transl. 1, 80–104.
Chinomona, E., and Maziriri, E. (2017). The influence of brand trust, brand familiarity and brand experience on brand attachment: a case of consumers in the Gauteng Province of South Africa. J. Econ. Behav. Stud. 9, 69–81.
Chinomona, R. (2013). The influence of brand experience on brand satisfaction, Trust And Attachment In South Africa. Int. Bus. Econ. Res. J. 12, 1303–1316. doi: 10.19030/iber.v12i10.8138
Cho, E. (2011). Development of a Brand Image Scale and the Impact of Lovemarks on Brand Equity. Ph.D. dissertation, Iowa State University, Ames, IA.
Clark, M. S., and Mills, J. (1979). Interpersonal attraction in exchange and communal relationships. J. Pers. Soc. Psychol. 37, 12–24. doi: 10.1037/0022-3514.37.1.12
Clark, M. S., and Monin, J. K. (2006). “Giving and receiving communal responsiveness as love,” in The New Psychology of Love , eds R. J. Sternberg and K. Weis (New Haven, CT: Yale University Press), 200–221.
Collins, N. L., and Feeney, B. C. (2000). A safe haven: an attachment theory perspective on support seeking and caregiving in intimate relationships. J. Pers. Soc. Psychol. 78, 1053–1073.
Collisson, B., and Howell, J. L. (2014). The liking-similarity effect: perceptions of similarity as a function of liking. J. Soc. Psychol. 154, 384–400. doi: 10.1080/00224545.2014.914882
Cook, K. S. (2003). Trust in Society. New York, NY: Russell Sage Foundation.
Costa, D. L., and Kahn, M. E. (2003a). Civic engagement and community heterogeneity: an economist’s perspective. Perspect. Polit. 1, 103–111. doi: 10.1017/S1537592703000082
Costa, D. L., and Kahn, M. E. (2003b). Understanding the American Decline in Social Capital, 1952-1998. Kyklos 56, 17–46. doi: 10.1111/1467-6435.00208
Cronk, L. (1993). Parental favoritism toward daughters. Am. Sci. 81, 272–279. doi: 10.2307/29774922
D’Augelli, A. R., Hershberger, S. L., and Pilkington, N. W. (1998). Lesbian, gay, and bisexual youth and their families: disclosure of sexual orientation and its consequences. Am. J. Orthopsychiatry 68, 361–371.
De Boer, A., Van Buel, E. M., and Ter Horst, G. J. (2012). Love is more than just a kiss: a neurobiological perspective on love and affection. Neuroscience 201, 114–124. doi: 10.1016/j.neuroscience.2011.11.017
de Paúl, J., and Domenech, L. (2000). Childhood history of abuse and child abuse potential in adolescent mothers: a longitudinal study. Child Abuse Negl. 24, 701–713.
Dew, J. P., and Dakin, J. (2011). Financial disagreements and marital conflict tactics. J. Financial Ther. 2:7. doi: 10.4148/jft.v2i1.1414
Dixon, S. V., Graber, J. A., and Brooks-Gunn, J. (2008). The roles of respect for parental authority and parenting practices in parent-child conflict among African American, Latino, and European American families. J. Fam. Psychol. 22, 1–10. doi: 10.1037/0893-3200.22.1.1
Elbedweihy, A. M., Jayawardhena, C., Elsharnouby, M. H., and Elsharnouby, T. H. (2016). Customer relationship building: the role of brand attractiveness and consumer–brand identification. J. Bus. Res. 69, 2901–2910. doi: 10.1016/j.jbusres.2015.12.059
Erciş, A., Ünal, S., Candan, F. B., and Yıldırım, H. (2012). The effect of brand satisfaction, trust and brand commitment on loyalty and repurchase intentions. Procedia Soc. Behav. Sci. 58, 1395–1404. doi: 10.1016/j.sbspro.2012.09.1124
Esch, F., Langner, T., Schmitt, B. H., and Geus, P. (2006). Are brands forever? How brand knowledge and relationships affect current and future purchases. J. Prod. Brand Manage. 15, 98–105. doi: 10.1108/10610420610658938
Esch, T., and Stefano, G. B. (2005). The neurobiology of love. Neuroendocrinol. Lett. 26, 175–192. doi: 10.2174/157340005774575037
Feeney, B. C., and Collins, N. L. (2001). Predictors of caregiving in adult Intimate relationships: an attachment theoretical perspective. J. Pers. Soc. Psychol. 80, 972–994. doi: 10.1037/0022-3514.80.6.972
Feeney, J. A., and Noller, P. (1990). Attachment Style as a Predictor of Adult Romantic Relationships. J. Pers. Soc. Psychol. 58, 281–291. doi: 10.1016/j.psychres.2018.01.010
Fehr, B. (1994). Prototype-based assessment of laypeople’s views of love. Pers. Relat. 1, 309–331. doi: 10.1111/j.1475-6811.1994.tb00068.x
Feldman, R. (2017). The neurobiology of human attachments. Trends Cogn. Sci. 21, 80–99. doi: 10.1016/j.tics.2016.11.007
Fisher, H. (2005). Why We Love: The Nature and Chemistry of Romantic Love. New York, NY: Henry Holt and Co.
Fisher, H., Aron, A., and Brown, L. L. (2005). Romantic love: an fMRI study of a neural mechanism for mate choice. J. Comp. Neurol. 493, 58–62. doi: 10.1002/cne.20772
Fisher, H. E., Aron, A., and Brown, L. L. (2006). Romantic love: a mammalian brain system for mate choice. Philos. Trans. R. Soc. Lond. Ser. B Biol. Sci. 361, 2173–2186. doi: 10.1098/rstb.2006.1938
Fisher, H. E., Aron, A., Mashek, D., Li, H., Strong, G., and Brown, L. L. (2002a). The neural mechanisms of mate choice: a hypothesis. Neuro Endocrinol. Lett. 23(Suppl. 4), 92–97.
Fisher, H. E., Aron, A., Mashek, D., Li, H., and Brown, L. L. (2002b). Defining the brain systems of lust, romantic attraction, and attachment. Arch. Sex. Behav. 31, 413–419.
Fisher, H. E., Brown, L. L., Aron, A., Strong, G., and Mashek, D. (2010). Reward, addiction, and emotion regulation systems associated with rejection in love. J. Neurophysiol. 104, 51–60. doi: 10.1152/jn.00784.2009
Fitzpatrick, J., and Lafontaine, M.-F. (2017). Attachment, trust, and satisfaction in relationships: investigating actor, partner, and mediating effects. Pers. Relat. 24, 640–662. doi: 10.1111/pere.12203
Foster, F. H. (2001). The family paradigm of inheritance law, 80 N.C. N. C. L. Rev. 80, 12–13.
Fournier, S. (1998). Consumers and their brands: developing relationship theory in consumer research. J. Consum. Res. 24, 343–373.
Frei, J. R., and Shaver, P. R. (2002). Respect in close relationships: prototype definition, self-report assessment, and initial correlates. Pers. Relat. 9, 121–139. doi: 10.1111/1475-6811.00008
Freud, S., and Rieff, P. (1997). Sexuality and the Psychology of Love. New York, NY: Collier Books.
Gaines, S. O. (1994). Exchange of respect-denying behaviors among male-female friendships. J. Soc. Pers. Relat. 11, 5–24. doi: 10.1177/0265407594111001
Gaines, S. O. (1996). Impact of interpersonal traits and gender-role compliance on interpersonal resource exchange among dating and engaged/married couples. J. Soc. Pers. Relat. 13, 241–261. doi: 10.1177/0265407596132005
Garg, R., Mukherjee, J., Biswas, S., and Kataria, A. (2016). An investigation into the concept of brand love and its proximal and distal covariates. J. Relat. Mark. 15, 135–153. doi: 10.1080/15332667.2016.1209047
Giles, J. (2015). Sexual attraction: the psychology of allure. Praeger 351, 23–25.
Gillath, O., Mikulincer, M., Birnbaum, G. E., and Shaver, P. R. (2008). When sex primes love: subliminal sexual priming motivates relationship goal pursuit. Pers. Soc. Psychol. Bull. 34, 1057–1069. doi: 10.1177/0146167208318141
Gomillion, S., Gabriel, S., and Murray, S. L. (2014). A friend of yours is no friend of mine. Soc. Psychol. Pers. Sci. 5, 636–643. doi: 10.1177/1948550614524447
Gottman, J. (1993). A theory of marital dissolution and stability. J. Fam. Psychol. 7, 57–75. doi: 10.1037/0893-3200.7.1.57
Gottman, J. (1994). What Predicts Divorce?: The Relationship Between Marital Processes and Marital Outcomes. Hillsdale, NJ: Lawrence Erlbaum Associates.
Gottman, J. M. (1999). The Marriage Clinic: A Scientifically-Based Marital Therapy. New York, NY: W.W. Norton.
Grabill, C. M., and Kent, K. A. K. (2000). Attachment style and intimacy in friendship. Pers. Relat. 7, 363–378.
Graham, J. M., and Christiansen, K. (2009). The reliability of romantic love: a reliability generalization meta-analysis. Pers. Relat. 16, 49–66. doi: 10.1111/j.1475-6811.2009.01209.x
Grant-Jacob, J. A. (2016). Love at first sight. Front. Psychol. 7:1113. doi: 10.3389/fpsyg.2016.01113
Grote, N. K., and Frieze, I. H. (1994). The measurement of friendship-based love in intimate relationships. Pers. Relat. 1, 275–300. doi: 10.1111/j.1475-6811.1994.tb00066.x
Gu, R., Huang, W., Camilleri, J., Xu, P., Wei, P., Eickhoff, S. B., et al. (2019). Love is analogous to money in human brain: COORDINATE-based and functional connectivity meta-analyses of social and monetary reward anticipation. Neurosci. Biobehav. Rev. 100, 108–128. doi: 10.1016/j.neubiorev.2019.02.017
Guéguen, N., and Lamy, L. (2012). Men’s social status and attractiveness. Swiss J. Psychol. 71, 157–160. doi: 10.1024/1421-0185/a000083
Guttmann, J., and Rosenberg, M. (2003). Emotional intimacy and children’s adjustment: a comparison between single-parent divorced and intact families. Educ. Psychol. 23, 457–472. doi: 10.1080/01443410303213
Ha, H.-Y., and Perks, H. (2005). Effects of consumer perceptions of brand experience on the web: brand familiarity, satisfaction and brand trust. J. Consum. Behav. 4, 438–452. doi: 10.1002/cb.29
Ha, T., Overbeek, G., and Engels, R. C. M. E. (2010). Effects of attractiveness and social status on dating desire in heterosexual adolescents: an experimental study. Arch. Sex. Behav. 39, 1063–1071. doi: 10.1007/s10508-009-9561-z
Hagen, E. (1999). The functions of postpartum depression. Evol. Hum. Behav. 20, 325–359.
Halloran, T. (2014). The Eight Phases of Brand Love. Available online at: https://hbr.org/2014/02/the-eight-phases-of-brand-love (accessed February 22, 2020).
Harlow, H. F. (1958). Classics in the History of Psychology. New York, NY: York University.
Haskett, M. E., Johnson, C. A., and Miller, J. W. (1994). Individual differences in risk of child abuse by adolescent mothers: assessment in the perinatal period. J. Child Psychol. Psychiatry 35, 461–476.
Hatfield, E., Brinton, C., and Cornelius, J. (1989). Passionate love and anxiety in young adolescents. Motiv. Emot. 13, 271–289. doi: 10.1007/BF00995539
Hatfield, E., Cacioppo, J. T., and Rapson, R. L. (1994). Emotional contagion. Curr. Dir. Psychol. Sci. 2, 96–99. doi: 10.1111/1467-8721.ep10770953
Hatfield, E., and Sprecher, S. (1986). Measuring passionate love in intimate relationships. J. Adolesc. 9, 383–410.
Hay, E. L., Fingerman, K. L., and Lefkowitz, E. S. (2007). The experience of worry in parent–adult child relationships. Pers. Relat. 14, 605–622. doi: 10.1111/j.1475-6811.2007.00174.x
Hazan, C., and Shaver, P. (1987). Romantic love conceptualized as an attachment process. J. Pers. Soc. Psychol. 52, 511–524.
Hendrick, C., and Hendrick, S. (1986). A theory and method of love. J. Pers. Soc. Psychol. 50, 392–402. doi: 10.1037/0022-3514.50.2.392
Hendrick, C., and Hendrick, S. S. (1989). Research on love: Does it measure up? J. Pers. Soc. Psychol. 56, 784–794.
Hendrick, C., Hendrick, S. S., and Zacchilli, T. L. (2011). Respect and love in romantic relationships. Actas Investig. Psicol. 1, 316–329.
Hendrick, S. S., and Hendrick, C. (1993). Lovers as friends. J. Soc. Pers. Relat. 10, 459–466. doi: 10.1177/0265407593103011
Hendrick, S. S., and Hendrick, C. (2006). Measuring respect in close relationships. J. Soc. Pers. Relat. 23, 881–899. doi: 10.1177/0265407506070471
Hendrick, S. S., Hendrick, C., and Logue, E. M. (2010). Respect and the family. J. Fam. Theory Rev. 2, 126–136. doi: 10.1111/j.1756-2589.2010.00046.x
Honari, B., and Saremi, A. A. (2015). The study of relationship between attachment styles and obsessive love style. Procedia Soc. Behav. Sci. 165, 152–159. doi: 10.1016/J.SBSPRO.2014.12.617
Hooks, P. J. (1990). The real mother-issues in adoption. Jefferson J. Psychiatry 8:8. doi: 10.29046/JJP.008.2.005
Huang, S.-M., Fang, S.-R., Fang, S.-C., and Huang, C.-C. (2016). The influences of brand benefits on brand loyalty: intermediate mechanisms. Aust. J. Manage. 41, 141–160. doi: 10.1177/0312896214553516
Hughes, D. A. (1999). Adopting children with attachment problems. Child Welf. 78, 541–560.
Jin, W., Xiang, Y., and Lei, M. (2017). The deeper the love, the deeper the hate. Front. Psychol. 8:1940. doi: 10.3389/fpsyg.2017.01940
Karandashev, V. (2015). Unit 5 social psychology and culture subunit 4 interpersonal and intergroup relations article 2 6-1-2015 recommended citation Karandashev. Online Read. Psychol. Cult. 5. doi: 10.9707/2307-0919.1135
Karandashev, V., and Fata, B. (2014). Change in physical attraction in early romantic relationships. Interpers. Int. J. Pers. Relatsh. 8, 257–267. doi: 10.5964/ijpr.v8i2.167
Kim, C. K., Han, D., and Park, S.-B. (2001). The effect of brand personality and brand identification on brand loyalty: applying the theory of social identification. Jpn. Psychol. Res. 43, 195–206. doi: 10.1111/1468-5884.00177
Kim-Spoon, J., Longo, G. S., and McCullough, M. E. (2012). Adolescents who are less religious than their parents are at risk for externalizing and internalizing symptoms: the mediating role of parent-adolescent relationship quality. J. Fam. Psychol. 26, 636–641. doi: 10.1037/a0029176
Klaus, M. H., Jerauld, R., Kreger, N. C., McAlpine, W., Steffa, M., and Kennell, J. H. (1972). Maternal attachment. N. Engl. J. Med. 286, 460–463. doi: 10.1056/NEJM197203022860904
Kunce, L. J., and Shaver, P. R. (1994). “An attachment-theoretical approach to caregiving in romantic relationships,” in Advances in Personal Relationships, Attachment Processes in Adulthood , Vol. 5, eds Bartholomew and D. Perlman (London: Jessica Kingsley Publishers), 205–237.
Laborde, N. D., vanDommelen-Gonzalez, E., and Minnis, A. M. (2014). Trust - that’s a big one: intimate partnership values among urban Latino youth. Cult. Health Sex. 16, 1009–1022. doi: 10.1080/13691058.2014.921837
LaFollette, H., and Graham, G. (1986). Honesty and intimacy. J. Soc. Pers. Relat. 3, 3–18. doi: 10.1177/0265407586031001
Larzelere, R. E., and Huston, T. L. (1980). The dyadic trust scale: toward understanding interpersonal trust in close relationships. J. Marriage Fam. 42, 595–604. doi: 10.2307/351903
Laurenceau, J.-P., Barrett, L. F., and Rovine, M. J. (2005). The interpersonal process model of intimacy in marriage: a daily-diary and multilevel modeling approach. J. Fam. Psychol. 19, 314–323. doi: 10.1037/0893-3200.19.2.314
Laurenceau, J.-P., Feldman Barrett, L., and Pietromonaco, P. R. (1998). Intimacy as an interpersonal process& quot; the importance of self-disclosure, partner disclosure, and perceived partner responsiveness in interpersonal exchanges. J. Pers. Soc. Psychol. 74, 1238–1251.
Lauricella, A. M. (2009). Why do Mommy and Daddy Love You More? An Investigation of Parental Favoritism from an Evolutionary Perspective. Available online at: https://etd.ohiolink.edu/rws_etd/document/get/bgsu1250869200/inline (accessed February 22, 2020).
Lindo, J. M., Schaller, J., and Hansen, B. (2013). Economic Downturns and Child Abuse. NBER Working Paper No. 18994. Cambridge, MA: National Bureau of Economic Research.
Lindsey, D., and Sarah, B. (2010). Interpreting honor crimes: the institutional disregard towards female victims of family violence in the Middle East. Int. J. Criminol. Sociol. Theory 3.
Luchies, L. B., Rusbult, C. E., Kumashiro, M., Eastwick, P. W., Coolsen, M. K., and Finkel, E. J. (2013). Trust and biased memory of transgressions in romantic relationships. J. Pers. Soc. Psychol. 104, 673–694. doi: 10.1037/a0031054
Luhmann, N. (1979). Trust and Power. New York, NY: John Wiley & Sons.
Luo, S., and Zhang, G. (2009). What leads to romantic attraction: similarity. Reciprocity, security, or beauty? Evidence from a speed-dating study. J. Personal. 77, 933–964. doi: 10.1111/j.1467-6494.2009.00570.x
Lutz-Zois, C. J., Bradley, A. C., Mihalik, J. L., and Moorman-Eavers, E. R. (2006). Perceived similarity and relationship success among dating couples: an idiographic approach. J. Soc. Pers. Relat. 23, 865–880. doi: 10.1177/0265407506068267
Mann, J. (1992). “Nurturance or negligence: maternal psychology and behavioral preference among preterm twins,” in The Adapted Mind , eds J. Barkow, L. Cosmides, and J. Tooby (New York, NY: Oxford University Press), 367–390.
Manne, S., Ostroff, J., Rini, C., Fox, K., Goldstein, L., and Grana, G. (2004). The interpersonal process model of intimacy: the role of self-disclosure, partner disclosure, and partner responsiveness in interactions between breast cancer patients and their partners. J. Fam. Psychol. 18, 589–599. doi: 10.1037/0893-3200.18.4.589
Masuda, M. (2003). Meta-analyses of love scales: Do various love scales measure the same psychological constructs? Jpn. Psychol. Res. 45, 25–37. doi: 10.1111/1468-5884.00030
Mathes, E. W., and Severa, N. (1981). Jealousy, romantic love, and liking: theoretical considerations and preliminary scale development. Psychol. Rep. 49, 23–31. doi: 10.2466/pr0.1981.49.1.23
McKelvie, S. J., and Matthews, S. J. (1976). Effects of physical attractiveness and favourableness of character on liking. Psychol. Rep. 38, 1223–1230. doi: 10.2466/pr0.1976.38.3c.1223
Meisenzahl, J. (2017). Correlation of Brand Experience and Brand Love Using the Example of FlixBus. Master’s thesis, Seinajok University of Applied Sciences, Seinäjoki.
Meyers, S. A., and Berscheid, E. (1997). The language of love: the difference a preposition makes. Pers. Soc. Psychol. Bull. 23, 347–362. doi: 10.1177/0146167297234002
Mikulincer, M. (2006). “Attachment, caregiving, and sex within romantic relationships a behavioral systems perspective,” in Dynamics of Romantic Love: Attachment, Caregiving, and Sex , eds M. Mikulincer, and G. S. Goodman (New York, NY: Guilford Publications), 23–44.
Montoya, R. M., Horton, R. S., and Kirchner, J. (2008). Is actual similarity necessary for attraction? A meta-analysis of actual and perceived similarity. J. Soc. Pers. Relat. 25, 889–922. doi: 10.1177/0265407508096700
Moreland, R. L., and Zajonc, R. B. (1982). Exposure effects in person perception: Familiarity, similarity, and attraction. J. Exp. Soc. Psychol. 18, 395–415. doi: 10.1016/0022-1031(82)90062-2
Morris, D. (1982). “Attachment and intimacy,” in Intimacy , eds M. Fischer, and G. Stricter (Boston, MA: Springer), 305–323. doi: 10.1007/978-1-4684-4160-4_19
Morry, M. M. (2005). Relationship satisfaction as a predictor of similarity ratings: a test of the attraction-similarity hypothesis. J. Soc. Pers. Relat. 22, 561–584. doi: 10.1177/0265407505054524
Neto, F. (2012). Compassionate love for a romantic partner, love styles and subjective well-being. Interpers. Int. J. Pers. Relatsh. 6, 23–39. doi: 10.5964/ijpr.v6i1.88
Noriuchi, M., and Kikuchi, Y. (2013). [Neural basis of maternal behavior]. Seishin Shinkeigaku Zasshi 115, 630–634.
Noriuchi, M., Kikuchi, Y., and Senoo, A. (2008). The functional neuroanatomy of maternal love: mother’s response to infant’s attachment behaviors. Biol. Psychiatry 63, 415–423. doi: 10.1016/j.biopsych.2007.05.018
Norton, M., Frost, J., Ariely, D., Reis, H., Maniaci, M., Caprariello, P., et al. (2015). When does familiarity promote versus undermine interpersonal attraction? A proposed integrative model from erstwhile adversaries. Perspect. Psychol. Sci. 10, 3–19. doi: 10.1177/1745691614561682
Oleson, M. D. (1996). Adolescents’ Recollection of Early Physical Contact: Implications for Attachment and Intimacy. Master’s thesis, Utah State University, Logan, UT.
Orosz, G., Szekeres, Á., Kiss, Z. G., Farkas, P., and Roland-Lévy, C. (2015). Elevated romantic love and jealousy if relationship status is declared on Facebook. Front. Psychol. 6:214. doi: 10.3389/fpsyg.2015.00214
Papp, L. M., Cummings, E. M., and Goeke-Morey, M. C. (2009). For richer, for poorer: money as a topic of marital conflict in the home. Fam. Relat. 58, 91–103. doi: 10.1111/j.1741-3729.2008.00537.x
Park, C. W., MacInnis, D. J., and Eisingerich, A. B. (2016). Brand Admiration: Building a Business People Love , 1st Edn. Hoboken, NJ: Wiley.
Park, C. W., Macinnis, D. J., Priester, J., Eisingerich, A. B., and Iacobucci, D. (2010). Brand attachment and brand attitude strength: conceptual and empirical differentiation of two critical brand equity drivers. J. Mark. 74, 1–17.
Pascual, C. O., and Académico, C. (2015). María del Rosario Zulaica López TRABAJO FIN DE GRADO Brand Awareness and Brand Love. Is the too-of-Mind the Most Loved On? An Application to Fashion Retailers. Available online at: https://biblioteca.unirioja.es/tfe_e/TFE001238.pdf (accessed February 22, 2020).
Pedeliento, G., Andreini, D., Bergamaschi, M., and Salo, J. (2016). Brand and product attachment in an industrial context: the effects on brand loyalty. Ind. Mark. Manage. 53, 194–206. doi: 10.1016/J.INDMARMAN.2015.06.007
Péloquin, K., Brassard, A., Delisle, G., and Bédard, M.-M. (2013). Integrating the attachment, caregiving, and sexual systems into the understanding of sexual satisfaction. Can. J. Behav. Sci. 45, 185–195. doi: 10.1037/a0033514
Rauschnabel, P. A., and Ahuvia, A. C. (2014). You’re so lovable: anthropomorphism and brand love. J. Brand Manage. 21, 372–395. doi: 10.1057/bm.2014.14
Regan, P. C., and Berscheid, E. (1999). Lust: What we Know about Human Sexual Desire. Thousand Oaks, CA: SAGE Publications, Inc. doi: 10.4135/9781452233727
Reis, H. T., and Shaver, P. (1988). “Intimacy as an interpersonal process,” in Handbook of Personal Relationships: Theory, Research and Interventions , eds S. Duck, D. F. Hay, S. E. Hobfoll, W. Ickes, and B. M. Montgomery (Oxford: John Wiley & Sons), 367–389.
Rempel, J. K., and Holmes, J. G. (1985). Trust in close relationships. J. Pers. Soc. Psychol. 49, 95–112. doi: 10.1037/0022-3514.49.1.95
Rodriguez, L. M., DiBello, A. M., Øverup, C. S., and Neighbors, C. (2015). The price of distrust: trust, anxious attachment, jealousy, and partner abuse. Partner Abuse 6, 298–319. doi: 10.1891/1946-6560.6.3.298
Rohde, P. A., Atzwanger, K., Butovskaya, M., Lampert, A., Mysterud, I., Sanchez-Andres, A., et al. (2003). Perceived parental favoritism, closeness to kin, and the rebel of the family The effects of birth order and sex. Evol. Hum. Behav. 24, 261–276. doi: 10.1016/S1090-5138(03)00033-3
Rubin, Z. (1970). Measurement of romantic love. J. Pers. Soc. Psychol. 16, 265–273.
Rusbult, C. E. (1980). Commitment and satisfaction in romantic associations: a test of the investment model. J. Exp. Soc. Psychol. 16, 172–186. doi: 10.1016/0022-1031(80)90007-4
Rusbult, C. E., Bissonnette, V. L., Arriaga, X. B., Cox, C. L., and Weiss, R. L. (1998). “Accommodation processes during the early years of marriage,” in The Developmental Course of Marital Dysfunction , ed. T. N. Bradbury (Cambridge: Cambridge University Press), 74–113. doi: 10.1017/CBO9780511527814.005
Russo, B., Boess, S., and Hekkert, P. (2011). ‘What’s love got to do with it?’ the experience of love in person-product relationships. Des. J. 14, 8–27. doi: 10.2752/175630610X12877385838687
Saegert, S., Swap, W., and Zajonc, R. B. (1973). Exposure, context, and interpersonal attraction. J. Pers. Soc. Psychol. 25, 234–242. doi: 10.1037/h0033965
Sailor, J. L. (2013). A phenomenological study of falling out of romantic love. Qual. Rep. 18, 1–22.
Salazar, L. R. (2015). Exploring the relationship between compassion, closeness, trust, and social support in same-sex friendships. J. Happiness Well Being 3, 15–29.
Salmon, C. A., Shackelford, T. K., and Michalski, R. L. (2012). Birth order, sex of child, and perceptions of parental favoritism. 52, 357–362. doi: 10.1016/j.paid.2011.10.033
Seshadri, K. G. (2016). The neuroendocrinology of love. Indian J. Endocrinol. Metab. 20, 558–563. doi: 10.4103/2230-8210.183479
Setyawan, A. A., and Kussudiyarsana, I. (2015). Brand trust and brand loyalty, an empirical study in indonesia consumers. Br. J. Mark. Stud. 4, 37–47.
Siennick, S. E. (2013). Still the Favorite? Parents’ differential treatment of siblings entering young adulthood. J. Marriage Fam. 75, 981–994.
Simpson, J. A. (2007). Foundations of Interpersonal Trust: Handbook of Basic Principles. New York, NY: Guilford.
Singh, R., Goh, A., Sankaran, K., and Bhullar, N. (2016). Similarity and liking effects on interpersonal attraction: test of the two-dimensional trust-respect model. Psychologia 59, 1–18. doi: 10.2117/psysoc.2016.1
Singh, R., Wegener, D. T., Sankaran, K., Singh, S., Lin, P. K. F., Seow, M. X., et al. (2015). On the importance of trust in interpersonal attraction from attitude similarity. J. Soc. Pers. Relat. 32, 829–850. doi: 10.1177/0265407515576993
Sinha, A. K. (2017). Impact of product innovation in building brand equity on consumer’s choice with a focus on brand resonance. Int. J. Innov. Manage. Technol. 8, 482–487. doi: 10.18178/ijimt.2017.8.6.775
Sprecher, S., Christopher, F. S., and Cate, R. (2006). “Sexuality in close relationships,” in The Cambridge Handbook of Personal Relationships , eds A. L. Vangelisti and D. Perlman (Cambridge: Cambridge University Press), 463–482. doi: 10.1017/CBO9780511606632.026
Sprecher, S., and Fehr, B. (2005). Compassionate love for close others and humanity. J. Soc. Pers. Relat. 22, 629–651. doi: 10.1177/0265407505056439
Stanley, S. M., Rhoades, G. K., and Whitton, S. W. (2010). Commitment: functions, formation, and the securing of romantic attachment. J. Fam. Theory Rev. 2, 243–257. doi: 10.1111/j.1756-2589.2010.00060.x
Steinberg, L. D., Catalano, R., and Dooley, D. (1981). Economic antecedents of child abuse and neglect. Child Dev. 52, 975–985. doi: 10.2307/1129102
Sternberg, R. J. (1986). A triangular theory of love. Psychol. Rev. 93, 119–135. doi: 10.1037/0033-295X.93.2.119
Sternberg, R. J. (1997). Construct validation of a triangular love scale. Eur. J. Soc. Psychol. 27, 313–335. doi: 10.1007/s10936-019-09661-y
Sternberg, R. J., and Grajek, S. (1984). The nature of love. J. Pers. Soc. Psychol. 47, 312–329. doi: 10.1037/0022-3514.47.2.312
Stokburger-Sauer, N., Ratneshwar, S., Sen, S., Howard, B. K., and Chair, W. B. (2008). Drivers of consumer-brand identification. Int. J. Res. Mark. 35.
Suitor, J. J., and Pillemer, K. (2007). Mothers’ favoritism in later life. Res. Aging 29, 32–55. doi: 10.1177/0164027506291750
Sullivan, R., Perry, R., Sloan, A., Kleinhaus, K., and Burtchen, N. (2011). Infant bonding and attachment to the caregiver: insights from basic and clinical science. Clin. Perinatol. 38, 643–655. doi: 10.1016/j.clp.2011.08.011
Sykes, R. E., Larntz, K., and Fox, J. C. (1976). Proximity and similarity effects on frequency of interaction in a class of naval recruits. Sociometry 39, 263. doi: 10.2307/2786519
Tedam, P. (2014). Witchcraft branding and the abuse of African children in the UK: causes, effects and professional intervention. Early Child Dev. Care 184, 1403–1414. doi: 10.1080/03004430.2014.901015
Thomson, M., MacInnis, D. J., and Whan Park, C. (2005). The ties that bind: measuring the strength of consumers’ emotional attachments to brands. J. Consum. Psychol. 15, 77–91. doi: 10.1207/S15327663JCP1501_10
Tobore, T. (2018). On the Principles of Social Gravity: How Human Systems Work, from the Family to the United Nations. Delaware, DE: Vernon Press.
Towner, S. L., Dolcini, M. M., and Harper, G. W. (2015). Romantic relationship dynamics of urban african american adolescents: patterns of monogamy, commitment, and trust. Youth Soc. 47, 343–373. doi: 10.1177/0044118X12462591
Turgut, M. U., and Gultekin, B. (2015). The critical role of brand love in clothing brands. J. Bus. Econ. Finance 4:126. doi: 10.17261/Pressacademia.201519963
Wetzel, C. G., and Insko, C. A. (1982). The similarity-attraction relationship: Is there an ideal one? J. Exp. Soc. Psychol. 18, 253–276. doi: 10.1016/0022-1031(82)90053-1
Whang, Y.-O., Allen, J., Sahoury, N., and Zhang, H. (2004). “Falling in love with a product: the structure of a romantic consumer-product relationship,” in Advances in Consumer Research , eds B. E. Kahn, and M. F. Luce (Valdosta, GA: Association for Consumer Research), 320–327.
Whitley, B. E. (1993). Reliability and aspects of the construct validity of sternberg’s triangular love scale. J. Soc. Pers. Relat. 10, 475–480. doi: 10.1177/0265407593103013
Wieselquist, J., Rusbult, C. E., Foster, C. A., and Agnew, C. R. (1999). Commitment, pro-relationship behavior, and trust in close relationships. J. Pers. Soc. Psychol. 77, 942–966. doi: 10.1037/0022-3514.77.5.942
Wilson, S., Morse, J. M., and Penrod, J. (1998). Developing reciprocal trust in the caregiving relationship. Qual. Health Res. 8, 446–465. doi: 10.1177/104973239800800402
Yasin, M., and Shamim, A. (2013). Brand love: mediating role in purchase intentions and word-of-mouth. IOSR J. Bus. Manage. 7, 101–109.
Zarantonello, L., Romani, S., Grappi, S., and Bagozzi, R. P. (2016). Brand hate. J. Prod. Brand Manage. 25, 11–25. doi: 10.1108/JPBM-01-2015-0799
Zhou, L. (2017). The Aquila Digital Community How Visual Communication Strategies, Brand Familiarity, And Personal Relevance Influence Instagram Users’ Responses To Brand Content. Graphic Communications Commons. Available online at: https://aquila.usm.edu/dissertationshttps://aquila.usm.edu/dissertations/1435 (accessed February 22, 2020).
Zimmerman, K. J., Smith, J. M., Simonson, K., and Myers, B. W. (2015). Familial relationship outcomes of coming out as an atheist. Secular. Nonrelig. 4, 1–13. doi: 10.5334/snr.aw
Keywords : triangular theory of love, Romance, brand love, parental love, maternal love, Meaning of love, Definition of love, am I in love
Citation: Tobore TO (2020) Towards a Comprehensive Theory of Love: The Quadruple Theory. Front. Psychol. 11:862. doi: 10.3389/fpsyg.2020.00862
Received: 20 September 2019; Accepted: 07 April 2020; Published: 19 May 2020.
Reviewed by:
Copyright © 2020 Tobore. This is an open-access article distributed under the terms of the Creative Commons Attribution License (CC BY) . The use, distribution or reproduction in other forums is permitted, provided the original author(s) and the copyright owner(s) are credited and that the original publication in this journal is cited, in accordance with accepted academic practice. No use, distribution or reproduction is permitted which does not comply with these terms.
*Correspondence: Tobore Onojighofia Tobore, [email protected]
Disclaimer: All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Click through the PLOS taxonomy to find articles in your field.
For more information about PLOS Subject Areas, click here .
Loading metrics
Open Access
Peer-reviewed
Research Article
Regulation of Romantic Love Feelings: Preconceptions, Strategies, and Feasibility
* E-mail: [email protected]
Affiliations Department of Psychological Sciences, University of Missouri–St. Louis, St. Louis, Missouri, United States of America, Department of Psychology, University of Maryland, College Park, Maryland, United States of America
Affiliation Institute of Psychology, Erasmus University Rotterdam, Rotterdam, The Netherlands
- Sandra J. E. Langeslag,
- Jan W. van Strien

- Published: August 16, 2016
- https://doi.org/10.1371/journal.pone.0161087
- Reader Comments
Love feelings can be more intense than desired (e.g., after a break-up) or less intense than desired (e.g., in long-term relationships). If only we could control our love feelings! We present the concept of explicit love regulation, which we define as the use of behavioral and cognitive strategies to change the intensity of current feelings of romantic love. We present the first two studies on preconceptions about, strategies for, and the feasibility of love regulation. Questionnaire responses showed that people perceive love feelings as somewhat uncontrollable. Still, in four open questions people reported to use strategies such as cognitive reappraisal, distraction, avoidance, and undertaking (new) activities to cope with break-ups, to maintain long-term relationships, and to regulate love feelings. Instructed up-regulation of love using reappraisal increased subjective feelings of attachment, while love down-regulation decreased subjective feelings of infatuation and attachment. We used the late positive potential (LPP) amplitude as an objective index of regulation success. Instructed love up-regulation enhanced the LPP between 300–400 ms in participants who were involved in a relationship and in participants who had recently experienced a romantic break-up, while love down-regulation reduced the LPP between 700–3000 ms in participants who were involved in a relationship. These findings corroborate the self-reported feasibility of love regulation, although they are complicated by the finding that love up-regulation also reduced the LPP between 700–3000 ms in participants who were involved in a relationship. To conclude, although people have the preconception that love feelings are uncontrollable, we show for the first time that intentional regulation of love feelings using reappraisal, and perhaps other strategies, is feasible. Love regulation will benefit individuals and society because it could enhance positive effects and reduce negative effects of romantic love.
Citation: Langeslag SJE, van Strien JW (2016) Regulation of Romantic Love Feelings: Preconceptions, Strategies, and Feasibility. PLoS ONE 11(8): e0161087. https://doi.org/10.1371/journal.pone.0161087
Editor: Alexandra Key, Vanderbilt University, UNITED STATES
Received: March 8, 2016; Accepted: July 31, 2016; Published: August 16, 2016
Copyright: © 2016 Langeslag, van Strien. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Data Availability: Our data cannot be made publicly available for ethical reasons. That is, participants were not asked for permission for their data to be shared. Parts of the data are available on request. Please send requests to Sandra Langeslag ( [email protected] ).
Funding: The authors received no specific funding for this work.
Competing interests: The authors have declared that no competing interests exist.
Introduction
Romantic love strikes virtually everyone at least once (i.e., its lifetime prevalence approaches 100%) [ 1 ] and has a great impact on our lives. Romantic love has positive effects on individuals and society as a whole. For example, love is associated with positive emotions such as euphoria [ 2 ] and romantic relationships enhance happiness and life satisfaction [ 3 ]. But love also has a negative impact on individuals and society. For example, love is associated with stress [ 4 ] and jealousy [ 5 ], and romantic break-ups are associated with sadness and shame [ 6 ], a decrease in happiness and life satisfaction [ 7 ], and depression [ 8 ]. The high prevalence of love combined with its significant positive and negative impact on individuals and society make it an important research topic.
The word ‘love’ has many different meanings and may have different meanings to different people. Researchers have proposed several taxonomies of love, with various numbers of love types or components [ 9 – 13 ]. In this study, two types of love feelings are considered: infatuation and attachment. Infatuation is the overwhelming, amorous feeling for one individual, and is similar to the concepts ‘passion’ or ‘infatuated love’ [ 10 ], ‘romantic love’ [ 11 ], ‘passionate love’ [ 12 ], and ‘attraction’ [ 13 ]. Attachment, on the other hand, is the comforting feeling of emotional bonding with another individual, and is similar to the concepts ‘intimacy’ with ‘decision/commitment’ [ 10 ], and ‘companionate love’ [ 10 – 12 ].
Love feelings are sometimes weaker than desired. Infatuation is typically most intense at the early stages of love after which it decreases relatively quickly [ 13 – 15 ] and attachment takes some time to develop [ 13 – 15 ] after which it decreases over the course of decades [ 16 ]. The decrease of infatuation and attachment over time threatens the stability of romantic relationships. Indeed, falling out of love is the primary reason for divorce [ 17 ]. Love feelings can also be stronger than desired. People may, for example, be in love with someone who does not love them back or who has broken up with them. Clearly, it would be advantageous if we could regulate love feelings at will, so that we could up-regulate them when they are weaker than desired, and down-regulate them when they are stronger than desired.
We define love regulation as the use of behavioral or cognitive strategies to change the intensity of current feelings of romantic love. In an interview study, participants reported that their love feelings were involuntary and uncontrollable [ 2 ]. Nevertheless, three lines of research suggest that love regulation may actually be feasible. First, it is well known that people can regulate their emotions [ 18 – 21 ], which entails generating new emotions or changing the intensity of current emotions using behavioral or cognitive strategies [ 20 ]. There are multiple emotion regulation strategies, including situation selection, distraction, expression suppression, and cognitive reappraisal. Situation selection is to avoid or seek out certain situations to change the way you feel (e.g., attending a party to have fun) [ 21 ]. Distraction entails performing a secondary task to reduce the intensity of emotions (e.g., playing a video game to forget about a bad incident at work) [ 20 ]. Expression suppression involves inhibiting the expression of an emotion (e.g., keeping a poker face) [ 22 ]. Cognitive reappraisal involves reinterpreting the situation to change the way you feel (e.g., decreasing or increasing nervousness by reinterpreting an upcoming job interview as an opportunity to learn more about the company or as a once in a lifetime opportunity, respectively) [ 22 ]. Emotion regulation can be used to up- and down-regulate positive and negative emotions [ 23 ] and may happen implicitly or explicitly [ 18 ].
However, love is sometimes considered a motivation (or drive) rather than an emotion [ 24 ]. One reason why love would not be an emotion is that it elicits different emotions depending on the situation. Reciprocated love, for example, may elicit the emotion euphoria, while unreciprocated love may elicit the emotion sadness. It is therefore important that a second line of research has shown that people can use cognitive strategies to regulate their motivations, including sexual arousal [ 25 ], excitement about monetary reward [ 26 – 29 ], and craving for alcohol, food, and cigarettes [ 30 , 31 ]. The evidence that motivations can be regulated intentionally supports the idea that explicit love regulation may be feasible.
Finally, a third research line has shown that people think more favorably of their romantic partner than objectively justified [ 32 , 33 ]. Importantly, people who idealize their partner and whose partners idealize them have happier relationships [ 34 ]. These findings suggest that implicit up-regulation of love feelings for the current romantic partner is feasible and that it contributes to relationship satisfaction.
Even though this last research line shows that people can regulate their love feelings implicitly, there are no studies that provide information about the deliberate, explicit up- and down-regulation of love feelings. In two studies, we systematically examined preconceptions about, strategies for, and the feasibility of explicit regulation of love feelings. The first goal was to determine whether people think that love feelings can be controlled or not. Participants answered a series of questions that measured perceived control over love feelings and previous research [ 2 ] led us to hypothesize that people would perceive love feelings as uncontrollable. The second goal was to reveal which strategies people use when they try to up- and down-regulate their love feelings. Participants responded to four open questions and we expected that people would report the use of typical behavioral and cognitive emotion regulation strategies mentioned above. First, we conducted a pilot study (Study 1) and then we conducted another study (Study 2) to confirm the findings of the pilot study.
In addition, Study 2 employed a love regulation task to achieve the final research goal, which was to examine if people can intentionally up- and down-regulate love feelings. In this first empirical test of the feasibility of love regulation, we focused on the reappraisal strategy because it is considered effective in altering feeling intensity and beneficial for cognitive and social functioning [ 21 ]. Situation-focused reappraisal entails changing the emotional meaning of a situation by reinterpreting it [ 21 ], for example by focusing on positive or negative aspects of the situation, or by imagining a positive or negative outcome [ 35 ]. The use of cognitive reappraisal to regulate love feelings is related to the notion that cognitive processes, including making attributions, are associated with relationship satisfaction [ 36 , 37 ]. We focus on the intensity of infatuation and attachment rather than relationship outcomes, since love feelings do not occur exclusively in the context of romantic relationships [ 14 ].
Because it depends on the situation whether people would benefit from love up- or down-regulation, we tested a group of people who were involved in a romantic relationship and a group of people who had recently experienced a romantic break-up. People who are currently in a romantic relationship were expected to benefit from love up-regulation, because that would stabilize their relationship. People who have just experienced a break-up, in contrast, would benefit from love down-regulation, because that could help them cope with the break-up. Because previous research has shown that intense feelings of romantic love can be elicited by viewing pictures of the beloved [ 38 ], pictures of the (ex-)partner were used to elicit feelings of love, which participants were instructed to regulate in an explicit regulation task. Because self-reports are the only way to assess phenomenology (i.e., how someone feels) [ 39 ], participants rated how infatuated and how attached they felt after each regulation condition. It was hypothesized that love up-regulation would increase feelings of infatuation and attachment, whereas love down-regulation would decrease feelings of infatuation and attachment in both groups. It is of course important to dissociate between the concept of love regulation and the well-established concept of emotion regulation. Therefore, participants also rated how negative or positive they felt after each regulation condition. It was expected that love up-regulation would make the relationship group feel more positive, while love down-regulation would make them feel more negative. The opposite pattern was expected for the break-up group: feeling more negative following up-regulation and more positive following down-regulation. This hypothesis shows how love regulation is theoretically distinct from emotion regulation. That is, love regulation targets the intensity of love feelings rather than emotions. Of course, the change in love feelings may in turn influence emotions or affect. The direction of the effect of love regulation on emotion or affect may differ depending on the context, as indicated by the hypothesized opposite effects of love regulation on emotion/affect in the relationship and break-up groups.
Even though self-reports gain a unique insight into what people experience, they also suffer from social desirability biases and demand characteristics [ 40 , 41 ]. Therefore, in addition to subjective self-reports, we used event-related potentials (ERPs) as a more objective measure of love regulation success. ERPs have been used before to study emotion regulation and to study romantic love, but not to study love regulation. The late positive potential (LPP) reflects multiple and overlapping positivies over the posterior scalp beginning in the time range of the classic P300, i.e., around 300 ms after stimulus onset. The LPP amplitude is typically enhanced for negative and positive compared to neutral stimuli [ 19 ] and is therefore thought to reflect the affective and motivational intensity of information and the resulting motivated attention [ 42 ]. Correspondingly, we have shown that the LPP is enhanced in response to pictorial and verbal beloved-related information compared to control information [ 32 , 43 , 44 ]. Importantly, the LPP amplitude is modulated by emotion regulation instructions according to the regulatory goal: emotion down-regulation reduces the LPP amplitude, while emotion up-regulation enhances the LPP amplitude [ 27 , 45 – 49 ]. The LPP amplitude can therefore be used as an objective measure of regulation success [ 19 ]. Because the LPP reflects affective and motivational significance and the resulting motivated attention, rather than valence [ 42 ], regulation effects in the LPP amplitude reflect how regulation changes the affective and motivational intensity of information and the amount of motivated attention allocated to that information. It was expected that love up-regulation would enhance the LPP in response to pictures of the (ex-)partner in both groups, which would indicate that love up-regulation would enhance the affective and motivational significance of, and the resulting motivated attention to the (ex-)partner. Love down-regulation, in contrast, was expected to reduce the LPP amplitude to (ex-)partner pictures in both groups, which would indicate that love down-regulation would reduce the affective and motivational significance of, and the resulting motivated attention to the (ex-)partner.
Study 1 –Methods
Participants.
Thirty-two participants (18–30 yrs, M = 21.4, 7 men) who were in love by self-report were recruited from the University of Maryland community in the US. Being in love was an inclusion criterion because some of the questions assessing perceived control over love feelings (see below) contained a blank in which the participants had to mentally insert the name of their beloved. The study was approved by the Institutional Review Board of the University of Maryland and written informed consent was obtained. Participants were remunerated with $10.
First, participants completed some questions about their love feelings and their romantic relationship [ 44 ]. Participants also completed the Infatuation and Attachment Scales (IAS) [ 14 ], and the Passionate Love Scale (PLS) [ 50 ] to assess the intensity of infatuation and attachment. Then, participants completed 17 questions to assess perceived control of love feelings (Cronbach’s alpha = .93), see the S1 Appendix . These questions were phrased to measure perceived control over love in general, and over infatuation and attachment specifically. They were also phrased to measure perceived control over one’s own vs. people’s love feelings, and over the intensity and object of love feelings. Participants responded using a 9-point Likert scale (1 = totally disagree, 9 = totally agree).
Subsequently, participants answered four open questions about the use of behavioral and cognitive strategies in the contexts of heartbreak and long-term relationships. We distinguished between emotion regulation and love down-regulation in the context of heartbreak by asking two questions: “What do you do or think to feel better when you have a broken heart?” (i.e., emotion regulation), “What do you do or think to decrease feelings of love when you have a broken heart?” (i.e., love down-regulation). In addition, we distinguished between maintaining relationships and love up-regulation in the context of long-term relationships by asking two questions: “What do you do or think to maintain a long-term relationship?” (i.e., maintaining relationships), and “What do you do or think to prevent that feelings of love decline in a long-term relationship?” (i.e., love up-regulation). If participants had not experienced heartbreak or any long-term relationships, they replied with what they think they would do in those circumstances.
The mean score on the 17 perceived control questions was subjected to a one-sample t -test against 5, to test if it differed from neutral. In addition, responses on subsets of the 17 questions that measured perceived control over a certain aspect of love were averaged to obtain measures of perceived control over seven different aspects of love (love in general, infatuation, attachment, self, people in general, intensity of love, and object of love). Five paired sample t -tests were conducted to test for differences in perceived control between related aspects of love (i.e., love in general vs. infatuation, love in general vs. attachment, infatuation vs. attachment, self vs. people in general, and intensity vs. object of feelings).
The responses to the four open strategy questions were analyzed qualitatively. Many participants listed multiple strategies in response to each of the four open strategy questions. Each strategy was scored as being an exemplar of a certain category. A priori categories were emotion regulation strategies such as reappraisal, distraction, and suppression [ 20 , 21 ]. In the heartbreak context, reappraisal was subdivided into “focus on the negative aspects of the beloved/relationship”, “think of negative future scenarios”, “think about the positive aspects of the situation”, and “other”. In the long-term relationship context, reappraisal was subdivided into “focus on the positive aspects of the beloved/relationship”, and “think of positive future scenarios”. Other categories such as avoidance (see Tables 1 and 2 ) were added on the basis of participants’ responses.
- PPT PowerPoint slide
- PNG larger image
- TIFF original image
https://doi.org/10.1371/journal.pone.0161087.t001
https://doi.org/10.1371/journal.pone.0161087.t002
Study 1 –Results
Participant characteristics.
All participants had an opposite-sex beloved. Twenty-seven (84%) of the participants reported to be in a relationship with their beloved, which supports the idea that love does not occur exclusively in the context of relationships [ 14 ]. See Table 3 for the other love characteristics.
Means (ranges in parentheses).
https://doi.org/10.1371/journal.pone.0161087.t003
Perceived control
The mean score on the 17 perceived control questions was 4.5 ( SD = 1.4). A one-sample t -test revealed that this tended to be lower than 5 (= neutral), t (31) = -1.9, p = .066, which implies that participants perceive love feelings as neither controllable, nor uncontrollable, or as somewhat uncontrollable, if anything. See Table 4 for the mean perceived control over the seven different aspects of love. Participants felt more in control of feelings of attachment than infatuation, t (31) = 2.4, p = .022. There was no difference between the perceived control over the own vs. people’s feelings, t (31) = 0.5, p = .64. Participants felt more control over the intensity than the object of their love feelings, t (31) = 2.1, p = .047.
https://doi.org/10.1371/journal.pone.0161087.t004
See Tables 1 and 2 for the regulation strategies reported. In the context of heartbreak, participants mostly used distraction, social support, and reappraisal. Distraction (e.g., watching TV, listening to music, focusing on work or school, or exercise) and seeking social support (e.g., talking to or spending time with family/friends) were used more to feel better than to decrease love feelings. In contrast, reappraisal was used more to decrease love feelings than to feel better. Reappraisal by focusing on negative aspects of the beloved was the most popular reappraisal strategy. Examples of other reappraisal strategies were thinking that time will heal, finding someone else to love, or focusing on positive aspects of oneself or one’s life. Thinking about positive aspects of the situation (e.g., focusing on the advantages of being single or being hopeful for the future), as well as avoidance (i.e., not talking about the beloved, getting rid of all pictures, and eliminating all contact) were moderately popular strategies to decrease love feelings. Strategies such as reappraisal by thinking about negative future scenarios (“it just wasn’t meant to last”), eating/smoking, and expressing emotions (“cry”) were used least often. None of the participants reported the use of suppression. Two participants reported that they did not, or could not, decrease love feelings.
In the context of long-term relationships, participants stressed the importance of communication/honesty and undertaking (new) activities with their beloved. Communication/honesty was deemed important for maintaining long-term relationships, whereas undertaking (new) activities with the beloved, which is a situation selection strategy, was mostly used to prevent love feelings from declining. Other strategies such as expressing love feelings to the beloved, trust, spending (quality) time with the beloved, loving unconditionally/making compromises, the two reappraisal strategies, and spending time apart from the beloved were mentioned as well. Six participants stated that love feelings would not decline if the relationship was good and/or that they would end the relationship if love feelings would decline.
In short, several behavioral and cognitive strategies were used in the contexts of heartbreak and long-term relationships. Some of these strategies were the typical cognitive and behavioral emotion regulation strategies, such as reappraisal, distraction, and situation selection. While some strategies seemed specific for feeling better during heartbreak or for maintaining long-term relationships, strategies such as reappraisal by focusing on negative aspects of the beloved or the relationship and undertaking (new) activities with the beloved seemed specific for down- and up-regulation of love feelings, respectively.
Interim Discussion
The results of this first exploratory study show that people perceive love feelings as neither controllable, nor uncontrollable (or as somewhat uncontrollable, if anything). People did perceive more control over some aspects of love than others and the majority of people reported to use a variety of strategies when heartbroken or when in a long-term relationship. Some strategies seemed specific for changing the intensity of love feelings, rather than for regulating emotions or maintaining relationships. Because this was only a pilot study with mostly female participants, we conducted a follow-up study (Study 2) to replicate and confirm these preliminary findings in a more gender-balanced sample. As mentioned in the introduction, Study 2 also included a love regulation task to test the feasibility of love regulation.
Study 2 –Methods
Twenty participants who were in a romantic relationship (19–25 yrs, M = 21.7, 10 men) and 20 participants who had recently experienced a romantic break-up (19–26 yrs, M = 21.9, 10 men) were recruited from the Erasmus University Rotterdam community in The Netherlands. For brevity, we will use the words ‘partner’ and ‘relationship’ in the remainder of the paper regardless of whether the relationship was ongoing or had dissolved. Inclusion criteria were normal or corrected to-normal vision, right-handedness (as determined by a hand preference questionnaire [ 51 ]), no use of medication known to affect the central nervous system, and no mental disorders. The reason for excluding participants with mental disorders was that many mental disorders are associated with emotion dysregulation [ 23 ], which indicates that love regulation may also be different in patients than in healthy controls. Four participants had to be excluded from the EEG analyses because of experimenter error during the EEG recording ( n = 3) or too many artifacts ( n = 1, more information below). Therefore the EEG analyses are based on 18 participants who were in a romantic relationship (19–25 yrs, M = 21.8, 9 men) and 18 participants who had recently experienced a romantic break-up (19–26 yrs, M = 21.7, 8 men). The study was approved by the Psychologie Ethische Commissie of the Erasmus Universiteit Rottterdam and written informed consent was obtained. Participants were remunerated with course credit or €15.
Questionnaires
In addition to the questions about their love feelings and their romantic relationship [ 44 ], the 17 perceived control questions (Cronbach’s alpha = .92), the four open regulation strategy questions, the Infatuation and Attachment Scales (IAS) [ 14 ], and the Passionate Love Scale (PLS) [ 50 ] used in Study 1, participants completed the Emotion Regulation Questionnaire (ERQ) [ 22 ] to assess individual differences in the habitual use of reappraisal and suppression. Participants also completed the Positive Affect Negative Affect Schedules (PANAS) twice, once about the last two weeks and once about this moment [ 52 ].
Participants provided 30 digital pictures of their partner. There were no other requirements than that the pictures had to contain the partner. Therefore, the pictures could display parts of the partner (e.g., just the face) or the whole body of the partner, people other than the partner, a variety of facial expressions, objects, and scenery. The pictures were presented to elicit love feelings [ 38 ] and to help the participant come up with negative or positive aspects of the partner/relationship and future scenarios (see below). It is important to note that the variety of information on the pictures does not confound the effects of regulation, because the same 30 partner pictures were presented in each regulation condition. For the same reason, differences in picture content between the two groups could not confound the differences in regulation effects between groups. In addition, the pictures ensure high ecological validity, as the partner is typically encountered in a wide variety of contexts and with varying facial expressions. The neutral stimuli were 30 neutral pictures displaying humans from the International Affective Picture System (IAPS) [ 53 ] with neutral normative valence ( M = 5.4, SD = 0.5) and low normative arousal ( M = 3.5, SD = 0.5) ratings, see S1 Text .
Love regulation task
Participants completed a love regulation task, see Fig 1 , while their electroencephalogram (EEG) was recorded. In the first two blocks, participants passively viewed partner and neutral pictures (order counterbalanced between participants). In the third and fourth block, participants were instructed to up- and down-regulate their love feelings in response to the partner pictures (order counterbalanced between participants) using reappraisal. Up-regulation instructions were to increase love feelings by thinking about positive aspects of the partner (e.g., “He is so funny”) or relationship (e.g., “We get along so well”), or positive future scenarios (e.g., “We’ll get married”). Down-regulation instructions were to decrease love feelings by thinking about negative aspects of the partner (e.g., “She is so lazy”) or relationship (e.g., “We often fight”), or negative future scenarios (e.g., “We won’t stay together forever”). Participants could use the information in the picture for inspiration. For example, the partner wearing a yellow shirt and standing next to a friend on a picture could inspire the participant to up-regulate love feelings by thinking “I love that yellow shirt he’s wearing” and to down-regulate love feelings by thinking “He is always hitting on that friend, and he might cheat on me one day”. These are instructions of situation-focused reappraisal, which involves reinterpreting “the nature of the events themselves, reevaluating others’ actions, dispositions, and outcomes” rather than self-focused reappraisal, which involves altering “the personal relevance of events” ([ 35 ], p. 484). That is, focusing on negative/positive aspects of the partner involves a reevaluation of the partner’s dispositions (“My partner is a wonderful person” when focusing on positive aspects vs. “My partner is a terrible person” when focusing on negative aspects), focusing on negative/positive aspects of the relationship involves a reevaluation of the relationship (“I am/was in a good relationship” when focusing on positive aspects, and “I am/was in a bad relationship” when focusing on negative aspects), and imagining positive/negative future relationship scenarios involves reevaluation of outcomes.
Please note that the stimulus in this figure is not actually one of the pictures that were submitted by the participants. Instead, it is an IAPS picture [ 53 ] that resembles the kinds of pictures that participants submitted.
https://doi.org/10.1371/journal.pone.0161087.g001
Each block started with an instruction word (‘view’, ‘increase’, ‘decrease’) for 4 sec and consisted of 30 trials. Trial structure was: fixation cross for 900–1100 ms, picture for 3 sec, and blank screen for 2 sec. After each block, participants completed four ratings on a 1–5 scale: infatuation, attachment, valence, and arousal, and they also completed the PANAS at this moment [ 52 ]. After the regulation task, participants wrote down what they had thought to up- and down-regulate love feelings to verify that they had followed the instructions.
EEG recording and preprocessing
The EEG was recorded using a 32-channel amplifier and data acquisition software (ActiveTwoSystem, BioSemi). The 32 Ag-AgCl active electrodes were placed upon the scalp by means of a head cap (BioSemi), according to the 10–20 International System. Vertical electro-oculogram and horizontal electro-oculogram were recorded by attaching additional electrodes (UltraFlat Active electrodes, BioSemi) above and below the left eye, and at the outer canthi of both eyes. Another two electrodes were attached to the left and right mastoids. An active electrode (common mode sense) and a passive electrode (driven right leg) were used to comprise a feedback loop for amplifier reference. All signals were digitized with a sampling rate of 512 Hz, a 24 bit A/D conversion and a low pass filter of 134 Hz. The EEG data were analyzed with BrainVision Analyzer 2 (Brain Products, Gilching, Germany). Per participant, a maximum of one bad electrode included in the analyses (see below) was corrected using spherical spline topographic interpolation. Offline, an average mastoids reference was applied and the data were filtered using a 0.1–30 Hz band pass filter (phase shift-free Butterworth filters; 24 dB/octave slope) and a 50 Hz notch filter. Data were segmented in epochs from 200 ms pre-stimulus until 3000 ms post-stimulus onset. Ocular artifact correction was applied semi-automatically according to the Gratton and Coles algorithm [ 54 ]. The 200 ms pre-stimulus period was used for baseline correction. Artifact rejection was performed at individual electrodes with the criterion minimum and maximum baseline-to-peak -75 to +75 μV. Because at least 12 trials are needed to adequately estimate emotion regulation effects in the LPP amplitude [ 55 ], the one participant that had fewer than 12 trials left per electrode per condition was excluded from the EEG analyses, as mentioned above. At the three electrodes used in the analyses (see below), the average number of accepted trials per condition ranged from 29.5 to 29.8 out of 30.
Statistical analyses
Questionnaire scores were analyzed with independent samples t -tests to test for differences between groups (adjusted t , df , and p values are shown when the Levene’s test for equality of variances indicated variance differences between the groups). Besides the one-sample t -test against 5 (= neutral), the perceived control scores were analyzed with three ANOVAs: one ANOVA with factors Love type (love in general, infatuation, attachment) and Group (relationship, break-up), one ANOVA with factors Self/People (self, people in general) and Group, and one ANOVA with factors Intensity/Object (intensity, object) and Group. Pearson correlation coefficients were computed between the seven perceived control scores and the two ERQ subscales across groups. Ratings and PANAS scores after the view conditions were analyzed with an ANOVA with factors Picture (partner, neutral) and Group. Ratings and PANAS scores following the three conditions with partner pictures were analyzed with an ANOVA with factors Regulation (view, up-regulation, down-regulation) and Group. In this analysis, only significant effects involving the factor Regulation are reported, because the main effect of Group is not relevant for the research question.
Because the LPP begins in the time range of the classic P300 [ 19 ] and can last as long as the stimulus duration [ 56 ], the ERP was quantified by mean amplitude measures in four time windows based on previous work [ 47 , 48 , 56 – 58 ]: 300–400 ms, 400–700 ms, 700–1000 ms, 1000–3000 ms. For each time window, mean amplitudes measures at Fz, Cz, and Pz were subjected to two ANOVAs. The first concerned the two view blocks and tested the factors Picture, Group, and Caudality (Fz, Cz, Pz). Only significant effects involving the factor Picture are reported, because those are relevant for the research question. The second ANOVA concerned the three blocks with partner pictures and tested the factors Regulation, Group, and Caudality. In this analysis, only significant effects involving the factor Regulation are reported, because those are relevant for the research question. When applicable, the degrees of freedom were corrected using the Greenhouse-Geisser correction. The F values, uncorrected degrees of freedom, the ε values and corrected probability values are reported. A significance level of 5% (two-sided) was selected and Fisher’s least significance difference (LSD) procedure was applied. This procedure controls type I error rate by conducting follow-up tests for significant main and interaction effects only. Those follow-up tests were paired samples t -tests testing differences between conditions across both groups (in case of significant main or interaction effects without the factor Group) or within groups (in case of significant interactions with the factor Group).
Study 2 –Results
Group characteristics.
All participants had an opposite-sex partner. The average time since the break-up was 3.0 months (range = 0.5–13.5). Ten of these break-ups were initiated by the partner, six by the participant, and four break-ups were a joint decision. See Table 4 for the other group characteristics and the statistics related to group differences. The relationship and break-up groups did not differ in how long they had known their partner for, how long ago their love feelings had started, and the duration of their relationships. The break-up groups did tend to report lower relationship quality than the relationship group. The break-up group also felt less attached and tended to feel more infatuated with their partner than the relationship group. Moreover, the break-up group tended to have experienced less positive affect during the past two weeks and had experienced more negative affect in the past two weeks and at the start of the testing session than the relationship group. Finally, the relationship and break-up groups did not differ in their habitual use of reappraisal and suppression. Thus, the two groups differed from each other on variables that can be expected to be related to whether someone is in a relationship or has experienced a break-up, but the groups did not differ on variables that should be unrelated to relationship status.
The mean score on the 17 perceived control questions was 4.5 ( SD = 1.4). A one-sample t -test showed that this was significantly lower than 5 (= neutral), t (39) = -2.2, p = .032, which suggests that participants perceive love feelings as uncontrollable. See Table 3 for the mean perceived control over the seven different aspects of love. There was a significant main effect of Love type, F (2,76) = 19.8, ε = 1.0, p < .001. Participants felt more in control of feelings of attachment than of feelings of infatuation or love in general, both p s < .001. In addition, there tended to be a main effect of Self/People, F (1,38) = 3.9, p = .056. Participants tended to feel that they were less able to control their love feelings than people in general are. Finally, there was a main effect of Intensity/Object, F (1,38) = 14.6, p < .001. Participants felt more in control of the intensity than of the object of their love feelings. In none of these analyses, the main effect of Group or interactions with Group were significant, all F s < 2.4, all p s > .13, so perceived control over different aspects of love feelings did not differ between the relationship and break-up groups.
The ERQ reappraisal score correlated positively with perceived control over individual love feelings, r (38) = .32, p = .044, and tended to correlate positively with perceived control over the intensity of love feelings, r (38) = .30, p = .056, and with perceived control over the object of love feelings, r (38) = .29, p = .075, see Fig 2 . These findings suggest that the more participants used the reappraisal strategy to regulate emotions in their daily life, the more they perceived love feelings as controllable.
https://doi.org/10.1371/journal.pone.0161087.g002
See Tables 1 and 2 for the regulation strategies reported. Participants mostly used distraction and reappraisal when heartbroken. Distraction was used more to feel better, while reappraisal by focusing on the negative aspects of the beloved/relationship was used more to decrease love feelings. The other strategies, such as reappraisal by thinking about the positive aspects of the situation, other ways of reappraising, avoidance, suppression (“making yourself strong (pretend) for the outside world”), eating/smoking, and expressing emotions were used least often when heartbroken. None of the participants reported the use of reappraisal by thinking about negative future scenarios. Two participants reported that they could not decrease love feelings. The use of the different strategies did not appear to differ between the relationship and break-up groups. Seeking social support was less popular in the current Dutch sample than in the US sample in Study 1.
Participants stressed the importance of communication/honesty and undertaking (new) activities with their beloved during long-term relationships. Communication/honesty was mostly used for maintaining long-term relationships. The break-up group used undertaking (new) activities with the beloved mostly to prevent love feelings from declining, while the relationship group used this strategy both to maintain their relationship and to prevent love feelings from declining. Strategies such as expressing love feelings to the beloved, spending (quality) time with the beloved, and loving unconditionally/making compromises were mentioned by some participants. The latter was used more for maintaining long-term relationships than for preventing love feelings from declining. Both reappraisal strategies (i.e., focusing on positive aspects of the beloved/relationship and thinking about positive future scenarios), trust, and spending time apart from the beloved were mentioned by some participants. Two participants specifically stated that love feelings would not decline if the relationship was good and/or that they would end the relationship if love feelings would decline. Other than the above-mentioned difference in the context of undertaking (new) activities, there were no obvious differences between the relationship and break-up groups. There were no major differences between this Dutch sample and the US sample in Study 1.
To conclude, participants reported to use several behavioral and cognitive strategies in heartbreak and long-term relationship contexts. As in Study 1, some of these strategies were the typical cognitive and behavioral emotion regulation strategies, such as reappraisal, distraction, situation selection, and suppression. As in Study 1, some strategies seemed specific for feeling better during heartbreak (i.e., emotion regulation) or for maintaining long-term relationships, while strategies such as reappraisal by focusing on the negative aspects of the beloved or the relationship and undertaking (new) activities with the beloved were used to down- and up-regulate love feelings, respectively.
See Fig 3 for the infatuation, attachment, valence, and arousal ratings at the end of each block in the regulation task.
https://doi.org/10.1371/journal.pone.0161087.g003
View blocks.
The infatuation ratings after the two view blocks showed main effects of Picture, F (1,38) = 27.1, p < .001, and Group, F (1,38) = 5.6, p = .023. Infatuation was higher after passive viewing of partner than neutral pictures, and higher in the relationship than the break-up group. Attachment ratings also showed main effects of Picture, F (1,38) = 23.9, p < .001, and Group, F (1,38) = 5.6, p = .023. Attachment was higher after passive viewing of partner than neutral pictures, and higher in the relationship than the break-up group. Thus, partner pictures elicited more feelings of infatuation and attachment than neutral pictures in both groups, which shows that the use of partner pictures was effective in eliciting love feelings [ 38 ].
For valence ratings, the main effects of Picture, F (1,38) = 9.9, p = .003, and Group, F (1,38) = 7.7, p = .008 were modulated by a significant Picture x Group interaction, F (1,38) = 20.7, p < .001. The relationship group felt more positive after passive viewing of partner than neutral pictures, p < .001, whereas the break-up group did not, p = .41. Arousal ratings showed a main effect of Picture, F (1,38) = 26.8, p < .001, which was modulated by a significant Picture x Group interaction, F (1,38) = 7.9, p = .008. The relationship group felt more aroused after passive viewing of partner than neutral pictures, p < .001, whereas the break-up group did not, p = .10. Thus, partner pictures elicited positive and arousing feelings in the relationship group but not in break-up group, which confirms that the two groups differed in anticipated ways.
Regulation blocks.
The infatuation ratings after the three blocks with partner pictures showed a main effect of Regulation, F (2,76) = 39.6, ε = .84, p < .001. Infatuation was lower after down-regulation than after passive viewing or up-regulation, both p s < .001. Attachment ratings also showed a main effect of Regulation, F (2,76) = 36.7, ε = .91, p < .001. Attachment was highest after up-regulation, intermediate after passive viewing, and lowest after down-regulation, all p s < .013. Valence ratings showed a main effect of Regulation, F (2,76) = 31.6, ε = .98, p < .001. Participants felt less positive after down-regulation than after passive viewing or up-regulation, both p s < .001. Arousal ratings showed no significant effects involving the factor Regulation, all p s > .26. To summarize, subjective love feelings were modulated in the expected directions by instructed love regulation in both groups. Up-regulation of love increased feelings of attachment, and down-regulation of love decreased feelings of infatuation and attachment. Finally, down-regulation of love decreased the pleasantness of feelings in both groups.
Positive and negative affect
See Fig 4 for positive and negative affect during the regulation task.
https://doi.org/10.1371/journal.pone.0161087.g004
Positive affect after the two view blocks showed a main effect of Picture, F (1,38) = 27.2, p < .001, which was modulated by a significant Picture x Group interaction, F (1,38) = 21.7, p < .001. The relationship group experienced more positive affect after passive viewing of partner than neutral pictures, p < .001, while the break-up group did not, p = .71. Negative affect showed main effects of Picture, F (1,38) = 9.6, p = .004, and Group, F (1,38) = 25.7, p < .001, which were modulated by a significant Picture x Group interaction, F (1,38) = 8.7, p = .005. The break-up group experienced more negative affect after passive viewing of partner than neutral pictures, p = .006, while the relationship group did not, p = .69. In short, partner pictures elicited positive affect in the relationship group, but negative affect in the break-up group, again confirming that the groups differed in expected ways.
Positive affect after the three blocks with partner pictures showed a main effect of Regulation, F (2,76) = 21.3, ε = .94, p < .001, which was modulated by a significant Regulation x Group interaction, F (2,76) = 8.4, ε = .94, p = .001. While the relationship group experienced most positive affect after passive viewing of partner pictures, intermediate positive affect after up-regulation and least positive affect after down-regulation, all p s < .034, positive affect in the break-up group was not affected by instructed love regulation, all p s > .17. Negative affect showed a main effect of Regulation, F (2,76) = 6.4, ε = .74, p = .007, which was modulated by a significant Regulation x Group interaction, F (2,76) = 5.0, ε = .74, p = .017. The relationship group experienced most negative affect after down-regulation, both p s < .008, whereas negative affect in the break-up group was not affected by instructed love regulation, all p s > .67. To summarize, love regulation decreased positive affect in the relationship group, although down-regulation decreased positive affect more than up-regulation. Down-regulation also increased negative affect in the relationship group. Regulation of love feelings did not influence affect in the break-up group.
Event-related potentials
See Fig 5 for the ERP waveforms and Fig 6 for the scalp topographies of the differences between partner and neutral pictures in the view blocks. In all four time windows, there was a significant main effect of Picture (300–400 ms: F (1,34) = 72.6, p < .001, 400–700 ms: F (1,34) = 101.6, p < .001, 700–1000 ms: F (1,34) = 112.3, p < .001 and 1000–3000 ms: F (1,34) = 51.1, p < .001), indicating that the ERP between 300–3000 ms was more positive in response to the partner than neutral pictures. The interactions involving the factors Picture and Group were not significant in any of the time windows, all F s < 1, ns , which indicated that the ERP response to the partner compared to the neutral pictures did not differ between the relationship and break-up groups. Partner and neutral pictures differ in multiple ways: partner pictures were familiar to the participants, elicited emotional feelings, displayed at least one familiar person, and may have displayed the participant him-/herself. Because all of these factors modulate the ERP [ 32 , 42 , 59 – 61 ], it is not surprising that the ERP difference between partner and neutral pictures is so extended in time and topography, and similar between the two groups. Please note that the up- and down-regulation effects of interest discussed below involve comparisons between up- and down-regulation of responses to the partner pictures only.
https://doi.org/10.1371/journal.pone.0161087.g005
https://doi.org/10.1371/journal.pone.0161087.g006
See Fig 5 for the ERP waveforms and Fig 7 for the scalp topographies of the differences between regulation and view conditions. In the 300–400 ms time window, there were a main effect of Regulation, F (2,68) = 4.4, ε = .96, p = .018, and a Regulation x Caudality interaction, F (4,136) = 3.7, ε = .62, p = .020. The ERP was more positive for up-regulation than passive viewing at Cz and Pz, both p s < .004. In the 400–700 ms time window, there was a Regulation x Group x Caudality interaction, F (4,136) = 4.9, ε = .72, p = .004, but none of the post hoc tests were significant. In the 700–1000 ms, there were Regulation x Caudality, F (4,136) = 5.8, ε = .65, p = .002, and Regulation x Group x Caudality, F (4,136) = 5.2, ε = .65, p = .004, interactions. In the relationship group, the ERP was less positive for up- and down-regulation than passive viewing at Pz, both p s < .002. In the break-up group, none of the post hoc tests were significant. In the 1000–3000 ms time window, there was a Regulation x Group x Caudality interaction, F (4,136) = 2.7, ε = .78, p = .048. In the relationship group, the ERP was less positive for down-regulation than passive viewing at Cz and Pz, both p s < .041, and for up-regulation than passive viewing at Pz, p = .005. In the break-up group, none of the post hoc tests were significant. Inspection of the data revealed that even though the break-up group showed a less positive ERP for down-regulation at Cz (and at Pz to a lesser extent), the variation in ERP amplitudes was larger in the break-up group (down-regulation effect at Cz = -1.7 μV, SD = 4.0) than the relationship group (down-regulation effect at Cz = -1.6 μV, SD = 3.0), which explains why the effect did not reach significance in the break-up group.
https://doi.org/10.1371/journal.pone.0161087.g007
To explore any associations between the LPP amplitude and self-reports measures, Pearson correlation coefficients were computed between regulation effects in the LPP amplitude and regulation effects in infatuation ratings, attachment ratings, valence ratings, arousal ratings, positive affect, and negative affect, across groups. Because the regulation effects were largest at electrodes Cz and/or Pz, LPP regulation effects were averaged across these two electrodes. In the 700–1000 ms time window, the up-regulation effect in the LPP amplitude was negatively correlated with the up-regulation effect in negative affect, r (34) = -.40, p = .015, see Fig 8 . This correlation was not inflated by the possibly outlying data point (i.e., up-regulation effect in negative affect = 1.5), because the correlation was even greater and more significant after exclusion of this data point, r (33) = -.44, p = .008. As can be seen in Fig 8 , the more participants showed an enhanced LPP in response to up-regulation compared to passive viewing between 700–1000 ms, the more their negative affect decreased as a result of love up-regulation. The other correlations between the up-regulation effects in the LPP amplitude in any of the time windows and the up-regulation effects in self-reports were not significant, -.31 < all r s(34) < .32, all p s > .063. None of the down-regulation effects in the LPP amplitude in any of the time windows were significantly correlated with down-regulation effects in self-reports, -.20 < all r s(34) < .24, all p s > .17.
A negative up-regulation effect in negative affect means a reduction in negative affect due to love up-regulation. A positive up-regulation effect in the LPP amplitude means that the LPP was enhanced for love up-regulation.
https://doi.org/10.1371/journal.pone.0161087.g008
To summarize, up-regulation elicited a more positive ERP than passive viewing at midline centro-parietal electrodes between 300–400 ms. In addition, up- and down-regulation elicited a less positive ERP than passive viewing mostly at midline parietal electrodes between 700–3000 ms in the relationship group. The more love up-regulation enhanced the LPP amplitude between 700–1000 ms, the greater the decrease in negative affect by love up-regulation.
Because love feelings may be more or less intense than desired, it would be helpful if people could up- and down-regulate feelings of romantic love at will. In two studies, we examined preconceptions about, strategies for, and the feasibility of love regulation.
As expected, participants had the preconception that love is somewhat uncontrollable, as indicated by their scores on the series of questions assessing the perceived controllability of love feelings. Moreover, a few participants reported that they are unable to decrease love feelings when heartbroken. Some participants even stated that love feelings should not be up-regulated to maintain long-term relationships, because declining love feelings would indicate that the relationship is not meant to be. Research, however, has shown that infatuation (i.e., passionate love) and attachment (i.e., companionate love) typically do decline over time [ 14 , 16 ], so having this opinion might limit one’s chances of having long-lasting relationships. However, the mean score on the perceived control questions approached the midpoint of the scale, indicating that participants did not entirely reject the idea of controllable love. In addition, participants perceived some aspects of love to be more controllable than other aspects. Participants perceived feelings of attachment as more controllable than feelings of infatuation and they felt more in control of the intensity of love feelings than of who they are in love with. Finally, the more participants use the reappraisal strategy to regulate emotions in their daily life, the more they perceived love feelings as controllable, which provides a hint that reappraisal may be an effective love regulation strategy. Nevertheless, the questions about perceived control over love feelings have a couple of limitations. First, the two studies were conducted in different countries, in different languages, and with relatively small samples with different gender ratios. Second, in order to not be too statistically conservative in this explorative study, we did not correct for the number of statistical tests employed. Please note that the tests we performed are not independent, which reduces the chance of type I errors [ 62 ]. In addition, we used two-sided tests even when we had an a priori directional hypothesis. This was done to not increase the chance of Type I errors and to not exclude the possibility of observing any effects that were contrary to the hypothesis, again, because of the exploratory nature of the study. Finally, to the extent that the measures in Studies 1 and 2 overlapped, we base the conclusions above only on findings that replicated in both studies. This greatly reduces the chance that our conclusions are based on country-, language-, or gender-specific effects, or on spurious findings. It would be interesting to test whether perceived control over love feelings varies between regulation directions (i.e., whether people think it is easier to down-regulate love than to up-regulate love, or vice versa) in future studies.
We asked participants what they typically do or think when they are heartbroken and when maintaining long-term relationships. Participants reported the use of prototypical emotion regulation strategies such as reappraisal, distraction, and situation selection. Only one participant mentioned using suppression. Research has shown that expression suppression does not actually alter the intensity of feelings and that it has negative effects on cognitive and social functioning [ 21 ], so it might not be an adaptive strategy for regulating love feelings.
Importantly, responses to the questions suggested that there was a dissociation in the use of certain strategies for regulating actual love feelings (i.e., love regulation) versus feeling better during heartbreak (i.e., emotion regulation) or maintaining long-term relationships. In the context of heartbreak, reappraisal was often used, especially to decrease love feelings rather than to feel better. In contrast, distraction was used during heartbreak more to feel better than to decrease love feelings. It has been shown that people prefer to use distraction over reappraisal in situations in which emotions are very intense [ 63 ], which is often the case during heartbreak. Reappraisal may be more advantageous in the long run though, because decreasing love feelings might help people to move on after a break-up.
Some participants reported avoiding beloved-related cues, such as pictures or conversations, when heartbroken, which is a situation selection strategy [ 21 ]. It has been proposed that romantic love shows parallels to drug addiction [ 2 , 64 ]. Beloved-related cues elicit love feelings [ 38 ], just like drug-related cues increase drug craving [ 65 ], so avoiding beloved-related cues may reduce ‘craving’ for the beloved in the short term. However, one type of treatment for substance dependence and other mental disorders is exposure therapy, which is based on the mechanism of extinction [ 66 ]. Because avoidance of beloved-related cues might prevent extinction of the love feelings, it may not be a suitable strategy for down-regulating love feelings in the longer term.
In the context of long-term relationships, participants often mentioned the importance of communication/honesty and of undertaking (new) activities with their beloved. While communication/honesty was used more to maintain long-term relationships than to prevent love from declining, undertaking (new) activities with the beloved was mostly used to prevent love from declining. Previous work suggests that doing exciting things with the beloved may indeed be a successful strategy for love up-regulation [ 67 , 68 ]. Correspondingly, research on long-term romantic love has shown that married couples who engaged in novel and challenging activities together reported increases in love, closeness, and relationship quality [ 69 , 70 ]. Thus, undertaking novel and exciting activities with the beloved, which is a situation selection strategy [ 21 ], may be an effective behavioral strategy for up-regulating love feelings. Surprisingly, reappraisal was mentioned only infrequently in the context of maintaining long-term relationships. Given that reappraisal is an effective and healthy emotion regulation strategy [ 21 , 22 ], it may be an adaptive strategy to prevent love feelings from declining in long-term relationships.
The four open questions about the use of behavioral and cognitive strategies in the contexts of heartbreak and long-term relationships have some limitations. First, these data were analyzed qualitatively rather than quantitatively. Second, the other questionnaires and tasks used in both studies restricted the samples to participants who were in love (Study 1), who were in a romantic relationship, or who had recently experienced a romantic break-up (Study 2). Therefore, participants will have answered questions that did not match their current status (e.g., answering questions about heartbreak while in a happy relationship) or prior experience (i.e., some participants may have never been heartbroken or in a long-term relationship, in which case they replied what they think they would do in those circumstances). It is important to note that these four strategy questions were used more to explore what types of strategies people employ in their love life to aid the design of future studies on love regulation rather than to provide a stringent test of a priori hypotheses. Nevertheless, the current findings await confirmation in future studies with quantitative analyses and matching of questions with prior experience and/or current status.
In the four open strategy questions, we did not ask participants about the effectiveness of the strategies they listed. In Study 2, in contrast, we did assess the effectiveness of explicit love up- and down-regulation using the cognitive reappraisal strategy. We measured regulation success by asking participants how much infatuation and attachment they experienced after each regulation condition, because self-report is the only way to assess phenomenological experience [ 39 ]. When instructed to up-regulate love feelings by thinking about positive aspects of the partner or the relationship or imagining positive future scenarios, participants reported increased levels of attachment. Although love up-regulation numerically increased feelings of infatuation, this effect was not statistically significant. Thus, love up-regulation using reappraisal may be more successful for up-regulating attachment than infatuation. Future research could test whether other strategies may be more effective for up-regulating infatuations levels. Because long-term relationships are threatened by diminishing levels of infatuation and attachment over time [ 14 , 16 ], up-regulation of love feelings might help to stabilize long-term relationships. Although it has been shown before that people idealize their beloved [ 32 , 33 ] and that partner idealization is associated with greater relationship satisfaction [ 34 ], the current study is unique in showing that people are capable of up-regulating their love feelings deliberately and intentionally.
When instructed to down-regulate love feelings by thinking about negative aspects of the partner or the relationship or imagining negative future scenarios, participants reported decreased levels of infatuation and attachment, as expected. This has important implications for people whose love feelings are stronger than desired. For example, this finding suggests that after the dissolution of a long-term relationship, when levels of attachments are presumably higher than levels of infatuation [ 14 ], love regulation using reappraisal may be used to cope with the break-up by decreasing feelings of attachment. In addition, the current findings suggest that love down-regulation using reappraisal may be used to decrease feelings of infatuation, for example when early stage love feelings are unreciprocated or when someone develops a crush on someone else than their partner. Although previous studies have shown that people can implicitly derogate the attractiveness of people other than the current partner [ 71 , 72 ], the current investigation is unique because it reveals that people can deliberately down-regulate their love feelings for their (ex-)partner.
Because self-reports are the only way to assess subjective feelings [ 39 ], they are often used in behavioral and neuroimaging studies on emotion regulation as a way to assess regulation success (e.g., [ 49 , 57 , 73 , 74 ]). However, self-reports do suffer from desirability biases and demand characteristics [ 40 , 41 ]. Participants were not informed of the exact research purpose or hypothesis before testing, but they were instructed to increase or decrease their love feelings using cognitive reappraisal. So when they were asked to rate infatuation and attachment levels at the end of each block, their responses may have been biased by their perception of the study’s hypothesis. Still, the instructions mentioned ‘love feelings’ whereas the ratings mentioned ‘infatuation’ and ‘attachment’, which may have made our expectations a little less obvious. Also, even though we did not have different expectations about the feasibility of increasing and decreasing love, and participants had no reason to assume we had, the up-regulation effects in self-reported infatuation and attachment were numerically smaller (0.1 to 0.3 points on a 1–5 scale) than the down-regulation effects (0.5 to 1.0 points on a 1–5 scale), which makes it less likely that participants responded according to a perceived hypothesis rather than according to their feelings. Nevertheless, the current results await replication in studies in which the hypothesis would be more obscure to participants. This could for example be established by instructing participants to think about positive/negative aspects or future scenarios without mentioning that this is supposed to change the intensity of their love feelings. Also, note that the self-reports regarding valence, arousal, positive affect, and negative affect discussed next are less susceptible to demand characteristics since participants were not instructed to change how positive, negative, or aroused they felt.
Because it is important to dissociate the concept of love regulation from the well-established concept of emotion regulation, we asked participants how negative or positive they felt after each regulation condition. Participants who were in a romantic relationship with their beloved experienced more unpleasant feelings, less positive affect, and more negative affect following love down-regulation. This was expected, as down-regulation of love feelings for a current long-term partner is usually undesirable. However, also participants who had recently experienced a break-up unexpectedly experienced more unpleasant feelings after love down-regulation. It may be that love down-regulation by focusing on negative aspects of the partner or the relationship or imagining negative future scenarios makes people feel bad because it involves negative thoughts. Although the current study did not study the long-term effects of love down-regulation using reappraisal, it has recently been shown that thinking negative thoughts about the relationship has adaptive features when recovering from a romantic break-up [ 75 ]. So, it is important to investigate both the short- and the long-term effects of love regulation, as those may be dissociated.
Love up-regulation resulted in decreased positive affect in participants who were in a relationship, which was unexpected. This may have occurred because of the effort it takes to apply cognitive reappraisal [ 18 ]. It could be that people who are in a happy relationship (as indicated by self-reported relationship quality) may prefer to just look at their partner, rather than to have to come up with positive aspects of the partner or the relationship, or positive future scenarios on demand. We did not test the long-term effects of love regulation, but it might be that even though it may be cumbersome at this moment to use reappraisal to up-regulate love feelings, it may have beneficial long-term effects in the context of romantic relationships. Future studies are needed to replicate this unexpected effect, to determine why it occurs, to explore if and how it can be reduced, and to test if it is perhaps accompanied by an advantageous long-term effect. Even though love up-regulation resulting in decreased positive affect in participants who were in a relationship is in contrast to the hypothesis, it does show that participants were not just regulating their emotions. In that case, love up-regulation would have resulted in more positive feelings in both groups. This suggests that it is important to distinguish between the effects of love regulation on love feelings and on affect, as a desired effect in love feelings might not result in better affect in the short run.
Love regulation did not change subjective arousal (cf. [ 76 ]. It could be that the five-point rating scale we used was too coarse to detect any changes in arousal due to love regulation. It may be better to use a finer scale in future studies. Alternatively or additionally, recent work has shown that reappraising anxiety as excitement (i.e., changing the valence from negative to positive) improved performance in anxiety-provoking tasks compared to trying to calm down (i.e., reducing arousal) [ 77 ], so it may be more beneficial to change valence rather than arousal when regulating love feelings. More research is needed to test this suggestion.
Unlike the self-reported infatuation and attachment levels, the LPP amplitude is not a direct measure of love intensity. The advantage of the LPP amplitude over self-reported feelings is that it is not susceptible to social desirability biases and demand characteristics. Because the LPP amplitude is typically enhanced in response to both positive and negative stimuli, the LPP does not reflect whether a stimulus elicits positive or negative feelings. Instead, the LPP amplitude has been used as an objective measure of regulation success [ 19 ] because it reflects the affective and motivational significance of a stimulus and the resulting motivated attention instead [ 42 ]. So, the LPP amplitude in response to a picture of the partner indicates how emotionally or motivationally significant the partner is and how much attention is being paid to him/her. The instruction to up-regulate love feelings resulted in a more positive ERP between 300–400 ms (cf. [ 27 ]. The latency and the midline centroparietal topography of this regulation effect confirms that regulation instructions modulated the LPP component [ 42 ]. The enhanced LPP indicates that love up-regulation enhances the affective and motivational significance of, and the resulting motivated attention to the (ex-)partner. Because stronger love feelings would result in enhanced significance of the partner, the enhanced LPP with love up-regulation corroborates the self-report finding that people are able to up-regulate their love feelings deliberately.
Love down-regulation decreased the LPP amplitude between 700–3000 ms in participants who were in a romantic relationship, which indicates that love down-regulation reduced the affective and motivational significance of, and the resulting motivated attention to the partner. Because weaker love feelings would result in reduced significance of the partner, the reduced LPP with love down-regulation corroborates the self-report finding that people are able to down-regulate their love feelings deliberately. It is important to note that the ERP reflects brain activation elicited by events, which are the presentations of partner and neutral pictures in this case. A reduced LPP amplitude by down-regulation is therefore not at odds with the increased self-reported negative affect at the end of the down-regulation block. That is, a reduced affective and motivational significance of, and motivated attention to the partner pictures (as reflected by the LPP amplitude) may very well be accompanied by an increase in general negative affect that is not linked to the 3-sec presentation of a picture and will therefore not be reflected in the ERP (e.g., because the baseline correction removed the effect). It is interesting that the down-regulation effect occurred a few hundred milliseconds later than the up-regulation effect (cf. [ 78 ]), which suggests that love down-regulation takes more time to take effect than love up-regulation. The down-regulation effect in the LPP amplitude did not reach significance in participants that had experienced a break-up, which is ironic because love down-regulation might benefit them more than people who are in a happy relationship. Greater interindividual variation is the likely cause of the down-regulation effect not being significant in the break-up group. This variation may have been due to the break-up group being rather heterogeneous in terms of time since break-up, intensity of love feelings for the ex-partner, and levels of positive and negative affect, since factors like these may affect love down-regulation success.
In contrast to the hypotheses, and to the notion that the LPP amplitude is modulated by regulation instruction according to the regulatory goal [ 19 ], the LPP amplitude was numerically, but not significantly, enhanced for down-regulation between 300–400 ms in both groups, and significantly reduced for up-regulation between 700–3000 ms in participants who were in a romantic relationship. Interpreting the LPP amplitude as reflecting the affective and motivational significance of, and the resulting motivated attention to a stimulus [ 42 ], the significantly reduced LPP amplitude for up-regulation between 700–3000 ms in participants who were in a romantic relationship suggests that, even though up-regulation initially (i.e., between 300–400 ms) increases the significance of, and attention to a current partner, it reduces it eventually (i.e., after 700 ms). Interestingly, the up-regulation effect in the LPP amplitude between 700–1000 ms showed significant individual differences. Even though the LPP was reduced by love up-regulation at the group level, participants who actually showed a more enhanced LPP amplitude as a result of love up-regulation in this time window also showed a greater decrease in negative affect as a result of love up-regulation. Because correlation does not imply causation, this effect could be interpreted in several ways. It might be that love up-regulation only leads to a reduction in negative affect when it is successful (as indicated by an enhanced LPP). Future research will need to replicate this effect and clarify its interpretation.
The unexpected LPP findings challenge the interpretation of the regulation effects in the LPP amplitude. It is important to note that the observed pattern resembles some previous emotion regulation studies that have revealed numerically or significantly enhanced LPP amplitudes for down-regulation [ 27 , 48 , 57 , 76 ] and numerically reduced LPP amplitudes for up-regulation [ 46 ] as well. There are several potential factors that could have caused these unexpected effects in the current and previous studies, such floor and ceiling effects [ 27 , 46 , 48 ], presentation of regulation instructions in a blocked rather than an intermixed fashion [ 47 , 78 ], letting participants choose between different regulation strategies [ 57 ], or switching between up- and down-regulation. More research is needed to systematically test these and other factors to better understand the effects of regulation task characteristics on the LPP amplitude. For example, the first author is currently working on studies testing whether floor and ceiling effects cause the unexpected effects of emotion regulation instructions on the LPP. In addition, future studies could directly compare the effects of presentation of regulation instructions in a blocked versus an intermixed fashion, and the effects of letting participants choose between different regulation strategies versus instructing them to use one particular strategy. In addition, it would be informative to compare the effects of having participants perform both up- and down-regulation in a testing session versus only one of the two. Studies like those will provide more information about what exactly the LPP amplitude reflects in regulation tasks. Depending on the conclusions of those studies, the LPP amplitude may or may not have limited usability as a measure of regulation success. Alternative measures that could have merit as an objective measure of love regulation success in future studies are behavioral measures, skin conductance, heartbeat-related measures [ 79 ], facial electromyography [ 80 ], and activation of brain regions that have been associated with love [ 81 ].
To conclude, to the best of our knowledge, this is the first study concerning explicit regulation of love feelings. We argue that love regulation targets actual love feelings and we recognize that that in turn may affect emotions and relationship characteristics. The results showed that people have the preconception that love is somewhat uncontrollable. Nevertheless, they use various behavioral and cognitive strategies to cope with romantic break-ups and to maintain long-term relationships. In the context of heartbreak, distraction was used to feel better after a break-up (i.e., emotion regulation), while reappraisal was used to down-regulate love feelings. In the context of long-term relationships, communication/honesty was important for maintaining long-term relationships, while undertaking (new) activities with the beloved was used to prevent love feelings from declining (i.e., love up-regulation). These preconceptions of, and strategies for love regulation were replicated in two independent samples. Importantly, people were able to up-regulate their love feelings by thinking about the positive aspects of their partner and/or relationship and imagining positive future scenarios. People were also able to down-regulate their love feelings by thinking about negative aspects of their partner and/or relationship and imagining negative future scenarios.
This study, being the first of its kind, provides many suggestions for future research. In this study, we only tested the short-term effects of love regulation. For daily life applicability, it would of course be important that the effects of love regulation are long-lived and/or that people are able to perform love regulation habitually to obtain a sustained effect. Therefore, future studies should examine the long-term effects of love regulation, including its effects on well-being and relationship stability and satisfaction, as well as ways in which love regulation can become habitual. It would also be interesting to examine the effectiveness of behavioral and cognitive strategies other than reappraisal for regulating love feelings, including distraction, avoidance, and undertaking (new) activities with the beloved. In addition, it is important dissociate the effects of love regulation on love feelings and on affect, as a desirable effect on love feelings may be accompanied by an undesirable effect on affect, or vice versa. Love up- and down-regulation have numerous applications, ranging from stabilizing long-term relationships including marriages, reducing heartbreak after romantic break-ups, ameliorating unwanted crushes and forbidden loves, and perhaps even coping with the death of a beloved. In short, love regulation may increase the positive effects and decrease the negative effects of love on individuals and on society and therefore deserves much attention from the scientific community.
Supporting Information
S1 appendix. questions about perceived control over love feelings..
https://doi.org/10.1371/journal.pone.0161087.s001
S1 Text. Neutral IAPS pictures.
https://doi.org/10.1371/journal.pone.0161087.s002
Acknowledgments
We thank Annemieke van Arum, Mandy van Dijk, Liesbeth Janssen, and Ginger Sassen for help with the data collection.
Author Contributions
- Conceptualization: SJEL JWvS.
- Formal analysis: SJEL.
- Investigation: JWvS.
- Methodology: SJEL JWvS.
- Resources: JWvS.
- Software: SJEL.
- Supervision: JWvS.
- Visualization: SJEL.
- Writing - original draft: SJEL.
- Writing - review & editing: SJEL JWvS.
- 1. Carver K, Joyner K, Udry JR. National estimates of adolescent romantic relationships. In: Florsheim P, editor. Adolescent Romantic Relations and Sexual Behavior: Theory, Research, and Practical Implications Mahwah, NJ: Lawrence Erlbaum Associates Publishers 2003. p. 23–56.
- View Article
- PubMed/NCBI
- Google Scholar
- 6. Leary MR, Koch EJ, Hechenbleikner NR. Emotional responses to interpersonal rejection. In: Leary M, editor. Interpersonal rejection. Oxford: Oxford University Press; 2001. p. 145–66.
- 12. Hatfield E. Passionate and companionate love. In: Sternberg RJ, Barnes ML, editors. The psychology of love. New Haven, CT: Yale University Press; 1988. p. 191–217.
- 17. Grant Thornton. For richer, for poorer? What’s yours is mine, and what’s mine is out of sight UK: 2012.
- 36. Vangelisti AL. Interpersonal processes in romantic relationships. In: Knapp ML, Daly JA, editors. The SAGE handbook of interpersonal communication2012. p. 597–631.
- 39. Barker C, Pistrang N, Elliott R. Research methods in clinical psychology: An introduction for students and practicioners. 2nd ed. Chichester, UK: Wiley; 2002.
- 41. Stone AA, Turkkan JS, Bachrach CA, Jobe JB, Kurtzman HS, Cain VS. The science of self-report : Implications for research and practice . Mahwah, NJ: Lawrence Erlbaum Associates; 2009.
- 50. Hatfield E. The passionate love scale. In: Davis CM, Yarber WL, Bauserman R, Schreer G, Davis SL, editors. Handbook of Sexuality-Related Measures. Thousand Oaks Sage Publications; 1998. p. 449–51.
- 53. Lang PJ, Bradley MM, Cuthbert BN. International affective picture system (IAPS): Digitized photographs, instruction manual and affective ratings Tech. Rep. No. A-6 ed. Gainsville, FL: University of Florida; 2005.
- 59. Rugg MD, Allan K. Memory retrieval: An electrophysiological perspective. In: Gazzaniga MS, editor. The New Cognitive Neurosciences. Cambridge: The MIT Press 2000.
- 76. Langeslag SJE. The effect of arousal on regulation of negative emotions using cognitive reappraisal: An ERP study. under review.
Academia.edu no longer supports Internet Explorer.
To browse Academia.edu and the wider internet faster and more securely, please take a few seconds to upgrade your browser .
Enter the email address you signed up with and we'll email you a reset link.
- We're Hiring!
- Help Center

The Effects of Romantic Relationships on the Academic Performance of University of the Philippines – Cebu College Students ACKNOWLEDGMENTS

Related Papers
Jedh Esterninos
ABSTRACT The study focused on the Academic Performance and the Married students. The researcher used the method of triangulation – Using Questionnaires, Focus group discussion, and Interviews. The objectives of the study are to present the level of academic performances of married students and their personalities. To determine the difficulties encountered by the married students and to identify strategies mechanized by the married students in accomplishing their studies. Using the data gathered, Answers from the questionnaires, suggestions and ideas from the respondents during the interviews. The researcher arrives at the findings, conclusion and recommendations of the study. To make this study fruitful and give benefits to the community specifically to the respondents – who are married students. The researcher recommends to the Local government, to the University, to the teachers, to the parents and to the students. The study also finds out some of the strategies of the married students in performing well in academic performance, give a tip on how the family time are balance, how their studies positively affect their children’s attitude towards education. And also the research inspires to give importance to pursuing the education. The research truly shows the current level of academic performance of the married students. The researcher also correlates the grades of Married students to their personality which results to low correlation, which makes the research interesting to finds out why. The researcher finds it out during the interviews – “That almost married students has a good personality and it is not affected by their grades or vice-versa, they just wanted to finish their study not worrying of getting high grades. But as the researcher finds out, some of them are excellent in academic performance. As the reader studies this research, They will discover it interesting and worth it to study this kind of research.
shiv juneja
Hypothesis-Being in a committed relationship in high school results in lower academic performance. Conceptualisation of Hypothesis: In today's world more than half of high school students have been in relationships and most of graduates too. Today people do prefer to form committed relationships later on in life and prioritise well, focusing on their education. However some do feel that they can be in a committed relationship and at the same time do their best in other spheres of life. We, are trying to prove that these people who are in committed relationships are not living upto their potential and would be better off without a relationship. Other tests in particular the one done by StudyMode shows that more than half of those children who have mobile phones in school text their partner during classes, a tenth email their partner and 41% even say that they've skipped class before to be with their significant other. All these facts are reinstating our belief that students get distracted by their significant others. Well in our minds a committed relationship is one where both partners are emotionally attached and have been emotionally invested in there significant other for over 2-3 months(includes before getting into the relationship). They depend on each other for stability in their lives. As we need to make sure we get accurate results. We would also like to make clear what we mean by terms such as emotional stability and their relations to relationships. Irrational thinking, impulsiveness and a fluctuating level of happiness are the three things one can notice in those who are emotionally unstable. This aspect comes into context as when committed partners start causing one to think irrationally or be impulsive about matters concerning their partners. These people can be easily affected and distracted by even the littlest things in their relationship and unable to focus while going through a rough patch. They start to depend on their partners to keep up a certain level of emotional balance. We sense this is not only distracting one away from paying attention in class but limiting their ability to do work and the quality of their work when under stress and emotional imbalance. Academic performance and what effects it: to reach optimum academic performance a work ethic and an intellectually advanced brain is not all that is required to excel. We believe one must have 2 non school hours dedicated to homework and self study or tuition in some cases. We believe one must get enough rest, 7-8 hours of sleep and maintain a healthy body. One must not feel emotionally or socially neglected by family or friends as anything that can effect one's behaviour and thought processes negatively in school or at home, can effect the quality of the work they put in towards academics. Our third point shows us exactly why the effects of relationships can be harmful to academic performances. Our friends from other schools and our classmates as well have all had changes in their life whether minute or large upon getting in relationships. By trying to prove our hypothesis we will show how these changes in their life have effected academic performance. All aspects that affect academic performance will be analysed after the survey to prove our hypothesis.
Renalyn Pradilla
Sean Natividad
Aica Solon II
Flor Opsima
International journal of humanities and social sciences
Zahra Dasht Bozorgi
This study investigated the relationship between love styles, personality traits and quality of life of the married students. Statistical population consists of all married students of Islamic Azad University of Qom, of whom, 200 subjects were selected using the stepwise cluster random sampling. The research instrument included Love Attitudes Scale of Hendrick & Hendrick (1986), NEO Personality Inventory (1985) and Dyadic Adjustment Scale by Spanier (1976). The results of data analysis using the Pearson correlation coefficient showed a significant relationship between the love styles, personality traits, and quality of marital life. Results of the regression analysis also showed that variables of conscientiousness, extroversion, EROS love style , agreeableness, STORGE love style, and openness are good predictors for criterion variable of the quality of marital life.
The Eurasia Proceedings of Educational and Social Sciences
Tolga Erdogan
Marj Florentino
This study is focused on the social factors that affect the academic performance of the first year College of Education students in the Polytechnic University of the Philippines, particularly the campus organizations, sports activities, and romantic relationships. The researchers wanted to know the perception of the students on these factors and how does it affect their academic performance.
Loading Preview
Sorry, preview is currently unavailable. You can download the paper by clicking the button above.
RELATED PAPERS
Archives of Business Research
Benjamin Omolayo
Procedia - Social and Behavioral Sciences
Mary N N E K A Nwikpo
Gholam Ali Afrooz
Abdullahi umar
Jurnal Bimbingan dan Konseling Islam
Sri Sofiana Amni
Ijrdt Journal
International Journal of Management, Technology, and Social Sciences (IJMTS)
Dr. Gururaj Itagi
Titilola Adebowale
Academic achievement of higher secondary school students in relation to their family relationship
Dr. NISAR A H M A D KUMAR
Psychological Applications and Trends 2019
GUIDANCE OFFICE
Humberto Bravo
European Academic research
Mukhtar Barnoma
University Of Saint Louis- Tuguegarao
Rowell Bustillo
Indian Journal of Applied Research
minoo chehrzad
Cyreanth Trujulan
Abdullah Al Zabir , Asif Mahmud
Arul Lawrence A S
The Journal of Social Sciences Research
President Ramon Magsaysay State University
ilknur avci
Mediterranean Journal of Humanities
Edina Ajanovic
Iranian journal of nursing and midwifery research
hasan ashrafi rizi
Tilamsik: The Southern Luzon Journal of Arts and Sciences
Marissa Cadao-Esperal , Tilamsik: The Southern Luzon Journal of Arts and Sciences
Amelia Imanda
RELATED TOPICS
- We're Hiring!
- Help Center
- Find new research papers in:
- Health Sciences
- Earth Sciences
- Cognitive Science
- Mathematics
- Computer Science
- Academia ©2024
- DOI: 10.36948/ijfmr.2024.v06i02.15753
- Corpus ID: 268822827
Exploring the Impact of Ai on Architectural Creativity and Efficiency
- Noor Afshan , Ar. Sameer Sharma
- Published in International Journal For… 31 March 2024
- Engineering
2 References
Researchgate, related papers.
Showing 1 through 3 of 0 Related Papers
An official website of the United States government
The .gov means it’s official. Federal government websites often end in .gov or .mil. Before sharing sensitive information, make sure you’re on a federal government site.
The site is secure. The https:// ensures that you are connecting to the official website and that any information you provide is encrypted and transmitted securely.
- Publications
- Account settings
Preview improvements coming to the PMC website in October 2024. Learn More or Try it out now .
- Advanced Search
- Journal List
- PMC11335839

Drug–Drug Interactions Involving High-Alert Medications that Lead to Interaction-Associated Symptoms in Pediatric Intensive Care Patients: A Retrospective Study
Lisa marie kiesel.
1 Clinical Pharmacy, Institute of Pharmacy, Medical Faculty, Leipzig University, and Drug Safety Center, Leipzig University and Leipzig University Hospital, Leipzig, Germany
Astrid Bertsche
2 Division of Neuropediatrics, University Hospital for Children and Adolescents, Greifswald, Germany
3 Center for Pediatric Research, University Hospital for Children and Adolescents, Leipzig, Germany
Wieland Kiess
Manuela siekmeyer, thilo bertsche, martina patrizia neininger, associated data.
Children treated in a pediatric intensive care unit (PICU) often receive several drugs together, among them drugs defined as high-alert medications (HAMs). Those drugs carry a high risk of causing patient harm, for example, due to a higher potential for interactions. HAMs should therefore be administered with caution, especially in a PICU.
The objective of the current study was to identify drug–drug interactions involving HAMs that increase the risk of interaction-associated symptoms in pediatric intensive care.
In a retrospective study, we analyzed the electronic documentation of patients hospitalized for at least 48 h in a general PICU who received at least two different drugs within a 24-h interval. We assessed potential drug–drug interactions involving HAM on the basis of the two drug information databases UpToDate and drugs.com. Furthermore, we analyzed whether symptoms were observed after the administration of drug pairs that could lead to interaction-associated symptoms. For drug pairs involving HAM administered on at least 2% of patient days, and symptoms observed at least ten times after a respective drug pair, we calculated odds ratios, 95% confidence intervals, and p -values by using a univariate binary logistic regression.
Among 315 analyzed patients, 81.3% (256/315) received drugs defined as high-alert medication for pediatric patients. Those high-alert medications were involved in 20,150 potential drug–drug interactions. In 14.0% (2830/20,150) of these, one or more symptoms were observed that could be a possible consequence of the interaction, resulting in 3203 observed symptoms affecting 56.3% (144/256) of patients receiving high-alert medication. The odds ratios for symptoms observed after a drug–drug interaction were increased for eight specific symptoms (each p ≤ 0.05), especially hemodynamic alterations and disturbances of electrolyte and fluid balance. The odds ratio was highest for decreased blood pressure observed after the administration of the drug pair fentanyl and furosemide (OR 5.06; 95% confidence interval 3.5–7.4; p < 0.001). Increased odds ratios for specific symptoms observed after drug–drug interactions resulted from eight combinations composed of eight different drugs: digoxin, fentanyl, midazolam, phenobarbital, potassium salts and vancomycin (high-alert medications), and the diuretics furosemide and hydrochlorothiazide (non-high-alert medications). The resulting drug pairs were: potassium salts–furosemide, fentanyl–furosemide, vancomycin–furosemide, digoxin–furosemide, digoxin–hydrochlorothiazide, fentanyl–phenobarbital, potassium salts–hydrochlorothiazide, and midazolam–hydrochlorothiazide.
Conclusions
In a cohort of PICU patients, this study identified eight specific drug pairs involving high-alert medications that may increase the risk of interaction-associated symptoms, mainly hemodynamic alterations and electrolyte/fluid balance disturbances. If the administration of those drug pairs is unavoidable, patients should be closely monitored.
Supplementary Information
The online version contains supplementary material available at 10.1007/s40272-024-00641-x.
| More than half of the patients receiving high-alert medications were affected by a total of 3203 symptoms observed after drug–drug interactions involving high-alert medications. More than one in four observed symptoms were associated with a drug–drug interaction at a significant odds ratio. |
| Specific drug pairs were identified that may increase the risk of interaction-associated symptoms, mainly categorized as hemodynamic alterations and fluid and electrolyte balance disturbances. Those drug pairs involved eight drugs frequently administered in a PICU. |
| Physicians should avoid the administration of these specific drug pairs, or if their administration is unavoidable, monitor patients closely for corresponding symptoms. |
Introduction
Children admitted to a pediatric intensive care unit (PICU) are often in a critical state of health and require complex drug treatment. Although administration of multiple drugs together leads to an increased risk of drug-related problems [ 1 , 2 ], previous studies reported most patients in PICUs received a median number of ten different drugs per patient day [ 3 , 4 ]. Especially in the PICU, so-called high-alert medications (HAMs) must be administered frequently. Due to various factors, such as a narrow therapeutic range or a high potential for drug–drug interactions (DDIs) [ 5 , 6 ], these drugs bear a higher risk of causing patient harm compared with other drugs, according to the Institute for Safe Medication Practices (ISMP) [ 7 ]. Therefore, the administration of HAM should be given careful consideration. The ISMP developed its first list of HAMs for the acute care setting in 1995 [ 7 ]. Until now, few studies have identified specialized lists of HAM for children [ 6 , 8 – 10 ]. Schilling et al. combined results from three previous studies to develop a list of 20 HAMs for pediatric patients in the German setting. They described DDI as a drug-related problem for half of those 20 [ 6 ].
There is scant literature about DDIs involving HAMs for pediatric patients or their implications for children admitted to a PICU. Therefore, we aimed to identify DDIs involving HAMs that may increase the risk of interaction-associated symptoms. We specifically targeted drug pairs that should be avoided in daily clinical practice or closely monitored if their administration is unavoidable. We did not distinguish between different severity grades for DDI and symptoms, as we aimed to assess the most common DDIs regardless of their classification according to the databases, and we endeavored not to overlook any relevant symptoms. Therefore, we also included drug–drug interactions with a low classification according to the databases, as these can also severely affect patients in a critical health state.
Material and Methods
Study design.
This retrospective study analyzed data from April 2018 to March 2019 obtained in a general PICU of a university hospital in Germany. Patients of all pediatric age groups were treated in the study unit, except neonates, who were treated in a separate neonatal intensive care unit. We assessed the electronic documentation for each patient in the hospital’s patient data management system to identify potential DDIs (pDDIs) involving at least one drug defined as a HAM. Furthermore, we analyzed symptoms observed after these pDDIs to detect interaction-associated symptoms.
We included patients hospitalized for at least 48 h in the study unit who received at least two different drugs within a 24-h interval during their stay. Patients on chemotherapy were excluded because they were mainly treated at the pediatric oncology unit of the university hospital and only transferred to the PICU for a short time if their health condition deteriorated severely.
The study titled “Adverse drug reactions in an interdisciplinary PICU” was conducted according to the guidelines of the Declaration of Helsinki and approved by the Ethics Committee at the Medical Faculty, Leipzig University, Germany (study number: 127/19-ek) on 2 May 2019. The ethics committee waived informed consent because this was a retrospective study, and patients’ treatment was not influenced.
Identification of HAM in the PICU and pDDIs Involving at Least One HAM in Clinical Care
On the basis of the electronic patient documentation, we first examined the administration of the 20 drugs that Schilling et al. [ 6 ] defined as HAM for hospitalized pediatric patients. We included 15 of those HAMs in our analysis because 5 of the 20 defined HAMs were not administered in our PICU during the study period: cyclosporine, phenytoin, amiodarone, vecuronium, and rocuronium. Second, we evaluated pDDIs that involved at least one HAM for each patient day. For this purpose, potentially interacting drug pairs were identified on the basis of two drug information databases: UpToDate (provided by Wolters Kluwer, Riverwoods, Illinois, USA) and drugs.com (provided by Drugsite Trust, Auckland, New Zealand). Each drug pair for which an interaction alert was reported in at least one of the databases was defined as a pDDI. To identify potentially interacting drug pairs, we considered a maximum time interval of 24 h between administering a HAM and another potentially interacting drug, regardless of whether the second drug was defined as a HAM. We considered a 24-h interval to be appropriate because estimating the correct half-lives of interacting drugs in individual patients in our cohort was hardly feasible due to the general developmental variability of pharmacokinetics and pharmacodynamics in children and the possible influence of the individual patient’s condition. Hence, if a potentially interacting drug was administered 24 h before or after a HAM, the event was categorized as a pDDI. If a pDDI occurred more than once within the defined time interval, it was counted only once. For continuous infusions, it was assessed for each drug administered concurrently whether a pDDI occurred due to the additional drug.
Identification of Interaction-Associated Symptoms
For each pDDI, we investigated whether symptoms that could be associated with it were observed after the administration. For this investigation, we examined the nurses’ and physicians’ daily documentation of the patient’s condition for symptoms that occurred within a 24-hour interval after administration of the second drug of the relevant drug pair. The documentation included automatically recorded vital parameters, laboratory parameters, and additional documentation, such as non-measurable symptoms as nausea or vomiting (Online Resource 1). For vital and laboratory parameters, age-dependent standard ranges for infants, children, and adolescents were determined by the treating physicians. For some patients, the attending physician adjusted the standard ranges to the patient’s health condition. In our analyses, we considered deviations from the determined patient–individual ranges. We focused on symptoms that were identified as possible consequences of a pDDI according to our database search in UpToDate and drugs.com. If at least one of these symptoms was associated with the relevant drug pair at a statistically significant odds ratio (OR), this was defined as a DDI. Since we took the underlying data on the symptoms from the documentation of physicians and nursing staff, it can be assumed that those symptoms were clinically relevant, as they would otherwise not have been documented.
To estimate the risk associated with the interaction of a particular drug pair for an observed symptom, we calculated the OR and 95% confidence interval. To ensure that the calculation was based on a sufficient occurrence of a particular drug pair and corresponding symptom, we set two criteria. First, we only considered potentially interacting drug pairs administered on at least 2% of patient days. Second, we focused only on corresponding symptoms observed at least ten times after a given drug pair. Combining potentially interacting drug pairs and symptoms that met these criteria, we created a contingency table that presents the frequency of the following combinations on each patient day: both the potentially interacting drug pair and corresponding symptom were observed; only the potentially interacting drug pair was observed; only the symptom was observed; and neither the potentially interacting drug pair nor the symptom was observed. On the basis of the contingency table, a univariate logistic regression was performed to obtain OR, 95% confidence interval, and p -value. The calculation was conducted using IBM SPSS Statistics Version 29 (IBM Corporation, Armonk, New York, USA). A p value ≤ 0.05 was considered to indicate significance.
Characteristics of Patients and Administered Drugs
We examined 1263 patients admitted to the PICU during the study period for the inclusion criteria (Fig. (Fig.1). 1 ). Of those, 315 (24.9%) patients fulfilled the inclusion criteria. Baseline patient characteristics are presented in Table Table1. 1 . In total, 255 different drugs were administered to the patients. Of these drugs, 5.9% (15/255) were identified as HAM for hospitalized pediatric patients, according to the study by Schilling et al. [ 6 ] (Table (Table2). 2 ). The most commonly administered sedative during the study period was midazolam [affected 173/315 (54.0%) patients on 1011/3788 (26.7%) patient days; Online Resource 2]. Potassium salts were the most frequently administered HAM, used on 39.0% of patient days (1477/3788), in 47.3% (149/315) of patients (Table (Table3 3 ).

Flow chart of patient inclusion
Baseline patient characteristics
| Characteristics | Value |
|---|---|
| Number of patients, (m/f) | 315 (183/132) |
| Median age, years (Q25/Q75; min/max) | 3.7 (0.8/11.3; 0.0/22.8) |
| Median weight, kg (Q25/Q75; min/max) | 13.0 (6.7/29.0; 2.3/156.0) |
| Median length of PICU stay, days (Q25/Q75; min/max) | 8 (4/14; 3/99) |
| Median simplified acute physiology score on PICU admission (Q25/Q75; min/max) | 13 (9/21; 2/50) |
| Status of ventilation at PICU admission, (%) | |
| Not ventilated | 151 (47.9) |
| Non-invasive ventilation | 116 (36.8) |
| Invasive ventilation | 48 (15.3) |
| Death, (%) | 6 (1.9) |
| Primary reason for PICU admission, (%) | |
| Surgical | 167 (53.0) |
| Gastrointestinal | 53 (16.8) |
| Musculoskeletal | 40 (12.7) |
| Neurologic | 25 (7.9) |
| Oncologic | 23 (7.3) |
| Ears-nose-throat/maxillofacial | 13 (4.1) |
| Urologic | 7 (2.2) |
| Other | 6 (1.9) |
| Medical | 141 (44.8) |
| Respiratory | 60 (19.0) |
| Neurologic | 20 (6.3) |
| Sepsis | 15 (4.8) |
| Gastrointestinal | 13 (4.1) |
| Metabolic | 11 (3.5) |
| Cardiovascular | 5 (1.2) |
| Other | 17 (5.4) |
| Trauma | 7 (2.2) |
PICU pediatric intensive care unit
Characteristics of drug therapy
| Characteristics | Value |
|---|---|
| Total number of administered drugs, | 43,200 |
| Number of different administered drugs, | 255 |
| Median number of drugs per patient per day, (Q25/Q75; min/max) | 10 (7/15;1/34) |
| Total number of administered HAM, / (%) | 5385/43,200 (12.5) |
| Number of different administered HAM, / (%) | 15/255 (5.9) |
| Median number of HAM per patient per day, (Q25/Q75; min/max) | 1 (0/2; 0/8) |
HAM high-alert medication
Frequency of high-alert medications administered in the pediatric intensive care unit during the study period. In our analysis, we included 15 of 20 drugs defined as high-alert medications for hospitalized pediatric patients according to Schilling et al. [ 6 ]
| High-alert medication | Number of patients receiving the high-alert medication, (%) ( = 315 patients) | Number of patient days with the high-alert medication, (%) ( = 3788 patient days) |
|---|---|---|
| Potassium salts | 149 (47.3) | 1477 (39.0) |
| Midazolam | 173 (54.9) | 1011 (26.7) |
| Vancomycin | 33 (10.5) | 449 (11.9) |
| Epinephrine | 74 (23.5) | 431 (11.4) |
| Clonidine | 30 (9.5) | 415 (11.0) |
| Phenobarbital | 65 (20.6) | 405 (10.7) |
| Fentanyl | 42 (13.3) | 389 (10.3) |
| Digoxin | 14 (4.4) | 302 (8.0) |
| Amphotericin B | 13 (4.1) | 131 (3.5) |
| Tacrolimus | 12 (3.8) | 127 (3.4) |
| Propofol | 40 (12.7) | 84 (2.2) |
| Dobutamine | 7 (2.2) | 69 (1.8) |
| Norepinephrine | 18 (5.7) | 35 (0.9) |
| Morphine | 12 (3.8) | 33 (0.9) |
| Dopamine | 3 (1.0) | 27 (0.7) |
The remaining five high-alert medications were not administered during the study period: cyclosporine, phenytoin, amiodarone, vecuronium, and rocuronium
pDDIs Involving at Least One HAM
Analyzing each patient’s electronic documentation, we identified 20,150 pDDIs involving at least one HAM on the basis of our database search in UpToDate and drugs.com. We calculated a rate of 78.7 pDDIs per patient that involved at least one HAM (20,150 pDDI involving at least one HAM/256 patients receiving HAM). The 20,150 pDDIs resulted from 469 different drug pairs. Of these potentially interacting drug pairs, 14.3% (67/469) were administered on at least 2% of patient days. The frequency of the potentially interacting drug pairs and their classifications according to the databases is presented in Online Resource 3.
Interaction-Associated Symptoms Identified in the PICU
We observed at least one symptom after 14.0% (2830/20,150) of pDDIs, resulting in a total of 3203 observed symptoms affecting 56.3% (144/256) of patients receiving HAM (Table 4 ). While we observed one symptom after the administration of 87.7% (2482/2830) of those pDDIs, more than one symptom was observed after 12.3% (348/2830) of pDDIs.
Frequency of symptoms observed after potential drug–drug interactions involving high-alert medications
| Symptom | Frequency of symptoms, | Frequency related to total of symptoms, % ( = 3203) | Frequency of patients affected by the respective symptom after a pDDI involving HAM, (%) ( = 256 patients receiving HAM) |
|---|---|---|---|
| Increased heart rate | 781 | 24.4 | 62 (24.2) |
| Hyponatremia | 390 | 12.2 | 52 (20.3) |
| Vomiting | 262 | 8.2 | 41 (16.0) |
| Hypokalemia | 243 | 7.6 | 18 (7.0) |
| Decreased blood pressure | 237 | 7.4 | 28 (10.9) |
| Respiratory depression | 164 | 5.1 | 24 (9.4) |
| Urinary retention | 137 | 4.3 | 29 (11.3) |
| Hyperkalemia | 131 | 4.1 | 43 (16.8) |
| Edema | 128 | 4.0 | 13 (5.1) |
| Nausea | 119 | 3.7 | 24 (9.4) |
| Agitation | 118 | 3.7 | 21 (8.2) |
| Decreased diuresis | 112 | 3.5 | 23 (9.0) |
| Decreased heart rate | 96 | 3.0 | 10 (3.9) |
| Hypomagnesemia | 57 | 1.8 | 14 (5.5) |
| Sweating | 46 | 1.4 | 9 (3.5) |
| Hypocalcemia | 43 | 1.3 | 12 (4.7) |
| Increased blood pressure | 43 | 1.3 | 12 (4.7) |
| Fever | 19 | 0.6 | 12 (4.7) |
| Dyspnea | 14 | 0.4 | 7 (2.7) |
| Seizures | 14 | 0.4 | 5 (2.0) |
| Constipation | 10 | 0.3 | 4 (1.6) |
| Diarrhea | 9 | 0.3 | 2 (0.8) |
| Dizziness | 8 | 0.2 | 3 (1.2) |
| Abdominal pain | 5 | 0.2 | 3 (1.2) |
| Sedation | 4 | 0.1 | 1 (0.4) |
| Excessive diuresis | 3 | 0.1 | 2 (0.8) |
| Hypercalcemia | 3 | 0.1 | 2 (0.8) |
| Increased PTH | 3 | 0.1 | 1 (0.4) |
| Exanthema | 2 | 0.1 | 2 (0.8) |
| Tachypnea | 2 | 0.1 | 2 (0.8) |
HAM high-alert medication, pDDI potential drug–drug interaction, PTH parathyroid hormone
The most pDDIs after which we observed at least one symptom involved potassium salts (2.4%; 493/20,150), followed closely by digoxin (2.4%; 480/20,150) and fentanyl (2.4%; 476/20,150; Fig. Fig.2 2 ).

For each high-alert medication, the number of potential drug–drug interactions (total interactions: N = 20,150) is plotted against how often at least one symptom was observed after a potential drug–drug interaction involving the respective high-alert medication (total interactions followed by symptoms: N = 2830)
For 33.1% (1061/3203) of observed symptoms, the preconditions for the calculation of the OR were fulfilled (Table (Table5). 5 ). We found an increased OR for hyponatremia, hypokalemia, decreased blood pressure, increased heart rate, urinary retention, edema, sweating, and restlessness (each p ≤ 0.05; Table Table5). 5 ). Those eight specific symptoms accounted for 28.0% (897/3203) of all observed symptoms potentially related to DDI. These DDIs involved eight different drugs in eight different combinations. Of the eight drugs, 75% (6/8) were defined as HAM for pediatric patients: digoxin, fentanyl, midazolam, phenobarbital, potassium salts, and vancomycin. The remaining 25% (2/8) were diuretics not defined as HAM: furosemide and hydrochlorothiazide. The highest OR was found for decreased blood pressure observed after administration of the drug pair fentanyl and furosemide (OR 5.06; 95% CI 3.5–7.4; p < 0.001), followed by hypokalemia observed after administration of the drug pairs digoxin and furosemide (OR 4.16; 95% CI 3.1–5.6; p < 0.001) and digoxin and hydrochlorothiazide (OR 3.86; 95% CI 2.9–5.1; p < 0.001).
Drug–drug interactions involving high-alert medications and subsequent symptoms observed within 24 h after the administration of the respective drug–drug interaction
| pDDI | Classification | Associated symptom | Patient days with/without pDDI and symptom, | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Drug 1 | Drug 2 | UpToDate | drugs.com | pDDI | Yes | Yes | No | No | Odds ratio [95% CI] | value | |
| Symptom | Yes | No | Yes | No | |||||||
| Potassium salts | Furosemide | B | n/a | Hyponatremia | 163 | 667 | 341 | 2617 | 1.88 [1.5; 2.3] | < 0.001* | |
| Fentanyl | Furosemide | C | Moderate | Decreased blood pressure | 43 | 275 | 104 | 3366 | 5.06 [3.5; 7.4] | < 0.001* | |
| Urinary retention | 86 | 232 | 541 | 2929 | 2.01 [1.5; 2.6] | < 0.001* | |||||
| Increased heart rate | 76 | 242 | 521 | 2949 | 1.78 [1.3; 2.3] | < 0.001* | |||||
| Vancomycin | Furosemide | n/a | Moderate | Edema | 83 | 150 | 490 | 3065 | 3.46 [2.6; 4.6] | < 0.001* | |
| Decreased diuresis | 42 | 191 | 575 | 2980 | 1.14 [0.8; 1.6] | 0.459 | |||||
| Vomiting | 36 | 197 | 502 | 3053 | 1.11 [0.8; 1.6] | 0.573 | |||||
| Digoxin | Furosemide | n/a | Moderate | Hypokalemia | 89 | 134 | 523 | 3042 | 3.86 [2.9; 5.1] | < 0.001* | |
| Nausea | 10 | 213 | 177 | 3388 | 0.90 [0.5; 1.7] | 0.748 | |||||
| Increased heart rate | 35 | 188 | 562 | 3003 | 0.99 [0.7; 1.4] | 0.978 | |||||
| Hypomagnesemia | 12 | 211 | 238 | 3327 | 0.80 [0.4; 1.4] | 0.451 | |||||
| Digoxin | HCT | n/a | Moderate | Hypokalemia | 86 | 120 | 526 | 3056 | 4.16 [3.1; 5.6] | < 0.001* | |
| Increased heart rate | 29 | 177 | 568 | 3014 | 0.87 [0.6; 1.3] | 0.496 | |||||
| Fentanyl | Phenobarbital | D | Major | Restlessness | 80 | 59 | 961 | 2688 | 3.79 [2.7; 5.4] | < 0.001* | |
| Sweating | 30 | 109 | 480 | 3169 | 1.82 [1.2; 2.8] | 0.005* | |||||
| Potassium salts | HCT | B | n/a | Hyponatremia | 85 | 229 | 419 | 3055 | 2.71 [2.1; 3.5] | < 0.001* | |
| Midazolam | HCT | n/a | Moderate | Decreased blood pressure | 20 | 168 | 127 | 3473 | 3.26 [2.0; 5.3] | < 0.001* | |
| Increased heart rate | 56 | 132 | 541 | 3059 | 2.40 [1.7; 3.3] | < 0.001* | |||||
For each drug combination and observed symptom, the frequencies of patient days on which the respective potential drug–drug interaction was or was not administered and whether the symptom was observed is shown. From those numbers, the odds ratios, 95% confidence intervals, and p -values were calculated using a univariate logistic regression
HCT hydrochlorothiazide, n/a not applicable (not listed in the respective database), pDDI potential drug–drug interaction
*Significant
a Categorized as high-alert medication for hospitalized pediatric patients according to Schilling et al. [ 6 ]
b Classification used in UpToDate: “D—Consider therapy modification; C—Monitor therapy; B—No action needed. Agents may interact with each other”
c Classification used in Drugs.com: “Major—Avoid combinations; Moderate—Usually avoid combination. Use it only under special circumstances; Minor—Take steps to circumvent the interaction risk and/or establish a monitoring plan”
HAMs are Common Drugs Administered in the PICU
According to the ISMP, HAMs carry a higher risk of patient harm compared with ordinary drugs [ 7 ]. Even when used as prescribed, they significantly increase the risk of drug-related problems [ 11 ]. In our study, 81% of critically ill children received at least one drug defined as HAM for pediatric patients by Schilling et al. [ 6 ]. Potassium salts, midazolam, and vancomycin were the HAMs most frequently administered. This is in line with a previous study in a pediatric emergency setting reporting that 91% of patients were prescribed at least one HAM, with potassium salts being the most frequently administered [ 12 ].
More than 20,000 pDDIs with HAM During a 1-Year Study
It is widely known that pDDIs are highly prevalent in PICUs. They are associated with various factors, such as a high number of administered drugs, a complex chronic condition, or an increased length of hospitalization [ 4 , 13 , 14 ]. Although previous studies determined pDDI as a cause of drug-related problems with HAM for pediatric patients, there is only limited knowledge about the frequency of pDDIs in pediatric intensive care [ 6 , 8 , 10 ]. In our study, we found more than 20,000 pDDIs involving HAM in 256 pediatric patients over the 1-year study period. A previous Brazilian study of adult intensive care patients reported 846 HAM-related pDDIs in 60 patients [ 15 ]. Compared with our research, the Brazilian study reported a considerably lower rate of HAM-related pDDIs per patient (79 versus 14). Part of this difference may be explained by the fact that pediatric patients requiring intensive care are more susceptible to drug–drug interactions [ 16 ]. However, it may also be related to the fact that the Brazilian study was performed on the basis of the database Micromedex 2.0 only [ 15 ]. Several studies recommended using at least two databases to determine pDDIs in daily routine [ 17 – 19 ] . Thus, we used the two databases, UpToDate and drugs.com, to avoid underestimating any potential risks. However, since the concordance between different databases is limited, comparing various studies can be challenging [ 20 , 21 ].
Physicians Should be Aware of Interaction-Associated Symptoms
For 2830 pDDIs, we observed 3203 symptoms occurring after the administration of the potentially interacting drug pairs. More than one in four detected symptoms were eventually associated with a DDI. Those interaction-associated symptoms comprised eight specific symptoms, mainly hemodynamic alterations or electrolyte and fluid balance disturbances. These symptoms were frequently reported in previous pediatric intensive care studies [ 3 , 22 – 24 ]. The study presented here shows that DDI involving HAM should be considered a likely trigger for symptoms in addition to other factors, such as the underlying disease or non-drug treatments, such as surgeries. It can also be assumed that various factors contribute to the occurrence of a symptom. When identifying DDIs and following interaction-associated symptoms, we did not distinguish between different severity grades of DDI or symptoms, as the main aim of our study was to identify drug pairs that are frequently associated with symptoms that are considered clinically relevant by the responsible physicians and nurses. Physicians usually receive a considerable number of alerts when using a database-related interaction checker. This may quickly lead to over-alerting. Therefore, we aimed to provide physicians with a concise overview of clinically relevant DDIs that occur frequently in a PICU. Our findings could be implemented in commonly used database-related interaction checkers to draw physicians’ attention to drug pairs involving HAM that are potentially associated with an increased risk of adverse events.
We identified eight specific drug pairs composed of eight different drugs that may lead to an increased risk of interaction-associated symptoms. By calculating the OR for a DDI and a respective symptom, we took into account how often a symptom was observed on patient days when the interacting drug pair was administered compared with days when the respective drug pair was not administered. In particular, this should minimize the risk that certain combinations of DDI and symptoms are over- or underestimated. For the interaction of fentanyl and furosemide, we found the highest OR for the symptom of decreased blood pressure. Both drugs have been shown to belong to the top ten of the most frequently administered drugs and to be among the drugs most commonly involved in pDDIs in the pediatric intensive care setting [ 4 ]. In our study, DDI was associated with a potential fivefold increased risk of decreased blood pressure. The second highest OR, indicating a potential fourfold increased risk, was found for the interaction of digoxin with hydrochlorothiazide and the observed symptom of hypokalemia. Consequently, when the administration of drug pairs associated with a potentially increased risk of interaction-associated symptoms is unavoidable, patients should be closely monitored for potential symptoms.
Until now, few studies have dealt with interaction-associated symptoms in the pediatric intensive care setting [ 14 , 25 , 26 ]. One of those studies only focused on cytochrome P450-mediated drug–drug interactions [ 25 ]. Two other studies concentrated on symptoms on the basis of clinical monitoring and laboratory results, as we did in our research. Both studies also identified hemodynamic alterations and electrolyte and fluid balance disturbances as symptoms following DDIs. However, neither of those studies noted specific interactions that increased the risk of the detected symptoms [ 14 , 26 ]. Our study went one step further by revealing eight interacting drug pairs that may increase the risk of the identified interaction-associated symptoms in clinical practice. We found symptoms that are widely known to follow the respective DDI, such as the association of hyponatremia with the DDI of potassium salts and furosemide, or the increased risk for hypokalemia associated with the DDI of digoxin and furosemide. However, we also observed symptoms after a DDI that we did not expect. For example, we unexpectedly found that the DDI of fentanyl and furosemide was associated with a potential risk increase for urinary retention, or that the DDI of vancomycin and furosemide was associated with edema. Especially for symptoms that unexpectedly are observed after a specific DDI, other factors, such as the state of illness or a surgery that could also lead to the symptom, should be critically evaluated.
Limitations
Some limitations have to be considered when interpreting our study results. First of all, the relevance of some drugs administered in our study can vary in different PICUs around the world. However, the 15 drugs defined as HAM that were in the focus of our study are used in many PICUs worldwide [ 4 , 27 – 31 ].
As recommended by previous studies [ 17 – 19 ], we used two databases to prevent failure to detect interactions that could lead to interaction-associated symptoms. However, we could not identify a database specializing in DDI for pediatrics. Previous studies did not find an age-related trend in the magnitude of DDIs, although it should be noted that there are insufficient data for children under 2 years of age [ 32 , 33 ]. In addition, extrapolating data from adults to children may over- or underestimate the severity of DDIs [ 34 ]. Additionally, as most databases are limited to the information on the interactions of two drugs, potential synergistic or antagonistic effects of combinations consisting of three or more drugs might be overlooked.
Furthermore, the allowed maximum time interval of 24 h between the administration of two drugs may be too long for an interaction for some drug pairs. According to a previous review by Bakker et al., the optimal time interval would consider the half-lives of interacting drugs [ 21 ]. However, due to the developmental variability of pharmacokinetics and pharmacodynamics in children, it is very challenging to determine standardized drug half-lives in the pediatric population [ 35 ]. In addition, the individual patients’ conditions, such as renal function, can also have significant influence on drugs’ half-lives [ 36 ]. In addition, a constant plasma concentration is aimed for with many drugs, which is why a longer-lasting interaction potential can be assumed, although the half-lives of the individual drugs are varying. To ensure a standardized approach for evaluating DDI, we established a 24-h time interval as described in the review by Bakker et al. if consideration of drug half-lives is not feasible [ 21 ]. This methodological approach might potentially increase the risk of overestimation.
The retrospective design is another limitation of this study, as using nurses’ and physicians’ daily documentation entails the risk of missing data. That could lead to information bias, as the documentation was not primarily compiled to answer research questions. Consequently, using the patient documentation as data basis may have an impact on the identification of symptoms themselves, and on the observed associations between interacting drugs pairs and subsequent symptoms. Furthermore, due to the retrospective design, we could not assess whether the physicians accepted certain expectable symptoms as an inevitable consequence of the chosen drug therapy because the patient’s state of health required the administration.
In addition, it should be kept in mind that the administration of a HAM alone and the underlying disease may also increase the risk of adverse events. However, we focused on acknowledged DDIs and interaction-associated symptoms reported in established databases. We endeavored to identify symptoms prone to being associated with a DDI by calculating ORs, as those interactions potentially contribute to evoking symptoms, or to prolonging or exacerbating existing symptoms. These drug combinations should therefore be given special consideration in the routine care of critically ill pediatric patients who are already at risk.
Our study sheds light on a topic about which knowledge is limited: symptoms associated with DDIs involving HAM. We showed that pDDIs involving HAM are very common in pediatric intensive care. More than one in four observed symptoms were associated with a DDI. These symptoms were mainly disturbances of electrolyte and fluid balance and hemodynamic alterations. Focusing on drug pairs with a potentially increased risk of triggering these symptoms, we identified eight specific drug pairs composed of eight different drugs. However, administration of these drug pairs may be unavoidable. In that case, patients should be carefully monitored for electrolyte and fluid balance disturbances and hemodynamic alterations, which were observed as the most frequent interaction-associated symptoms.
Below is the link to the electronic supplementary material.
Acknowledgements
We thank all the physicians and nurses in the participating PICU for their helpful collaboration.
Declarations
Open Access funding enabled and organized by Projekt DEAL.
A. Bertsche reports grants from UCB Pharma GmbH and honoraria for speaking engagements from Biogen GmbH, Desitin Arzneimittel GmbH, Eisai GmbH, GW Pharma GmbH, Neuraxpharm GmbH, Shire/Takeda GmbH, UCB Pharma GmbH, and ViroPharma GmbH. The other authors declare they have no conflicts of interests.
The data that support the findings of this study are available on request from the corresponding author. The data are not publicly available due to ethical and privacy considerations to protect the confidentiality of patients.
The study was conducted according to the guidelines of the Declaration of Helsinki and approved by the Ethics Committee of the Medical Faculty, Leipzig University, Germany (127/19-ek). The study was performed in accordance with the ethical standards as laid down in the 1964 Declaration of Helsinki and its later amendments.
As this was a retrospective study and data were collected from patient records without any influence on patients’ treatment, the ethics committee waived informed consent.
Not applicable.
Conceptualization: Lisa Marie Kiesel and Martina Patrizia Neininger; methodology: Lisa Marie Kiesel, Martina Patrizia Neininger, Astrid Bertsche, Thilo Bertsche, Manuela Siekmeyer, and Wieland Kiess; formal analysis: Lisa Marie Kiesel; investigation: Lisa Marie Kiesel and Martina Patrizia Neininger; writing—original draft preparation: Lisa Marie Kiesel and Martina Patrizia Neininger; writing—review and editing: Astrid Bertsche, Thilo Bertsche, Manuela Siekmeyer, and Wieland Kiess; supervision: Martina Patrizia Neininger; project administration: Lisa Marie Kiesel and Martina Patrizia Neininger. All authors read and approved the final version.

IMAGES
VIDEO
COMMENTS
Behavioral systems and romantic love. 5. being loved, esteemed, and accepted by relationship partners; and optimistic beliefs about one's. ability to cope with stress and manage distress. Bowlby ...
Scholars across an array of disciplines including social psychologists have been trying to explain the meaning of love for over a century but its polysemous nature has made it difficult to fully understand. In this paper, a quadruple framework of attraction, resonance or connection, trust, and respect are proposed to explain the meaning of love ...
The questionnaire used in the present research is Sternberg's Triangular love scale (1997) which consists of 45 questions with 9 - point Likert sca les. The first 15 items in the sca le reflect
PDF | On Jan 1, 2020, Thiago de Almeida and others published The concept of love: an exploratory study with a sample of young Brazilians | Find, read and cite all the research you need on ResearchGate
Among them, the Journal of Social and Personal Relationships (400 publications, IF 2021 = 2.681) had the highest number of papers on romantic love research, followed by Personal Relationships (189 ...
Scholars across an array of disciplines including social psychologists have been trying to explain the meaning of love for over a century but its polysemous nature has made it difficult to fully understand. In this paper, a quadruple framework of attraction, resonance or connection, trust, and respect are proposed to explain the meaning of love.
Love feelings can be more intense than desired (e.g., after a break-up) or less intense than desired (e.g., in long-term relationships). If only we could control our love feelings! We present the concept of explicit love regulation, which we define as the use of behavioral and cognitive strategies to change the intensity of current feelings of romantic love. We present the first two studies on ...
Abstract. Love is a perennial topic of fascination for scholars and laypersons alike. Whereas psychological science was slow to develop active interest in love, the past few decades have seen considerable growth in research on the subject, to the point where a uniquely psychological perspective on love can be identified.
Published 1986. Psychology. Psychological Review. This article presents a triangular theory of love. According to the theory, love has three components: (a) intimacy, which encompasses the feelings of closeness, connectedness, and bondedness one experiences in loving relationships; (b) passion, which encompasses the drives that lead to romance ...
to love research in the U.S. has been more an impediment than a terminus (other countries, particularly Canada, have taken a more enlightened view, as have at least two private foundations, the Fetzer and Templeton Institutes). As we describe in the remainder of this article, the scientific study of love is alive, well, and thriving (even in ...
stablished evidence for the construct validity of the Love Language model (Chapman, 1992). Egbert and Polk (2006) found that the five fac-tors were correlated with Stafford et al. (2000) relational mainte. ance typology (i.e., assurances, social networks, openness, positivity, and shared tasks). Those who scored h.
Love is a universal emotion that has become the basis of marriage and family for many societ - ies, which researchers continue to explore. This research will add to the knowledge of interper-sonal romantic attraction, further exposing love's complex nature. Dr. Earl Naumann's (2001) survey in his book, Love at First Sight, served
Abstract. Romantic love could be considered as a collection of activities associated with the acquisition and retention of emotions needed to survive and reproduce. These emotions change the individual's behavioural strategies in a way that will increase the likelihood of achieving these goals. Love may be defined as an emergent property of an ...
As a matter of fact, the author explains how he was severely criticized by the academic community by doing a research about love because it has been seen as an unserious topic (even if love has been studied from different approaches and disciplines such as philosophy, literature, archeology, anthropology and psychology) and how revealing the ...
e ffects on personal and relational health. This article presents a review of lit-. erature regarding t he influence of th e various love styles —. identified by Lee. [1] —on quality and ...
University of Wisconsin. Address of the President at the sixty-sixth Annual Convention of the American Psychological Association, Washington, D. C., August 31, 1958. First published in American Psychologist, 13, 573-685. Love is a wondrous state, deep, tender, and rewarding. Because of its intimate and personal nature it is regarded by some as ...
3) According to Branden, this is the kind of love that brings out the very best in people. Romantic love is known by many names, "passionate love," "erotic love," "Eros," and being "in love" (Berscheid, 2010). According to Maslow love is one of four basic human needs (physiological, safety, love, and esteem).
International Journal of Research Publication and Reviews, Vol 2, no 11, pp 1264-1267, November 2021 ... The research found that romantic love, without the common obsession factor of early-stage relationships, can and does exist in long-term marriages, and is correlated to well-being, marital satisfaction, and high self-esteem. However, obsessive
The goal of this paper is to increase knowledge about the social definition of love in the context of an intimate relationship. The empirical material analyzed comes from Focus Group Interviews, Bulletin Board Discussions online, and representative research conducted using the CAWI method.
The research instrument included Love Attitudes Scale of Hendrick & Hendrick (1986), NEO Personality Inventory (1985) and Dyadic Adjustment Scale by Spanier (1976). The results of data analysis using the Pearson correlation coefficient showed a significant relationship between the love styles, personality traits, and quality of marital life.
1.9% of p articipants. The statistical analysis conducted in this study revealed that participants who preferred qualit y. time as their love language reported the highest levels of relationship ...
R Discovery powered by AI literature search, accelerates your research discovery journey, with latest and relevant content in your area of interest. Enjoy seamless research reading with R Discovery's Reading Feed, which identifies articles based on your interests and delivers personalized recommendations in a simple social media style.
Last March, Ristroph and Purdue PhD student Luiza Stolte Bezerra Lisboa Oliveira published a critical review of the research literature on the Uptake and Translocation of Organic Nanodelivery Vehicles in Plants in Environmental Science and Technology.
London: Trent focus group. 5_Introduction-to-qualitative-research-2009-libre.pdf (d1wqtxts1xzle7.cloudfront.net). Google Scholar Harazni L, Alkaissi A (2015) The experiences of mothers and teachers of attention deficit/hyperactivity disorder children, and their management practices for the behaviors of the child a descriptive phenomenological ...
PDF | Romantic love has been explored for centuries revealing multiple emotions and feelings related to this phenomenon. Romantic relationship, a... | Find, read and cite all the research you need ...
Abstract Artificial intelligence (AI) is revolutionizing the architectural industry, enhancing both creativity and efficiency. This study explores AI's impact on construction practice, aiming to clarify its role in enhancing creative efficiency and streamlining operations. Through a literature review, it examines AI's transformative effects on design processes and key tools for integration ...
Supplementary file1 (PDF 505 KB) 40272_2024_641_MOESM1_ESM.pdf (505K) GUID: 9CD2B7C8-2BE4-4F3F-BAF7-1ED7D07657BC. Abstract. Background. ... That could lead to information bias, as the documentation was not primarily compiled to answer research questions. Consequently, using the patient documentation as data basis may have an impact on the ...
Download full-text PDF Read full-text. ... In this paper, we focus on the love styles and components of love in 106 psychology students aged 19-55 years. ... The research aimed to analyze the love ...